Cystic liver lesions: a pictorial review
- PMID: 35838923
- PMCID: PMC9287528
- DOI: 10.1186/s13244-022-01242-3
Cystic liver lesions: a pictorial review
Abstract
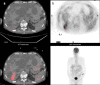
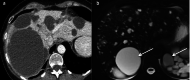
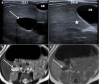
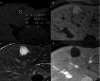
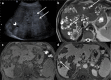
Hepatic cysts (HC) are sac-like structures mainly filled with liquid and showing a distinct membrane. They are usually found incidentally through imaging. A wide spectrum of imaging patterns may be observed for common and uncommon, neoplastic and non-neoplastic diseases. While simple hepatic cysts occur frequently and do not require any treatment or follow-up, non-typical cysts should be carefully analysed to avoid misdiagnosing a lesion that would require appropriate management. Therefore, adequate knowledge of all the relevant imaging patterns is critical to secure an accurate diagnosis. The aim of this review is to describe the imaging features of the different types of hepatic cysts.
Keywords: Computed tomography; Cysts; Hepatic; Magnetic resonance imaging; Ultrasonography.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
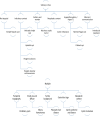
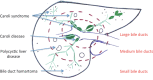

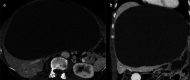
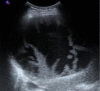
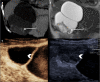
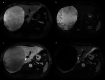

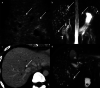


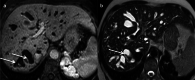


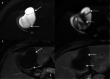
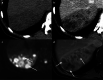
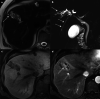
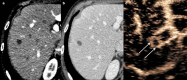


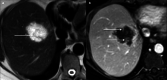
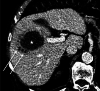
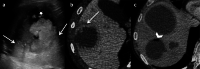
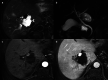

References
Publication types
LinkOut - more resources
Full Text Sources

