Time Free From Hospitalization in Children and Adolescents With Cystic Fibrosis: Findings From FEV1, Lung Clearance Index and Peak Work Rate
- PMID: 35813385
- PMCID: PMC9257036
- DOI: 10.3389/fped.2022.926248
Time Free From Hospitalization in Children and Adolescents With Cystic Fibrosis: Findings From FEV1, Lung Clearance Index and Peak Work Rate
Abstract
Background: An exercise test combined with a multiple breath washout nitrogen test (MBWN2) may offer a comprehensive clinical evaluation of cystic fibrosis (CF) disease in children with normal spirometry. The purpose of the present study is to explore whether information derived from spirometry, MBWN2, and exercise tests can help the CF multidisciplinary team to characterize time free from hospitalization due to pulmonary exacerbation (PE) in a cohort of pediatric patients with CF.
Methods: This prospective observational study was carried out at the Lombardia Region Reference Center for Cystic Fibrosis in Milano, Italy. In 2015, we consecutively enrolled children and adolescents aged <18 years with spirometry, MBWN2, and Godfrey exercise test performed during an outpatient visit.
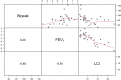
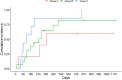
Results: Over a median follow-up time of 2.2 years (interquartile range [IQR], 2.01; 3.18), 28 patients aged between 13.0 and 17.4 years were included. When lung functions were outside the normal range, 50% of patients were hospitalized 4 months after the outpatient visit, and their response to exercise was abnormal (100%). Half of the individuals with normal forced expiratory volume in the first second (FEV1) and abnormal lung clearance index (LCI) experienced the first hospital admission 9 months after the clinic visit, and 84.2% presented an abnormal response to exercise. Conversely, 15.8% had abnormal exercise responses when lung functions were considered normal, with half of the adolescents hospitalized at 11 months.
Conclusion: Maintaining ventilation homogeneity, along with a normal ability to sustain intense work, may have a positive impact on the burden of CF disease, here conceived as time free from hospitalization due to PE.
Keywords: cystic fibrosis; exercise tolerance; hospitalization; lung clearance index (LCI); lung function; pulmonary exacerbation.
Copyright © 2022 Gambazza, Mariani, Brivio, Carta, Blardone, Lisiero, Russo and Colombo.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Comparison of Multiple Breath Washout and Spirometry in Children with Primary Ciliary Dyskinesia and Cystic Fibrosis and Healthy Controls.Ann Am Thorac Soc. 2020 Sep;17(9):1085-1093. doi: 10.1513/AnnalsATS.201905-375OC. Ann Am Thorac Soc. 2020. PMID: 32603187 Free PMC article.
-
Variability of lung clearance index in clinically stable cystic fibrosis lung disease in school age children.J Cyst Fibros. 2018 Mar;17(2):236-241. doi: 10.1016/j.jcf.2017.08.004. Epub 2017 Aug 16. J Cyst Fibros. 2018. PMID: 28822728
-
Abnormal Lung Clearance Index in Cystic Fibrosis Children with Normal FEV1 and Single-Breath Nitrogen Washout Test.Lung. 2021 Feb;199(1):37-41. doi: 10.1007/s00408-020-00412-8. Epub 2021 Jan 3. Lung. 2021. PMID: 33389068
-
Lung clearance index in subjects with cystic fibrosis in Italy.Ital J Pediatr. 2019 May 2;45(1):56. doi: 10.1186/s13052-019-0647-5. Ital J Pediatr. 2019. PMID: 31046783 Free PMC article. Review.
-
The lung clearance index as a monitoring tool in cystic fibrosis: ready for the clinic?Curr Opin Pulm Med. 2018 Nov;24(6):579-585. doi: 10.1097/MCP.0000000000000515. Curr Opin Pulm Med. 2018. PMID: 30095491 Review.
Cited by
-
Ventilatory Threshold and Risk of Pulmonary Exacerbations in Cystic Fibrosis.Respir Care. 2023 May;68(5):620-627. doi: 10.4187/respcare.10428. Epub 2023 Apr 4. Respir Care. 2023. PMID: 37015814 Free PMC article.
References
-
- Vandekerckhove K, Keyzer M, Cornette J, Coomans I, Pyl F, De Baets F, et al. . Exercise performance and quality of life in children with cystic fibrosis and mildly impaired lung function: relation with antibiotic treatments and hospitalization. Eur J Pediatr. (2017) 176:1689–96. 10.1007/s00431-017-3024-7 - DOI - PubMed

