Riding the wave: a quantitative report of electrocardiogram utilization for myocardial infarction confirmation
- PMID: 35802516
- PMCID: PMC9359650
- DOI: 10.1152/ajpheart.00201.2022
Riding the wave: a quantitative report of electrocardiogram utilization for myocardial infarction confirmation
Abstract
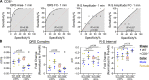
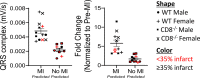
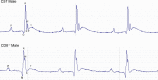
The purpose of this study was to generate a quantitative profile of electrocardiograms (ECGs) for confirming surgical success of permanent coronary artery ligation. An ECG was recorded at baseline, and 0, 1, and 5 min after ligation and analyzed using iWorkx LabScribe software. Cohort 1 (C57Bl6/J, n = 8/sex) was enrolled to determine ECG characteristics that were confirmed in cohort 2 (C57Bl6/J, n = 6/sex; CD8-/-n = 6 males/4 females). Of the 16 mice in cohort 1, 12 (6/sex) had an infarct ≥35% and four mice (2/sex) had <35% based on 2,3,5-triphenyltetrazolium chloride staining. After ligation, the QRS complex and R-S amplitude were significantly different compared with baseline. No differences were observed in the R-S amplitude between mice with infarcts ≥35% versus <35% at any time point, whereas the QRS complex was significant 1 min after ligation. Receiver operating characteristic (ROC) curve linked changes in the QRS complex but not the R-S amplitude at 1 and 5 min with surgical success. Data were normalized to baseline values to calculate fold change. ROC analysis of the normalized QRS data indicated strong sensitivity and specificity for infarcts ≥35%; normalized R-S amplitude remained nonsignificant. With a cutoff generated by ROC analysis of cohort 1 (>80% sensitivity; >90% specificity), the non-normalized QRS complex of cohort 2 had an 86% success rate (2 false positives; 1 false negative). The normalized data had a 77% success rate (2 false positives; 3 false negatives). Neither sex nor genotype was associated with false predictions (P = 0.18). Our data indicate that the area under the QRS complex 1 min after ligation can improve reproducibility in MI surgeries.NEW & NOTEWORTHY Our study describes a quantitative method for using an electrocardiogram (ECG) to determine which animals have infarcts that reflect coronary artery ligation. Using a quantitative ECG, investigators will have the benefit of having real-time feedback during the procedure, which will ultimately decrease the amount of time investigators spend performing experiments. This overall increase in efficiency will help investigators decrease animal numbers used due to better surgical outcomes.
Keywords: electrocardiogram; heart; myocardial infarction; reproducibility.
Conflict of interest statement
No conflicts of interest, financial or otherwise, are declared by the authors.
Figures





References
-
- Ibánez B, James S, Agewall S, Antunes MJ, Bucciarelli-Ducci C, Bueno H, Caforio ALP, Crea F, Goudevenos JA, Halvorsen S, Hindricks G, Kastrati A, Lenzen MJ, Prescott E, Roffi M, Valgimigli M, Varenhorst C, Vranckx P, Widimský P. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Rev Esp Cardiol (Engl Ed) 70: 1082, 2017. doi: 10.1016/j.rec.2017.11.010. - DOI - PubMed
-
- Lindsey ML, de Castro Bras LE, DeLeon-Pennell KY, Frangogiannis NG, Halade GV, O'Meara CC, Spinale FG, Kassiri Z, Kirk JA, Kleinbongard P, Ripplinger CM, Brunt KR. Reperfused vs. nonreperfused myocardial infarction: when to use which model. Am J Physiol Heart Circ Physiol 321: H208–H213, 2021. doi: 10.1152/ajpheart.00234.2021. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

