Effect of Subanaesthetic Dose of Ketamine on Pneumoperitoneal Response and Clinical Recovery in Patients Undergoing Laparoscopy
- PMID: 35801328
- PMCID: PMC9361062
- DOI: 10.5152/TJAR.2022.21066
Effect of Subanaesthetic Dose of Ketamine on Pneumoperitoneal Response and Clinical Recovery in Patients Undergoing Laparoscopy
Abstract
Objective: Although suppression of intraperitoneal gas insufflation response is possible with a higher dose of opioids, sedatives, and inha- lational agents, delayed emergence and poor clinical recovery are still a matter of concern. Here our primary aim was to assess the quality of recovery and the secondary aim includes postinsufflation response, postoperative pain intensity, total opioid requirement, and looking for adverse effects, if any.
Methods: This prospective randomized double-blinded controlled study was conducted among 75 American Society of Anesthesiologist physical status I and II patients scheduled for laparoscopic surgeries under general anaesthesia. Group 1 received injection tramadol 1 mg kg-1 iv-1 5 minutes after intubation. Similarly, groups 2 and 3 received 0.25 mg kg-1 and 0.5 mg kg-1 injection of ketamine iv, respectively. Intraperitoneal insufflation response was observed from the beginning of insufflation till 15 minutes. Clinical recovery was measured in terms of vigilance, cognition, orientation, and comfort. Postoperative pain intensity was assessed at varying movement activities using numerical rating scale pain score and with the total opioid requirement. The collected data were analyzed using three-way ANOVA.
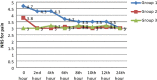
Results: Groups 1 and 2 had a fair clinical recovery. Postoperative pain intensity was least in group 2, and the postinsufflation mean arterial pressure was higher in groups 1 and 3. A total of 32% of participants had delirium in group 3.
Conclusions: Clinical recovery and perioperative analgesia were better in ketamine group (0.25 mg kg-1) without any perturbations in intra- operative pneumoperitoneal response. Hence it can be considered an optimal adjuvant in laparoscopic surgeries.
Figures
Similar articles
-
Safe and optimal pneumoperitoneal pressure for transperitoneal laparoscopic renal surgery in infant less than 10 kg, looked beyond intraoperative period: A prospective randomized study.J Pediatr Urol. 2016 Oct;12(5):281.e1-281.e7. doi: 10.1016/j.jpurol.2016.01.014. Epub 2016 Mar 4. J Pediatr Urol. 2016. PMID: 27751832 Clinical Trial.
-
Effectiveness of ondansetron as an adjunct to lidocaine intravenous regional anesthesia on tourniquet pain and postoperative pain in patients undergoing elective hand surgery: a systematic review protocol.JBI Database System Rev Implement Rep. 2015 Jan;13(1):27-38. doi: 10.11124/jbisrir-2015-1768. JBI Database System Rev Implement Rep. 2015. PMID: 26447005
-
Low-dose ketamine improves pain relief in patients receiving intravenous opioids for acute pain in the emergency department: results of a randomized, double-blind, clinical trial.Acad Emerg Med. 2014 Nov;21(11):1193-202. doi: 10.1111/acem.12510. Acad Emerg Med. 2014. PMID: 25377395 Clinical Trial.
-
Comparison of dexmedetomidine and midazolam for monitored anesthesia care combined with tramadol via patient-controlled analgesia in endoscopic nasal surgery: A prospective, randomized, double-blind, clinical study.Curr Ther Res Clin Exp. 2007 Mar;68(2):69-81. doi: 10.1016/j.curtheres.2007.04.001. Curr Ther Res Clin Exp. 2007. PMID: 24678121 Free PMC article.
-
Paravertebral anaesthesia with or without sedation versus general anaesthesia for women undergoing breast cancer surgery.Cochrane Database Syst Rev. 2021 Feb 25;2(2):CD012968. doi: 10.1002/14651858.CD012968.pub2. Cochrane Database Syst Rev. 2021. PMID: 33629404 Free PMC article.
References
-
- Das M, Ray M, Mukherjee G. Haemodynamic changes during laparoscopic cholecystectomy. Effect of clonidine premedication. Indian J Anaesth. 2007;51:205 210.
-
- Anjum N, Tabish H, Debdas S, Bani HP, Rajat C, Anjana Basu GD. Effects of dexmedetomidine and clonidine as propofol adjuvants on intra-operative hemodynamics and recovery profiles in patients undergoing laparoscopic cholecystectomy: A prospective randomized comparative study. Avicenna J Med. 2015;5(3):67 73. 10.4103/2231-0770.160231) - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources