Implementation and Outcomes of a Model of Care for Placenta Accreta Spectrum in a Community-Based Private Practice
- PMID: 35815573
- PMCID: PMC11105945
- DOI: 10.1055/s-0042-1749664
Implementation and Outcomes of a Model of Care for Placenta Accreta Spectrum in a Community-Based Private Practice
Abstract
Objective: The aim of the study is to describe a model of care and outcomes for placenta accreta spectrum (PAS) implemented in the context of a community based non-academic health system.
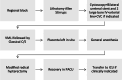
Study design: The program for management of PAS includes a multidisciplinary team approach with protocols for ultrasound assessment, diagnosis, and surgery. The program was implemented in the two largest private hospitals in the Twin Cities, Minnesota, United States. Maternal and fetal outcomes as well as cost were compared for histopathologic confirmed PAS cases before (2007-2014, n = 41) and after (2015-2017, n = 26) implementation of the PAS program.
Results: Implementation of the PAS program was associated with ICU admission reductions from 53.7 to 19.2%, p = 0.005; a decrease of 1,682 mL in mean estimated blood loss (EBL) (p = 0.061); a decrease in transfusion from 85.4 to 53.9% (p = 0.005). The PAS program also resulted in a (non-significant) decrease in both surgical complications from 48.8 to 38.5% (p = 0.408) and postoperative complications from 61.0 to 42.3% (p = 0.135). The total cost of care for PAS cases in the 3 years after implementation of the program decreased by 33%.
Conclusion: The implementation of a model of care for PAS led by a perinatology practice at a large regional non-academic referral center resulted in reductions of ICU admissions, operating time, transfusion, selected surgical complications, overall postoperative complications, and cost.
Key points: · Implementation of a PAS care model resulted in reduced ICU admissions from 53.7% to 19.2%.. · Patient safety increased by reducing blood loss, transfusions and postoperative complications.. · This model decreased operating time, as well as total cost of care by 33%..
The Author(s). This is an open access article published by Thieme under the terms of the Creative Commons Attribution-NonDerivative-NonCommercial License, permitting copying and reproduction so long as the original work is given appropriate credit. Contents may not be used for commercial purposes, or adapted, remixed, transformed or built upon. (https://creativecommons.org/licenses/by-nc-nd/4.0/).
Conflict of interest statement
Disclosure The authors report no conflicts of interest in this work.
Figures
Similar articles
-
Successful multidisciplinary team management of placenta accreta spectrum disorder: A referral center model in a middle-income country.Int J Gynaecol Obstet. 2024 May;165(2):813-822. doi: 10.1002/ijgo.15339. Epub 2024 Jan 8. Int J Gynaecol Obstet. 2024. PMID: 38189162
-
Placenta Accreta Spectrum Treatment With Intraoperative Multivessel Embolization: the PASTIME protocol.Am J Obstet Gynecol. 2021 Oct;225(4):442.e1-442.e10. doi: 10.1016/j.ajog.2021.07.001. Epub 2021 Jul 7. Am J Obstet Gynecol. 2021. PMID: 34245679
-
Maternal outcomes in unexpected placenta accreta spectrum disorders: single-center experience with a multidisciplinary team.Am J Obstet Gynecol. 2019 Oct;221(4):337.e1-337.e5. doi: 10.1016/j.ajog.2019.05.035. Epub 2019 Jun 4. Am J Obstet Gynecol. 2019. PMID: 31173748 Free PMC article.
-
Maternal outcomes of conservative management and cesarean hysterectomy for placenta accreta spectrum disorders: a systematic review and meta-analysis.BMC Pregnancy Childbirth. 2024 Jul 5;24(1):463. doi: 10.1186/s12884-024-06658-x. BMC Pregnancy Childbirth. 2024. PMID: 38969992 Free PMC article.
-
Anesthesia Considerations for Placenta Accreta Spectrum.Am J Perinatol. 2023 Jul;40(9):980-987. doi: 10.1055/s-0043-1761637. Epub 2023 Jun 19. Am J Perinatol. 2023. PMID: 37336215 Review.
Cited by
-
Neonatal outcomes in the surgical management of placenta accreta spectrum disorders: a retrospective single-center observational study from 468 Vietnamese pregnancies beyond 28 weeks of gestation.BMC Pregnancy Childbirth. 2024 Apr 2;24(1):228. doi: 10.1186/s12884-024-06349-7. BMC Pregnancy Childbirth. 2024. PMID: 38566074 Free PMC article.
-
Intended Conservative Management Versus Caesarean Hysterectomy for Known or Suspected Placenta Accreta Spectrum: A Cost-Effectiveness Analysis.BJOG. 2025 Jul;132(8):1096-1103. doi: 10.1111/1471-0528.18025. Epub 2024 Dec 5. BJOG. 2025. PMID: 39639523 Free PMC article.
References
-
- Publications Committee, Society for Maternal-Fetal Medicine . Belfort M A. Placenta accreta. Am J Obstet Gynecol. 2010;203(05):430–439. - PubMed
-
- Silver R M, Fox K A, Barton J R et al.Center of excellence for placenta accreta. Am J Obstet Gynecol. 2015;212(05):561–568. - PubMed
-
- Committee on Obstetric Practice . Committee opinion no. 529: placenta accreta. Obstet Gynecol. 2012;120(01):207–211. - PubMed
-
- Eller A G, Porter T F, Soisson P, Silver R M. Optimal management strategies for placenta accreta. BJOG. 2009;116(05):648–654. - PubMed
-
- Al-Khan A, Gupta V, Illsley N P et al.Maternal and fetal outcomes in placenta accreta after institution of team-managed care. Reprod Sci. 2014;21(06):761–771. - PubMed