Multiple VHL-related hemangioblastomas and holocord syrinx: identifying the causative lesion. Illustrative case
- PMID: 35855304
- PMCID: PMC9265196
- DOI: 10.3171/CASE21296
Multiple VHL-related hemangioblastomas and holocord syrinx: identifying the causative lesion. Illustrative case
Abstract
Background: Brainstem and spinal cord hemangioblastomas are a common manifestation of von Hippel-Lindau (VHL) disease. Cysts and associated syringes are the most common cause of significant morbidity in these patients. Surgical treatment of symptomatic hemangioblastomas are often complicated by the presence of multiple potential lesions, leading to cyst and syrinx formation.
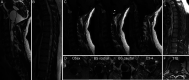
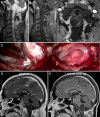
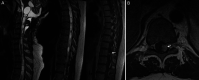
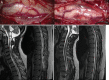
Observations: The authors present a case of a patient with multiple VHL-related hemangioblastomas who presented with syringobulbia and holocord syrinx. Resection of two cyst wall hemangioblastomas and one cervical hemangioblastoma only transiently improved syringobulbia. Eventual resolution of syringobulbia and collapse of the holocord syrinx only occurred following removal of a large lower thoracic hemangioblastoma.
Lessons: Surgical management of hemangioblastomas and associated cysts in patients with VHL should only target lesions most likely contributing to neurological deficits as excess surgical intervention risks treatment-related morbidity. The authors illustrate how anatomical and pathophysiological considerations as well as patient symptoms are key to identifying target lesions for resection and developing deliberate treatment plans.
Keywords: CNS = central nervous system; MRI = magnetic resonance imaging; POD = postoperative day; RUE = right upper extremity; VHL; VHL = von Hippel–Lindau; cyst; hemangioblastoma; syrinx; von Hippel–Lindau.
© 2021 The authors.
Conflict of interest statement
Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Figures

Similar articles
-
Neurosurgical treatment of von Hippel-Lindau-associated hemangioblastomas: benefits, risks and outcome.J Neurosurg Sci. 2008 Jun;52(2):29-36. J Neurosurg Sci. 2008. PMID: 18500215
-
The natural history of hemangioblastomas of the central nervous system in patients with von Hippel-Lindau disease.J Neurosurg. 2003 Jan;98(1):82-94. doi: 10.3171/jns.2003.98.1.0082. J Neurosurg. 2003. PMID: 12546356
-
Hemangioblastomas of the central nervous system in von Hippel-Lindau syndrome and sporadic disease.Neurosurgery. 2001 Jan;48(1):55-62; discussion 62-3. doi: 10.1097/00006123-200101000-00009. Neurosurgery. 2001. PMID: 11152361
-
Spinal cord hemangioblastomas in von Hippel-Lindau disease.Neurooncol Adv. 2024 Feb 13;6(Suppl 3):iii66-iii72. doi: 10.1093/noajnl/vdad153. eCollection 2024 Oct. Neurooncol Adv. 2024. PMID: 39430395 Free PMC article. Review.
-
Review of the Neurological Implications of von Hippel-Lindau Disease.JAMA Neurol. 2018 May 1;75(5):620-627. doi: 10.1001/jamaneurol.2017.4469. JAMA Neurol. 2018. PMID: 29379961 Review.
References
-
- Lonser RR, Glenn GM, Walther M, et al. von Hippel-Lindau disease. Lancet. 2003;361(9374):2059–2067. - PubMed
-
- Dornbos D, 3rd, Kim HJ, Butman JA, Lonser RR. Review of the neurological implications of von Hippel-Lindau disease. JAMA Neurol. 2018;75(5):620–627. - PubMed
-
- Wanebo JE, Lonser RR, Glenn GM, Oldfield EH. The natural history of hemangioblastomas of the central nervous system in patients with von Hippel-Lindau disease. J Neurosurg. 2003;98(1):82–94. - PubMed
-
- Lonser RR, Weil RJ, Wanebo JE, DeVroom HL, Oldfield EH. Surgical management of spinal cord hemangioblastomas in patients with von Hippel-Lindau disease. J Neurosurg. 2003;98(1):106–116. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

