Dynamic Regulatory Processes in the Transition From Suicidal Ideation to Action in Adults Leaving Inpatient Psychiatric Care: Protocol for an Intensive Longitudinal Study
- PMID: 35771618
- PMCID: PMC9284352
- DOI: 10.2196/38582
Dynamic Regulatory Processes in the Transition From Suicidal Ideation to Action in Adults Leaving Inpatient Psychiatric Care: Protocol for an Intensive Longitudinal Study
Abstract
Background: US suicide rates have risen steadily in the past decade, and suicide risk is especially high in the months after discharge from inpatient psychiatric treatment. However, suicide research has lagged in examining dynamic within-person processes that contribute to risk over time among individuals known to be at high risk of suicide. Almost no research has examined how affective, cognitive, and physiological processes change over minutes, hours, or days to confer risk of suicidal behavior in daily life.
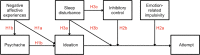
Objective: This protocol describes a longitudinal study designed to examine real-world changes in risk of suicide across multiple assessment domains. Specifically, the study involves following adults known to be at high risk of suicide after discharge from inpatient psychiatric care using self-report, interview, actigraphy, and behavioral methods to identify proximal contributors to suicidal thoughts and behaviors. First, we hypothesize that negative affective experiences, which are featured in most major suicide theories, will comprise a latent factor indicative of psychache (emotional pain), which will predict increases in suicidal thinking over time. Second, we hypothesize that poor inhibitory control in the context of negative affective stimuli, as well as emotion-related impulsivity, will predict the transition from suicidal thinking to suicidal behavior over time. Third, we hypothesize that short sleep duration will precede within-person increases in suicidal ideation as well as increased odds of suicidal behavior among those reporting suicidal thoughts.
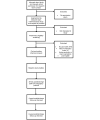
Methods: The desired sample size is 130 adults with past-week suicidal thoughts or behaviors who are receiving inpatient psychiatric treatment. Participants will complete a battery of measures while on the inpatient unit to assess negative affective experiences, emotion-related impulsivity, inhibitory control, typical sleep patterns, and relevant covariates. After discharge from inpatient care, participants will complete 4 weeks of signal-contingent ecological momentary assessment surveys, as well as mobile behavioral measures of inhibitory control, while wearing an actigraphy device that will gather objective data on sleep. Participants will complete interviews regarding suicidal thoughts and behaviors at 4 and 8 weeks after discharge.
Results: The study was funded by the National Institutes of Health in November 2020. Recruitment began in April 2021. Data analysis will begin after completion of data collection.
Conclusions: This study will elucidate how affective, cognitive, and physiological risk factors contribute (or do not contribute) to within-person fluctuations in suicide risk in daily life, with important implications for extant theories of suicide. Of import, the examined risk factors are all modifiable; thus, the results will inform identification of key targets for just-in-time, flexible, personalized, digital interventions that can be used to decrease emotional distress and prevent suicide among those at highest risk.
International registered report identifier (irrid): DERR1-10.2196/38582.
Keywords: actigraphy; affect; cognitive control; ecological momentary assessment; impulsivity; longitudinal; sleep; suicidal behavior; suicidal ideation.
©Sarah E Victor, Kirsten Christensen, Sheri L Johnson, Jason Van Allen, Leslie A Brick. Originally published in JMIR Research Protocols (https://www.researchprotocols.org), 30.06.2022.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
Similar articles
-
A Pilot Study Using Frequent Inpatient Assessments of Suicidal Thinking to Predict Short-Term Postdischarge Suicidal Behavior.JAMA Netw Open. 2021 Mar 1;4(3):e210591. doi: 10.1001/jamanetworkopen.2021.0591. JAMA Netw Open. 2021. PMID: 33687442 Free PMC article.
-
Proximal Risk for Suicide: Protocol for an Ecological Momentary Assessment Study.JMIR Res Protoc. 2022 Jul 12;11(7):e37583. doi: 10.2196/37583. JMIR Res Protoc. 2022. PMID: 35819832 Free PMC article.
-
Real-Time Real-World Digital Monitoring of Adolescent Suicide Risk During the Six Months Following Emergency Department Discharge: Protocol for an Intensive Longitudinal Study.JMIR Res Protoc. 2023 Jun 26;12:e46464. doi: 10.2196/46464. JMIR Res Protoc. 2023. PMID: 37358906 Free PMC article.
-
Don't Miss the Moment: A Systematic Review of Ecological Momentary Assessment in Suicide Research.Front Digit Health. 2022 May 6;4:876595. doi: 10.3389/fdgth.2022.876595. eCollection 2022. Front Digit Health. 2022. PMID: 35601888 Free PMC article.
-
Prevention of suicide and attempted suicide in Denmark. Epidemiological studies of suicide and intervention studies in selected risk groups.Dan Med Bull. 2007 Nov;54(4):306-69. Dan Med Bull. 2007. PMID: 18208680 Review.
Cited by
-
A systematic review on passive sensing for the prediction of suicidal thoughts and behaviors.Npj Ment Health Res. 2024 Sep 23;3(1):42. doi: 10.1038/s44184-024-00089-4. Npj Ment Health Res. 2024. PMID: 39313519 Free PMC article.
References
-
- Hedegaard H, Curtin SC, Warner M. Suicide mortality in the United States, 1999-2017. NCHS Data Brief. 2018 Nov;(330):1–8. http://www.cdc.gov/nchs/data/databriefs/db330-h.pdf - PubMed
-
- Hirsch JK, Cukrowicz KC. Suicide in rural areas: an updated review of the literature. J Rural Ment Health. 2014;38(2):65–78. doi: 10.1037/rmh0000018. - DOI
-
- Ivey-Stephenson AZ, Crosby AE, Jack SP, Haileyesus T, Kresnow-Sedacca MJ. Suicide trends among and within urbanization levels by sex, race/ethnicity, age group, and mechanism of death - United States, 2001-2015. MMWR Surveill Summ. 2017 Oct 06;66(18):1–16. doi: 10.15585/mmwr.ss6618a1. http://europepmc.org/abstract/MED/28981481 - DOI - PMC - PubMed
-
- Chung DT, Ryan CJ, Hadzi-Pavlovic D, Singh SP, Stanton C, Large MM. Suicide rates after discharge from psychiatric facilities: a systematic review and meta-analysis. JAMA Psychiatry. 2017 Jul 01;74(7):694–702. doi: 10.1001/jamapsychiatry.2017.1044. http://europepmc.org/abstract/MED/28564699 2629522 - DOI - PMC - PubMed
-
- Olfson M, Wall M, Wang S, Crystal S, Liu SM, Gerhard T, Blanco C. Short-term suicide risk after psychiatric hospital discharge. JAMA Psychiatry. 2016 Nov 01;73(11):1119–26. doi: 10.1001/jamapsychiatry.2016.2035. http://europepmc.org/abstract/MED/27654151 2551516 - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous