Corneal ulcers with non-infectious appearance caused by nasolacrimal duct obstruction or canaliculitis
- PMID: 35856006
- PMCID: PMC9287623
- DOI: 10.1016/j.ajoc.2022.101651
Corneal ulcers with non-infectious appearance caused by nasolacrimal duct obstruction or canaliculitis
Abstract
Purpose: To describe the clinical features of corneal ulcers with non-infectious appearance due to nasolacrimal disease in a retrospective case series.
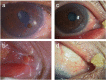
Observations: Eight eyes of 8 patients (aged 74.4 ± 11.1 years) with corneal disease due to nasolacrimal duct obstruction or canaliculitis, who were treated between October 2013 and December 2020 at 3 hospitals were included. Patient background, anterior ocular findings, organisms in secretion, and time course during treatment were retrospectively analyzed. The corneal findings were peripheral ulcers (5 cases), phlyctenular keratitis (1 case), and paracentral perforation with slight cellular infiltration (2 cases). All cases were suspected as autoimmune disease-related-corneal ulcers because of the pathogenic region and clinical appearance and later diagnosed as corneal disorders derived from nasolacrimal duct obstruction or canaliculitis. The autoimmune disease-like appearance and purulent secretion connecting the punctum with/without swelling were characteristic. The most common microorganism detected in the purulent secretions was Streptococcus spp.. The resolution of corneal lesions needed steroid eye drops with antibiotic eye drops. Two patients required a superficial corneal transplantation. The extraction of nasolacrimal calculus, punctal tube insertion, or dacryocystorhinostomy was necessary for complete healing of ocular surface disease.
Conclusions and importance: Nasolacrimal duct diseases cause corneal disorders without bacterial colonization and growth. When corneal ulcers resemble autoimmune disease in shape and are not accompanied by systemic disease, attention should be paid to nasolacrimal duct obstruction or canaliculitis.
Keywords: Canaliculitis; Corneal perforation; Corneal ulcer; Nasolacrimal duct obstruction.
© 2022 The Authors.
Figures
Similar articles
-
Bacteriology of the conjunctiva in pre-cataract surgery patients with occluded nasolacrimal ducts and the operation outcomes in Japanese patients.BMC Ophthalmol. 2017 Feb 20;17(1):15. doi: 10.1186/s12886-017-0410-x. BMC Ophthalmol. 2017. PMID: 28219366 Free PMC article.
-
Monocanalicular intubation with Monoka tubes for the treatment of congenital nasolacrimal duct obstruction.Ophthalmology. 1998 Feb;105(2):336-41. doi: 10.1016/s0161-6420(98)93445-5. Ophthalmology. 1998. PMID: 9479296
-
Microbiological spectrum of microbial keratitis in patients presenting with nasolacrimal duct obstruction.Eur J Ophthalmol. 2021 Jul;31(4):1720-1724. doi: 10.1177/1120672120940574. Epub 2020 Jul 3. Eur J Ophthalmol. 2021. PMID: 32615806
-
Acute Sterile Canaliculitis: A Case Report and Review of the Literature.Ophthalmic Plast Reconstr Surg. 2019 Jan/Feb;35(1):e8-e9. doi: 10.1097/IOP.0000000000001275. Ophthalmic Plast Reconstr Surg. 2019. PMID: 30407997 Review.
-
Insights in the treatment of congenital nasolacrimal duct obstruction.Rom J Ophthalmol. 2017 Apr-Jun;61(2):101-106. doi: 10.22336/rjo.2017.19. Rom J Ophthalmol. 2017. PMID: 29450381 Free PMC article. Review.
Cited by
-
Lacrimal drainage pathway disease-associated keratopathy effectively diagnosed with dacryoendoscopy: a report of two cases.BMC Ophthalmol. 2025 Apr 7;25(1):178. doi: 10.1186/s12886-025-04021-y. BMC Ophthalmol. 2025. PMID: 40197220 Free PMC article.
-
Peripheral ulcerative keratitis secondary to chronic Citrobacter koseri canaliculitis.Taiwan J Ophthalmol. 2023 Apr 17;13(3):376-379. doi: 10.4103/tjo.TJO-D-22-00144. eCollection 2023 Jul-Sep. Taiwan J Ophthalmol. 2023. PMID: 38089517 Free PMC article.
References
-
- Kim H.B., Ostler H.B. Marginal corneal ulcer. Arch Ophthalmol. 1977;95(3):454–455. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

