British Society of Gastroenterology guidelines on the management of functional dyspepsia
- PMID: 35798375
- PMCID: PMC9380508
- DOI: 10.1136/gutjnl-2022-327737
British Society of Gastroenterology guidelines on the management of functional dyspepsia
Abstract
Functional dyspepsia (FD) is a common disorder of gut-brain interaction, affecting approximately 7% of individuals in the community, with most patients managed in primary care. The last British Society of Gastroenterology (BSG) guideline for the management of dyspepsia was published in 1996. In the interim, substantial advances have been made in understanding the complex pathophysiology of FD, and there has been a considerable amount of new evidence published concerning its diagnosis and classification, with the advent of the Rome IV criteria, and management. The primary aim of this guideline, commissioned by the BSG, is to review and summarise the current evidence to inform and guide clinical practice, by providing a practical framework for evidence-based diagnosis and treatment of patients. The approach to investigating the patient presenting with dyspepsia is discussed, and efficacy of drugs in FD summarised based on evidence derived from a comprehensive search of the medical literature, which was used to inform an update of a series of pairwise and network meta-analyses. Specific recommendations have been made according to the Grading of Recommendations Assessment, Development and Evaluation system. These provide both the strength of the recommendations and the overall quality of evidence. Finally, in this guideline, we consider novel treatments that are in development, as well as highlighting areas of unmet need and priorities for future research.
Keywords: functional dyspepsia; meta-analysis.
© Author(s) (or their employer(s)) 2022. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures

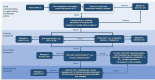
Comment in
-
Letter to the editor: Helicobacter pylori eradication - the proof is not in the symptoms.Gut. 2023 Nov 24;72(12):2387-2388. doi: 10.1136/gutjnl-2022-329057. Gut. 2023. PMID: 36379692 No abstract available.
References
-
- Walt RP, Axon ATR, Bouchier IAD, et al. Dyspepsia management guidelines. British Society of gastroenterology. Quorn Litho: Leicestershire, 1996.
-
- Howick J, Phillips B, Ball C. Oxford centre for evidence-based medicine levels of evidence University of Oxford, Centre for Evidence-Based Medicine; 2009.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
