Association of Early and Late Hospital Readmissions with a Novel Housing-Based Socioeconomic Measure
- PMID: 35769114
- PMCID: PMC9234927
- DOI: 10.1177/23333928221104644
Association of Early and Late Hospital Readmissions with a Novel Housing-Based Socioeconomic Measure
Abstract
Background: While socioeconomic status has been linked to hospital readmissions for several conditions, reliable measures of individual socioeconomic status are often not available. HOUSES, a new measure of individual socioeconomic status based upon objective public data about one's housing unit, is inversely associated with overall hospitalization rate but it has not been studied with respect to readmissions.
Purpose: To determine if patients in the lowest HOUSES quartile are more likely to be readmitted within 30 days (short-term) and 180 days (long-term).
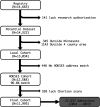
Methods: A retrospective cohort study of 11 993 patients having 21 633 admissions was conducted using generalized linear mixed-effects models.
Results: HOUSES quartile did not show any significant association with early readmission. However, when compared to the lowest HOUSES quartile, the second quartile (OR = 0.90, 95%CI 0.83-0.98) and the third quartile (OR = 0.91, 95%CI 0.83-0.99) were associated with lower odds of late readmission while the highest quartile (OR = 0.91, 95%CI 0.82-1.01) was not statistically different.
Conclusion: HOUSES was associated with late readmission, but not early readmission. This may be because early readmissions are influenced by medical conditions and hospital care while late readmissions are influenced by ambulatory care and home-based factors. Since HOUSES relies on public county assessor data, it is generally available and may be used to focus interventions on those at highest risk for late readmission.
Keywords: health outcomes; hospital readmission; managerial epidemiology; medical informatics; social determents of health.
© The Author(s) 2022.
Conflict of interest statement
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
Similar articles
-
An Innovative Individual-Level Socioeconomic Measure Predicts Critical Care Outcomes in Older Adults: A Population-Based Study.J Intensive Care Med. 2021 Jul;36(7):828-837. doi: 10.1177/0885066620931020. Epub 2020 Jun 25. J Intensive Care Med. 2021. PMID: 32583721 Free PMC article.
-
Risk Factors, Causes, and Costs of Hospital Readmission After Head and Neck Cancer Surgery Reconstruction.JAMA Facial Plast Surg. 2019 Mar 1;21(2):137-145. doi: 10.1001/jamafacial.2018.1197. JAMA Facial Plast Surg. 2019. PMID: 30418467 Free PMC article.
-
Association of a housing based individual socioeconomic status measure with diabetic control in primary care practices.Prim Care Diabetes. 2022 Feb;16(1):78-83. doi: 10.1016/j.pcd.2021.10.001. Epub 2021 Nov 19. Prim Care Diabetes. 2022. PMID: 34802978
-
Lower household income is associated with an increased risk of hospital readmission in patients with decompensated cirrhosis.J Gastroenterol Hepatol. 2021 Apr;36(4):1088-1094. doi: 10.1111/jgh.15153. Epub 2020 Jul 14. J Gastroenterol Hepatol. 2021. PMID: 32562577 Free PMC article.
-
A novel housing-based socioeconomic measure predicts hospitalisation and multiple chronic conditions in a community population.J Epidemiol Community Health. 2016 Mar;70(3):286-91. doi: 10.1136/jech-2015-205925. Epub 2015 Oct 12. J Epidemiol Community Health. 2016. PMID: 26458399 Free PMC article.
References
-
- Bailey M, Weiss A, Barrett M, Jiang H. Characteristics of 30-Day Readmissions, 2010-2016. Vol HCUP Statistical Brief #248. Rockville, MD: Agency for Healthcare Research and Quality; 2019. - PubMed
-
- Ashton CM, Kuykendall DH, Johnson ML, Wray NP, Wu L. The association between the quality of inpatient care and early readmission. Ann Intern Med. 1995;122(6):415-421. - PubMed
-
- Halfon P, Eggli Y, Pretre-Rohrbach I, Meylan D, Marazzi A, Burnand B. Validation of the potentially avoidable hospital readmission rate as a routine indicator of the quality of hospital care. Med Care. 2006;44(11):972-981. - PubMed
-
- Coleman EA, Parry C, Chalmers S, Min SJ. The care transitions intervention: results of a randomized controlled trial. Arch Intern Med. 2006;166(17):1822-1828. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources