Acute allograft dysfunction mimicking thrombotic microangiopathy in kidney transplant recipient with renal infarction: case report and review of literatures
- PMID: 35770103
- PMCID: PMC9187041
- DOI: 10.4285/kjt.20.0034
Acute allograft dysfunction mimicking thrombotic microangiopathy in kidney transplant recipient with renal infarction: case report and review of literatures
Abstract
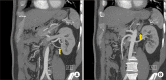
Acute allograft dysfunction is rarely observed in kidney transplantation (KT). We report an unusual case of acute allograft dysfunction mimicking thrombotic microangiopathy (TMA) in recipient with renal infarction. A 65-year-old man underwent KT from his 39-year-old son. Pre-transplant donor evaluation was normal except for the branches of the upper and lower pole renal arteries originating from the aorta in renal computed topographic angiography, respectively. The immediate post-transplant clinical course was uneventful, but serum creatinine (SCr) increased from 2.2 to 4.5 mg/dL, anemia and thrombocytopenia were shown, and serum lactate dehydrogenase increased to 919 U/L on the third day after transplantation. We suspected TMA, because of no evidence of acute bleeding. The laboratory parameters associated with TMA were within normal ranges. Renal magnetic resonance angiography revealed a focal wedge-shaped perfusion defect in the upper pole of the graft and renal Doppler ultrasonography showed decreased perfusion of the lower pole of the graft. Graft function improved with conservative therapy. The patient was discharged with SCr of 1.21 mg/dL. Graft function has been stable after discharge. Acute allograft infarction should be considered in the differential diagnosis of acute allograft dysfunction mimicking TMA in recipients with grafts supplied by multiple renal arteries.
Keywords: Kidney transplantation; Primary graft dysfunction; Thrombotic microangiopathy.
Copyright © 2020 The Korean Society for Transplantation.
Conflict of interest statement
Conflict of Interest Chul Woo Yang is an editorial board member of the journal but did not involve in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported.
Figures

References
Publication types
LinkOut - more resources
Full Text Sources

