Low anti-Müllerian hormone levels are associated with an increased risk of incident early-onset vasomotor symptoms among premenopausal women
- PMID: 35831405
- PMCID: PMC9279494
- DOI: 10.1038/s41598-022-16182-7
Low anti-Müllerian hormone levels are associated with an increased risk of incident early-onset vasomotor symptoms among premenopausal women
Abstract
The role of anti-Müllerian hormone (AMH) levels in incident vasomotor symptoms (VMS) is largely unknown. This study aimed to investigate the relationship between AMH levels and the development of early-onset VMS among premenopausal women. Our cohort study comprised 2041 premenopausal women aged 42-52 years free of VMS at baseline whose AMH levels were measured. VMS, including hot flushes and night sweats, were assessed using the Korean version of the Menopause-specific Quality of Life questionnaire. Early-onset VMS was defined as the occurrence of VMS prior to menopause. Parametric proportional hazards models were used to estimate adjusted hazard ratios (HRs) and 95% CI. During a median follow-up of 4.4 years, 708 premenopausal women developed early-onset VMS (incidence rate, 8.0 per 100 person-years). Lower AMH levels were statistically significantly associated with an increased risk of early-onset VMS. After adjusting for age and other confounders, multivariable-adjusted HRs (95% CI) for incident VMS comparing AMH quintiles 4-1 to the highest quintile were 1.02 (0.78-1.33), 1.37 (1.06-1.76), 1.36 (1.04-1.76), and 2.38 (1.84-3.08), respectively (P for trend < 0.001). Our results support an independent role of serum AMH levels in predicting incident early-onset VMS among premenopausal women in the late reproductive stage.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
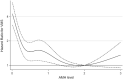
Figures

Similar articles
-
Alcohol Consumption Patterns and Risk of Early-Onset Vasomotor Symptoms in Premenopausal Women.Nutrients. 2022 May 29;14(11):2276. doi: 10.3390/nu14112276. Nutrients. 2022. PMID: 35684078 Free PMC article.
-
Vasomotor symptom characteristics: are they risk factors for incident diabetes?Menopause. 2018 May;25(5):520-530. doi: 10.1097/GME.0000000000001033. Menopause. 2018. PMID: 29206771 Free PMC article.
-
High low-density lipoprotein cholesterol level is associated with an increased risk of incident early-onset vasomotor symptoms.Sci Rep. 2022 Aug 27;12(1):14652. doi: 10.1038/s41598-022-19028-4. Sci Rep. 2022. PMID: 36030298 Free PMC article.
-
Vasomotor symptoms and risk of cardiovascular disease in peri- and postmenopausal women: A systematic review and meta-analysis.Maturitas. 2023 May;171:13-20. doi: 10.1016/j.maturitas.2023.02.004. Epub 2023 Mar 6. Maturitas. 2023. PMID: 36907116
-
Treatment strategies for reducing the burden of menopause-associated vasomotor symptoms.J Manag Care Pharm. 2008 Apr;14(3 Suppl):14-9. doi: 10.18553/jmcp.2008.14.S6-A.14. J Manag Care Pharm. 2008. PMID: 18439062 Free PMC article. Review.
Cited by
-
Antimüllerian Hormone as a Tool to Predict the Age at Menopause.Geriatrics (Basel). 2023 May 19;8(3):57. doi: 10.3390/geriatrics8030057. Geriatrics (Basel). 2023. PMID: 37218837 Free PMC article.
-
Impact of Systemic Lupus Erythematosus on Conception: Insights into Infertility, Fertility Preservation, Assisted Reproductive Technology, and Pregnancy Outcomes.Semin Reprod Med. 2024 Sep;42(3):209-227. doi: 10.1055/s-0044-1793827. Epub 2024 Dec 12. Semin Reprod Med. 2024. PMID: 39667369 Free PMC article. Review.
-
Associations of anti-Müllerian hormone levels among women in their mid-30s with menopausal symptoms ~14 years later.Menopause. 2024 Jun 1;31(6):505-511. doi: 10.1097/GME.0000000000002360. Epub 2024 Apr 30. Menopause. 2024. PMID: 38688466 Free PMC article.
-
Maximizing ovarian function and fertility following chemotherapy in premenopausal patients: Is there a role for ovarian suppression?Gynecol Oncol Rep. 2024 Apr 7;53:101383. doi: 10.1016/j.gore.2024.101383. eCollection 2024 Jun. Gynecol Oncol Rep. 2024. PMID: 38633671 Free PMC article. Review.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

