Double stapling method for closure of intraoperative alveolar air leakage adjacent to the staple line: a randomized experimental study on ex vivo porcine lungs
- PMID: 35813731
- PMCID: PMC9264071
- DOI: 10.21037/jtd-21-1960
Double stapling method for closure of intraoperative alveolar air leakage adjacent to the staple line: a randomized experimental study on ex vivo porcine lungs
Abstract
Background: Alveolar air leakage from a pleural defect around the staple line is one of the complications after wedge resection of the lung. An intraoperative closure of the pleural defect by suturing can cause additional pleural rupture due to tension of the pleura adjacent to staple lines. Therefore, we have introduced a novel closure method for pleural defect adjacent to the staple line, named the double stapling method. This study compared the efficacy of two closure methods; the double stapling method and conventional suturing method with pledgets using ex vivo porcine lungs.
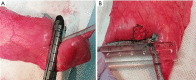
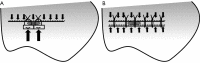
Methods: The double stapling method involves closing the pleural defect by suturing the two parallel staple lines at both sides of the pleural defect. This method was developed to distribute the pleural tension around the needle holes of suturing. As a model of pleural defect adjacent to the staple line after wedge resection, wedge resection of the caudal lobe of left porcine lungs was performed, and a superficial square pleural defect (10 mm × 10 mm) adjacent to the staple line was made by scalpel. The defect was closed using the following two methods: (I) suturing with pledgets (n=10); and (II) double stapling method (n=10). The lobe was inflated in water at an airway pressure of 20, 25, and 30 cmH2O; closure success or failure was judged by the absence or presence of air leakage.
Results: The closure success was confirmed in 2 (20%) out of 10 cases in the suturing with pledgets group and 9 (90%) out of 10 in the double stapling method group (P=0.007). In 4 out of 10 cases in the suturing with pledgets group, new pleural clefts longer than 3 mm were created around the needle holes of suturing.
Conclusions: Ex vivo experiments have suggested the superiority of the double stapling method for the intraoperative closure of alveolar air leakage adjacent to the staple line after wedge resection, compared to conventional suturing with the pledget method.
Keywords: Alveolar air leak; stapler; wedge resection.
2022 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jtd.amegroups.com/article/view/10.21037/jtd-21-1960/coif). All authors received scholarship donation from Eli Lilly Japan K.K., Shionogi & Co., Ltd., Taiho Pharmaceutical Co., Ltd., Chugai Pharmaceutical Co., Ltd., Daiichi Sankyo Co., Ltd., Kyowa Kirin Co., Ltd., Ethicon, Inc., and Covidien Japan Inc. The authors have no other conflicts of interest to declare.
Figures




Comment in
-
Air leaks: leave well enough alone.J Thorac Dis. 2022 Sep;14(9):3119-3121. doi: 10.21037/jtd-22-811. J Thorac Dis. 2022. PMID: 36245622 Free PMC article. No abstract available.
References
LinkOut - more resources
Full Text Sources
Research Materials
