Hepatic Function Predictive Value of Hepatic Venous Waveform versus Portal Vein Velocity in Liver Cirrhosis
- PMID: 35832354
- PMCID: PMC9272706
- DOI: 10.4103/JMU.JMU_91_21
Hepatic Function Predictive Value of Hepatic Venous Waveform versus Portal Vein Velocity in Liver Cirrhosis
Abstract
Background: This study assessed the hepatic vein waveform (HVW) and mean maximum portal vein velocity (MM-PVV) on Doppler ultrasound in patients with liver cirrhosis (LC) and compared it with that of age and sex-matched controls. It correlated the degree of HVW abnormality and MM-PVV changes with liver function based on Child-Turcotte-Pugh (CTP) to determine which was more predictive of CTP.
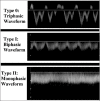
Methods: Sixty patients with LC and 60 healthy controls were consecutively recruited into this study. Each patient was classed based on the CTP system after relevant tests. Doppler evaluation of the hepatic vein (HV) and MM-PVV were performed. HVW obtained was classified either into triphasic, biphasic, or monophasic.
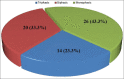
Results: Sixty cirrhotic and 60 age-matched control subjects aged 19-69 and 18-69 years, respectively, completed this study. All control subjects had a normal HVW pattern while 46 (76.7%) cirrhotic subjects had abnormal HVW (P < 0.001). The MM-PVV was significantly lower in cirrhotic subjects than in controls; 22.8 cm/s versus 33.6 cm/s (P < 0.001). The degree of HVW abnormality among cirrhotics showed a significant positive correlation with CTP (r = 0.283, P = 0.029). MM-PVV on the other hand showed no correlation with CTP class (r = -0.124; P = 0.346). Linear regression showed that HVW was a significant predictor of hepatic dysfunction based on CTP.
Conclusion: Changes in the waveform pattern of the HVs are a good predictor of the derangement of hepatic function in patients with LC than changes in PVV. HVW pattern could therefore serve as an adjunct to CTP class in hepatic function assessment.
Keywords: Hepatic vein waveform; liver cirrhosis; portal vein velocity; ultrasound.
Copyright: © 2022 Journal of Medical Ultrasound.
Conflict of interest statement
There are no conflicts of interest.
Figures
References
-
- Macarini L, Stoppino LP. Radiologic assessment of liver fibrosis – Present and future. In: Practical Management of Chronic Viral Hepatitis. In Tech. 2013. pp. 115–6. https://www.intechopen.com/books/3312.
-
- Goyal N, Jain N, Rachapalli V, Cochlin DL, Robinson M. Non-invasive evaluation of liver cirrhosis using ultrasound. Clin Radiol. 2009;64:1056–66. - PubMed
-
- Tsochatzis EA, Bosch J, Burroughs AK. Liver cirrhosis. Lancet. 2014;383:1749–61. - PubMed
-
- Baik SK, Kim JW, Kim HS, Kwon SO, Kim YJ, Park JW, et al. Recent variceal bleeding: Doppler US hepatic vein waveform in assessment of severity of portal hypertension and vasoactive drug response. Radiology. 2006;240:574–80. - PubMed
LinkOut - more resources
Full Text Sources