Imaging the acute respiratory distress syndrome: past, present and future
- PMID: 35833958
- PMCID: PMC9281340
- DOI: 10.1007/s00134-022-06809-8
Imaging the acute respiratory distress syndrome: past, present and future
Abstract
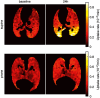
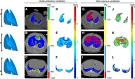
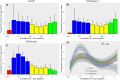
In patients with the acute respiratory distress syndrome (ARDS), lung imaging is a fundamental tool in the study of the morphological and mechanistic features of the lungs. Chest computed tomography studies led to major advances in the understanding of ARDS physiology. They allowed the in vivo study of the syndrome's lung features in relation with its impact on respiratory physiology and physiology, but also explored the lungs' response to mechanical ventilation, be it alveolar recruitment or ventilator-induced lung injuries. Coupled with positron emission tomography, morphological findings were put in relation with ventilation, perfusion or acute lung inflammation. Lung imaging has always been central in the care of patients with ARDS, with modern point-of-care tools such as electrical impedance tomography or lung ultrasounds guiding clinical reasoning beyond macro-respiratory mechanics. Finally, artificial intelligence and machine learning now assist imaging post-processing software, which allows real-time analysis of quantitative parameters that describe the syndrome's complexity. This narrative review aims to draw a didactic and comprehensive picture of how modern imaging techniques improved our understanding of the syndrome, and have the potential to help the clinician guide ventilatory treatment and refine patient prognostication.
Keywords: Acute respiratory distress syndrome; Computed tomography; Electrical impedance tomography; Lung ultrasounds; Positron emission tomography; Ventilator-induced lung injuries.
© 2022. Springer-Verlag GmbH Germany, part of Springer Nature.
Conflict of interest statement
LB has declared no conflicts of interest, financial or otherwise. DST has declared funding from the National Institute for Health, Hamilton Medical, and Mindray, all outside the present work. JCR has declared funding of an experimental study by Hamilton Medical, unrelated to the present work.
Figures

Comment in
-
Air leak, barotrauma susceptibility, and imaging in acute respiratory distress syndrome: novel application of an old tool.Intensive Care Med. 2022 Dec;48(12):1837-1838. doi: 10.1007/s00134-022-06902-y. Epub 2022 Oct 6. Intensive Care Med. 2022. PMID: 36203037 Free PMC article. No abstract available.
Similar articles
-
Mechanical ventilation in acute respiratory distress syndrome: The open lung revisited.Med Intensiva. 2017 Dec;41(9):550-558. doi: 10.1016/j.medin.2016.12.012. Epub 2017 Feb 24. Med Intensiva. 2017. PMID: 28238441 Review. English, Spanish.
-
Physiologically variable ventilation reduces regional lung inflammation in a pediatric model of acute respiratory distress syndrome.Respir Res. 2020 Oct 31;21(1):288. doi: 10.1186/s12931-020-01559-x. Respir Res. 2020. PMID: 33129315 Free PMC article.
-
Electrical Impedance Tomography in Acute Respiratory Distress Syndrome Management.Crit Care Med. 2022 Aug 1;50(8):1210-1223. doi: 10.1097/CCM.0000000000005582. Epub 2022 May 23. Crit Care Med. 2022. PMID: 35607967 Review.
-
[The mechanical ventilation guided by electrical impedance tomography in acute respiratory distress syndrome].Zhonghua Yi Xue Za Zhi. 2024 Apr 16;104(15):1247-1252. doi: 10.3760/cma.j.cn112137-20231007-00655. Zhonghua Yi Xue Za Zhi. 2024. PMID: 38637164 Chinese.
-
Acute Respiratory Distress Syndrome: Advances in Diagnosis and Treatment.JAMA. 2018 Feb 20;319(7):698-710. doi: 10.1001/jama.2017.21907. JAMA. 2018. PMID: 29466596 Review.
Cited by
-
[Artificial intelligence in intensive care medicine].Med Klin Intensivmed Notfmed. 2024 Apr;119(3):189-198. doi: 10.1007/s00063-024-01117-z. Epub 2024 Mar 28. Med Klin Intensivmed Notfmed. 2024. PMID: 38546864 Review. German.
-
Differences in clinical characteristics and quantitative lung CT features between vaccinated and not vaccinated hospitalized COVID-19 patients in Italy.Ann Intensive Care. 2023 Apr 3;13(1):24. doi: 10.1186/s13613-023-01103-2. Ann Intensive Care. 2023. PMID: 37010706 Free PMC article.
-
Combined lung compliance and oxygenation dynamics predict high-flow nasal cannula failure in acute respiratory distress syndrome: a retrospective cohort study.Am J Transl Res. 2025 Jun 15;17(6):4175-4186. doi: 10.62347/ELGT2750. eCollection 2025. Am J Transl Res. 2025. PMID: 40672630 Free PMC article.
-
Use of radiolabeled hyaluronic acid for preclinical assessment of inflammatory injury and acute respiratory distress syndrome.Nucl Med Biol. 2022 Nov-Dec;114-115:86-98. doi: 10.1016/j.nucmedbio.2022.10.002. Epub 2022 Oct 14. Nucl Med Biol. 2022. PMID: 36270074 Free PMC article.
-
Dead space ventilation-related indices: bedside tools to evaluate the ventilation and perfusion relationship in patients with acute respiratory distress syndrome.Crit Care. 2023 Feb 3;27(1):46. doi: 10.1186/s13054-023-04338-4. Crit Care. 2023. PMID: 36732812 Free PMC article. Review.
References
-
- The ARDS Definition Task Force Acute respiratory distress syndrome: the Berlin definition. JAMA. 2012;307:2526–2533. - PubMed
-
- Brusasco C, Santori G, Tavazzi G, Via G, Robba C, Gargani L, Mojoli F, Mongodi S, Bruzzo E, Trò R, Boccacci P, Isirdi A, Forfori F, Corradi F. Second-order grey-scale texture analysis of pleural ultrasound images to differentiate acute respiratory distress syndrome and cardiogenic pulmonary edema. J Clin Monit Comput. 2022;36:131–140. doi: 10.1007/s10877-020-00629-1. - DOI - PMC - PubMed
-
- Wallet F, Delannoy B, Haquin A, Debord S, Leray V, Bourdin G, Bayle F, Richard JC, Boussel L, Guerin C. Evaluation of recruited lung volume at inspiratory plateau pressure with PEEP using bedside digital chest X-ray in patients with acute lung injury/ARDS. Respir Care. 2013;58:416–423. doi: 10.4187/respcare.01893. - DOI - PubMed
-
- Gattinoni L, Pesenti A, Bombino M, Baglioni S, Rivolta M, Rossi F, Rossi G, Fumagalli R, Marcolin R, Mascheroni D, et al. Relationships between lung computed tomographic density, gas exchange, and PEEP in acute respiratory failure. Anesthesiology. 1988;69:824–832. doi: 10.1097/00000542-198812000-00005. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

