Postoperative Complications of Free Flap Reconstruction in Moderate-Advanced Head and Neck Squamous Cell Carcinoma: A Prospective Cohort Study Based on Real-World Data
- PMID: 35814388
- PMCID: PMC9263716
- DOI: 10.3389/fonc.2022.792462
Postoperative Complications of Free Flap Reconstruction in Moderate-Advanced Head and Neck Squamous Cell Carcinoma: A Prospective Cohort Study Based on Real-World Data
Abstract
Background: Postoperative complications (POCs) of moderate-advanced head and neck squamous cell carcinoma (HNSCC) after free flap reconstruction have received little attention. We investigated the risk factors that lead to POCs and their impact on management and prognosis.
Patients and methods: A single-center, prospective cohort study was conducted at Beijing Stomatological Hospital on primary HNSCC patients treated between 2015 and 2020.
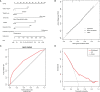
Results: In total, 399 consecutive HNSCC patients who underwent radical resection of the primary tumor and free flap reconstruction were enrolled in this study, 155(38.8%) experienced POCs. The occurrence of POCs directly led to worse short-term outcomes and poorer long-term overall survival (P=0.0056). Weight loss before the operation (P=0.097), Tumor site (P=0.002), stage T4b (P=0.016), an ACE-27 index of 2-3 (P=0.040), operation time≥8h (P=0.001) and Clindamycin as antibiotic prophylaxis (P=0.001) were significantly associated with POCs.
Conclusions: The occurrence of POCs significantly leads to worse short-term outcomes and increases the patients' burden.
Keywords: free flap reconstruction; head and neck cancer; postoperative complications; prediction model; risk factors.
Copyright © 2022 Li, Wang, Wei, Li, Liu, Cheng, Niu, Han and Feng.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


Similar articles
-
Comprehensive complication index: A new reporting standard for postoperative complications of free-flap reconstruction in head and neck cancer patients.Oral Surg Oral Med Oral Pathol Oral Radiol. 2023 Jan;135(1):33-41. doi: 10.1016/j.oooo.2022.05.007. Epub 2022 May 20. Oral Surg Oral Med Oral Pathol Oral Radiol. 2023. PMID: 35985962
-
Clinical impact of albumin in advanced head and neck cancer patients with free flap reconstruction-a retrospective study.PeerJ. 2018 Mar 12;6:e4490. doi: 10.7717/peerj.4490. eCollection 2018. PeerJ. 2018. PMID: 29576961 Free PMC article.
-
Systemic Inflammatory Markers as Predictors of Postoperative Complications and Survival in Patients With Advanced Head and Neck Squamous Cell Carcinoma Undergoing Free-Flap Reconstruction.J Oral Maxillofac Surg. 2022 Apr;80(4):744-755. doi: 10.1016/j.joms.2021.12.011. Epub 2021 Dec 22. J Oral Maxillofac Surg. 2022. PMID: 35032441
-
Impact of Postoperative Complications on Long-Term Survival After Resection of Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis.Ann Surg Oncol. 2021 Dec;28(13):8221-8233. doi: 10.1245/s10434-021-10317-2. Epub 2021 Jun 23. Ann Surg Oncol. 2021. PMID: 34160708
-
Evolution of treatment and high-risk features in resectable locally advanced Head and Neck squamous cell carcinoma with special reference to extracapsular extension of nodal disease.J BUON. 2015 Jul-Aug;20(4):943-53. J BUON. 2015. PMID: 26416042 Review.
Cited by
-
The Freestyle Multiperforator Island Flap: Beyond the Keystone Flap.Plast Reconstr Surg Glob Open. 2025 Feb 10;13(2):e6503. doi: 10.1097/GOX.0000000000006503. eCollection 2025 Feb. Plast Reconstr Surg Glob Open. 2025. PMID: 39931118 Free PMC article.
-
Exosomes Derived from Bone Marrow Mesenchymal Stem Cells Alleviate Ischemia-Reperfusion Injury and Promote Survival of Skin Flaps in Rats.Life (Basel). 2022 Oct 9;12(10):1567. doi: 10.3390/life12101567. Life (Basel). 2022. PMID: 36295004 Free PMC article.
-
The use of artificial intelligence in reconstructive surgery for head and neck cancer: a systematic review.Eur Arch Otorhinolaryngol. 2024 Nov;281(11):6057-6068. doi: 10.1007/s00405-024-08663-4. Epub 2024 Apr 25. Eur Arch Otorhinolaryngol. 2024. PMID: 38662215
-
Incidence and risk factors for postoperative delirium after head and neck cancer surgery: an updated meta-analysis.BMC Neurol. 2023 Oct 17;23(1):371. doi: 10.1186/s12883-023-03418-w. BMC Neurol. 2023. PMID: 37848819 Free PMC article. Review.
-
Ovine Forestomach Matrix in the Surgical Management of Complex Volumetric Soft Tissue Defects: A Retrospective Pilot Case Series.Eplasty. 2023 Sep 27;23:e66. eCollection 2023. Eplasty. 2023. PMID: 38045101 Free PMC article.
References
-
- Dort JC, Farwell DG, Findlay M, Huber GF, Kerr P, Shea-Budgell MA, et al. . Optimal Perioperative Care in Major Head and Neck Cancer Surgery With Free Flap Reconstruction: A Consensus Review and Recommendations From the Enhanced Recovery After Surgery Society. JAMA Otolaryngol Head Neck Surg (2017) 143:292–303. doi: 10.1001/jamaoto.2016.2981 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

