Repeated cerebellar infarction in the affected nondominant vertebral artery distribution with reversible vertebral artery occlusion elicited by head tilt: illustrative case
- PMID: 35855310
- PMCID: PMC9241342
- DOI: 10.3171/CASE2061
Repeated cerebellar infarction in the affected nondominant vertebral artery distribution with reversible vertebral artery occlusion elicited by head tilt: illustrative case
Abstract
Background: Bow hunter's syndrome or stroke (BHS) is characterized by rotational vertebrobasilar insufficiency elicited by rotation of the neck. It is caused by dynamic and reversible occlusion of the vertebral artery (VA). Reversible symptoms of rotational vertebrobasilar insufficiency are described as bow hunter's syndrome, although brain infarction is rarely reported as bow hunter's stroke.
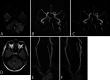
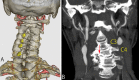
Observations: A 70-year-old man experienced repeated cerebellar infarctions three times in the posterior inferior cerebellar artery (PICA) distribution of the nondominant right VA connecting the basilar artery. The onset of symptoms indicating cerebellar infarcts and the patient's head position changes were unrelated. Dynamic digital angiography (DA) revealed that the nondominant right VA was occluded by an osteophyte from the C4 vertebral body, and the right PICA branches were shown to be passing through the distal right VA from the left VA. These findings were observed when the patient's head was tilted to the right. An arterio-arterial embolic mechanism was suggested as the cause of repeated cerebellar infarctions.
Lessons: Transient nondominant VA occlusion has been rarely reported as a cause of BHS when the head is tilted. To confirm the diagnosis of BHS, additional head tilt is recommended when performing dynamic DA in patients with a cervical osteophyte.
Keywords: 3D-CTA = three-dimensional computed tomography angiography; BHS = bow hunter’s syndrome or stroke; DA = digital angiography; DSA = digital subtraction angiography; DWI = diffusion-weighted imaging; MRA = magnetic resonance angiography; MRI = magnetic resonance imaging; PICA = posterior inferior cerebellar artery; VA = vertebral artery; bow hunter’s syndrome; cervical osteophyte; head tilt; repeated cerebellar infarction; stroke; transient vertebral artery occlusion.
© 2021 The authors.
Conflict of interest statement
Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Figures



Similar articles
-
Bow hunter's syndrome due to an embolic mechanism: illustrative case.J Neurosurg Case Lessons. 2021 Feb 15;1(7):CASE20150. doi: 10.3171/CASE20150. eCollection 2021 Feb 15. J Neurosurg Case Lessons. 2021. PMID: 36046772 Free PMC article.
-
Bow Hunter's Syndrome by Nondominant Vertebral Artery Compression: A Case Report, Literature Review, and Significance of Downbeat Nystagmus as the Diagnostic Clue.World Neurosurg. 2018 Mar;111:367-372. doi: 10.1016/j.wneu.2017.12.167. Epub 2018 Jan 5. World Neurosurg. 2018. PMID: 29309982 Review.
-
Bow hunter's syndrome revisited: 2 new cases and literature review of 124 cases.Neurosurg Focus. 2015 Apr;38(4):E7. doi: 10.3171/2015.1.FOCUS14791. Neurosurg Focus. 2015. PMID: 25828501 Review.
-
Case Report: Bow Hunter's Syndrome Caused by Compression of Extracranially Originated Posterior Inferior Cerebellar Artery.Front Neurol. 2021 Oct 26;12:756838. doi: 10.3389/fneur.2021.756838. eCollection 2021. Front Neurol. 2021. PMID: 34764931 Free PMC article.
-
A Juvenile Case of Bow Hunter's Syndrome Caused by Atlantoaxial Dislocation with Vertebral Artery Dissecting Aneurysm.World Neurosurg. 2020 May;137:393-397. doi: 10.1016/j.wneu.2020.02.041. Epub 2020 Feb 14. World Neurosurg. 2020. PMID: 32068175
Cited by
-
Safety and efficacy of dynamic catheter-directed cerebral digital subtraction angiography for diagnosis of bowhunter syndrome spectrum disorders: A systematic review of the literature.Interv Neuroradiol. 2024 Mar 13:15910199241236820. doi: 10.1177/15910199241236820. Online ahead of print. Interv Neuroradiol. 2024. PMID: 38477583 Free PMC article. Review.
-
Positional vertebral artery recanalization during neck flexion causing recurrent ischemic stroke.Radiol Case Rep. 2025 Jun 4;20(9):4180-4183. doi: 10.1016/j.radcr.2025.05.031. eCollection 2025 Sep. Radiol Case Rep. 2025. PMID: 40528914 Free PMC article.
References
-
- Bakay L, Leslie EV. Surgical treatment of vertebral artery insufficiency caused by cervical spondylosis. J Neurosurg. 1965;23(6):596–602. - PubMed
-
- Nagashima C. Surgical treatment of vertebral artery insufficiency caused by cervical spondylosis. J Neurosurg. 1970;32(5):512–521. - PubMed
-
- Husni EA, Bell HS, Storer J. Mechanical occlusion of the vertebral artery. A new clinical concept. JAMA. 1966;196(6):475–478. - PubMed
-
- Jost GF, Dalley AT. Bow hunter’s syndrome revisited: 2 new cases and literature review of 124 cases. Neurosurg Focus. 2015;38(4):E7. - PubMed
-
- Sorensen BF. Bow hunter’s stroke. Neurosurgery. 1978;2(3):259–261. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

