Effects of state opioid prescribing cap laws on opioid prescribing after surgery
- PMID: 35801988
- PMCID: PMC9441291
- DOI: 10.1111/1475-6773.14023
Effects of state opioid prescribing cap laws on opioid prescribing after surgery
Abstract
Objective: To evaluate the effects of state opioid prescribing cap laws on opioid prescribing after surgery.
Data sources: OptumLabs Data Warehouse administrative claims data covering all 50 states from July 2012 through June 2019.
Study design: We included individuals from 20 states that had implemented prescribing cap laws without exemptions for postsurgical pain by June 2019 and individuals from 16 control states plus the District of Columbia. We used a difference-in-differences approach accounting for differential timing in law implementation across states to estimate the effects of state prescribing cap laws on postsurgical prescribing of opioids. Outcome measures included filling an opioid prescription within 30 days after surgery; filling opioid prescriptions of specific doses or durations; and the number, days' supply, daily dose, and pill quantity of opioid prescriptions. To assess the validity of the parallel counterfactual trends assumption, we examined differences in outcome trends between law-implementing and control states in the years preceding law implementation using an equivalence testing framework.
Data collection/extraction methods: We included the first surgery in the study period for opioid-naïve individuals undergoing one of eight common surgical procedures.
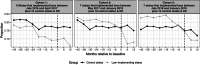
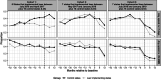
Principal findings: State prescribing cap laws were associated with 0.109 lower days' supply of postsurgical opioids on the log scale (95% Confidence Interval [CI]: -0.139, -0.080) but were not associated with the number (Average treatment effect on the treated [ATT]: -0.011; 95% CI: -0.043, 0.021) or daily dose of postsurgical opioid prescriptions (ATT: -0.013; 95% CI: -0.030, 0.005). The negative association observed between prescribing cap laws and the probability of filling a postsurgical opioid prescription (ATT: -0.041; 95% CI: -0.054, -0.028) was likely spurious, given differences between law-implementing and control states in the pre-law period.
Conclusions: Prescribing cap laws appear to have minimal effects on postsurgical opioid prescribing.
Keywords: causal inference; difference-in-differences; law; opioid; postsurgical pain.
© 2022 Health Research and Educational Trust.
Figures
Similar articles
-
Association Between State Opioid Prescribing Cap Laws and Receipt of Opioid Prescriptions Among Children and Adolescents.JAMA Health Forum. 2022 Aug 5;3(8):e222461. doi: 10.1001/jamahealthforum.2022.2461. eCollection 2022 Aug. JAMA Health Forum. 2022. PMID: 36003417 Free PMC article.
-
State prescribing cap laws' association with opioid analgesic prescribing and opioid overdose.Drug Alcohol Depend. 2022 Nov 1;240:109626. doi: 10.1016/j.drugalcdep.2022.109626. Epub 2022 Sep 10. Drug Alcohol Depend. 2022. PMID: 36115221 Free PMC article.
-
Effects of Opioid Prescribing Cap Laws on Opioid and Other Pain Treatments Among Persons with Chronic Pain.J Gen Intern Med. 2023 Mar;38(4):929-937. doi: 10.1007/s11606-022-07796-8. Epub 2022 Sep 22. J Gen Intern Med. 2023. PMID: 36138276 Free PMC article.
-
Exemptions to state laws regulating opioid prescribing for patients with cancer-related pain: A summary.Cancer. 2021 Sep 1;127(17):3137-3144. doi: 10.1002/cncr.33639. Epub 2021 May 27. Cancer. 2021. PMID: 34043811 Free PMC article. Review.
-
Laws limiting prescribing and dispensing of opioids in the United States, 1989-2019.Addiction. 2021 Jul;116(7):1817-1827. doi: 10.1111/add.15359. Epub 2021 Jan 18. Addiction. 2021. PMID: 33245795 Review.
Cited by
-
Effects of state opioid prescribing cap laws on providers' opioid prescribing patterns among patients with chronic non-cancer pain.Prev Med. 2023 Jul;172:107535. doi: 10.1016/j.ypmed.2023.107535. Epub 2023 May 5. Prev Med. 2023. PMID: 37150305 Free PMC article.
-
Trends in Opioid Prescribing and New Persistent Opioid Use After Surgery in the United States.Ann Surg. 2025 Mar 1;281(3):347-352. doi: 10.1097/SLA.0000000000006461. Epub 2024 Aug 1. Ann Surg. 2025. PMID: 39087325 Free PMC article.
-
Providing surgeons with feedback on their patients' postoperative home opioid consumption to limit postsurgical opioid prescribing and reduce unused pills: a pilot randomized clinical trial.Reg Anesth Pain Med. 2024 Oct 9:rapm-2024-105976. doi: 10.1136/rapm-2024-105976. Online ahead of print. Reg Anesth Pain Med. 2024. PMID: 39384332 No abstract available.
-
Changes in Surgical Opioid Prescribing and Patient-Reported Outcomes After Implementation of an Insurer Opioid Prescribing Limit.JAMA Health Forum. 2023 Oct 6;4(10):e233541. doi: 10.1001/jamahealthforum.2023.3541. JAMA Health Forum. 2023. PMID: 37831460 Free PMC article.
-
A Longitudinal Multivariable Analysis: State Policies and Opioid Dispensing in Medicare Beneficiaries Undergoing Surgery.J Gen Intern Med. 2024 Nov;39(15):2942-2951. doi: 10.1007/s11606-024-08888-3. Epub 2024 Jul 17. J Gen Intern Med. 2024. PMID: 39020230
References
-
- Bohnert ASB, Valenstein M, Bair MJ, et al. Association between opioid prescribing patterns and opioid overdose‐related deaths. JAMA. 2011;305(13):1315‐1321. - PubMed
-
- Dowell D, Haegerich TM, Chou R. CDC guideline for prescribing opioids for chronic pain—United States, 2016. MMWR Recomm Rep. 2016;65(1):1‐49. - PubMed
-
- Davis CS, Lieberman AJ. Laws limiting prescribing and dispensing of opioids in the United States, 1989–2019. Addiction. 2021;116(7):1817‐1827. - PubMed
-
- Chua KP, Kimmel L, Brummett CM. Disappointing early results from opioid prescribing limits for acute pain. JAMA Surg. 2020;155(5):375‐376. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

