Real-life short-term effectiveness of anti-osteoporotic treatments: a longitudinal cohort study
- PMID: 35784611
- PMCID: PMC9243369
- DOI: 10.1177/1759720X221105009
Real-life short-term effectiveness of anti-osteoporotic treatments: a longitudinal cohort study
Abstract
Introduction: Randomized clinical trials have shown that anti-osteoporotic treatments can increase bone mineral density (BMD) and reduce the incidence of fragility fractures. However, data on the real-life effectiveness of anti-osteoporotic medications are still scarce.
Methods: We conducted a cohort study on women at high risk of fracture. We retrieved clinical and densitometric data from the DeFRA database, which derives from the DeFRA tool, a web-based fracture risk assessment tool. Multivariable Cox regression survival models were employed to analyze the effectiveness of different anti-osteoporotic drugs on fracture. In sensitivity analyses, we conducted 1:1 propensity score matching analyses.
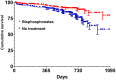
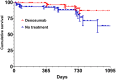
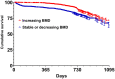
Results: Data on 50,862 women were available. Among these, 3574 individuals had at least two consecutive visits. The crude fracture rate was 91.9/1000 person-year for non-treated patients. The crude fracture rate in bisphosphonate users was 72.1/1000 person-year, in denosumab users was 58.2/1000 person-year, and in teriparatide users was 19.3/1000 person-year. Overall, we found that bisphosphonate use was associated with a 30% lower risk of fracture compared to no treatment [adjusted hazard ratio (aHR): 0.70, 95% confidence interval (CI): 0.50-0.98]. Treatment with denosumab and teriparatide were associated with 60% and 90% lower risk of fracture, respectively (aHR: 0.43, 95% CI: 0.24-0.75 and aHR: 0.09, 95% CI: 0.01-0.70). Bisphosphonate use was associated with a lower risk of fracture only after 1 year of treatment.
Conclusion: In conclusion, we found that all anti-osteoporotic medications considered in the study effectively reduced the risk of fracture in the real-life. The effect of bisphosphonate on fracture risk was apparent only after the first year of treatment. Our findings do not support the use of bisphosphonates in patients at imminent risk of fracture.
Keywords: anabolics; bisphosphonates; denosumab; osteoporosis; teriparatide.
© The Author(s), 2022.
Conflict of interest statement
Conflict of interest statement: The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: All authors have completed the ICMJE uniform disclosure form at www.icmje.org/coi_disclosure.pdf (available on request from the corresponding author) and declare no conflicts of interest. Giovanni Adami declares consultancy fee from Theramex and Galapagos outside the submitted work. Maurizio Rossini declares consultancy fees from Amgen, ABBvie, BMS, Eli Lilly, Galapagos, Novartis, Pfizer, Sandoz, Theramex and UCB outside the submitted work. All other authors declare no conflict of interest. The lead author (the manuscript’s guarantor) affirms that the manuscript is an honest, accurate, and transparent account of the study being reported; that no important aspects of the study have been omitted; and that any discrepancies from the study as planned (and, if relevant, registered) have been explained.
Figures
References
-
- Black DM, Rosen CJ. Clinical practice: postmenopausal osteoporosis. N Engl J Med 2016; 374: 254–262. - PubMed
-
- Albert SG, Wood E. Meta-analysis of clinical fracture risk reduction of antiosteoporosis drugs: direct and indirect comparisons and meta-regressions. Endocr Pract: Off J Am Coll Endocrinol Am Assoc Clin Endocrinol 2021; 27: 1082–1092. - PubMed
-
- Adami G, Giollo A, Rossini M, et al.. Different fracture risk profile in patients treated with anti-osteoporotic drugs in real-life. Reumatismo 2020; 72: 71–74. - PubMed
-
- Bouxsein ML, Eastell R, Lui L-Y, et al.. Change in bone density and reduction in fracture risk: a meta-regression of published trials. J Bone Miner Res: Off J Am Soc Bone Miner Res 2019; 34: 632–642. - PubMed
LinkOut - more resources
Full Text Sources

