Environmental Noise and Effects on Sleep: An Update to the WHO Systematic Review and Meta-Analysis
- PMID: 35857401
- PMCID: PMC9272916
- DOI: 10.1289/EHP10197
Environmental Noise and Effects on Sleep: An Update to the WHO Systematic Review and Meta-Analysis
Abstract
Background: Nighttime noise carries a significant disease burden. The World Health Organization (WHO) recently published guidelines for the regulation of environmental noise based on a review of evidence published up to the year 2015 on the effects of environmental noise on sleep.
Objectives: This systematic review and meta-analysis will update the WHO evidence review on the effects of environmental noise on sleep disturbance to include more recent studies.
Methods: Investigations of self-reported sleep among residents exposed to environmental traffic noise at home were identified using Scopus, PubMed, Embase, and PsycINFO. Awakenings, falling asleep, and sleep disturbance were the three outcomes included. Extracted data were used to derive exposure-response relationships for the probability of being highly sleep disturbed by nighttime noise [average outdoor A-weighted noise level () 2300-0700 hours] for aircraft, road, and rail traffic noise, individually. The overall quality of evidence was assessed using Grading of Recommendations, Assessment, Development, and Evaluations (GRADE) criteria.
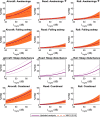
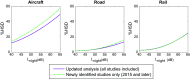
Results: Eleven studies ( responses) were included in addition to 25 studies ( responses) from the original WHO analysis. When sleep disturbance questions specifically mentioned noise as the source of disturbance, there was moderate quality of evidence for the probability of being highly sleep disturbed per 10-dB increase in for aircraft [; 95% confidence interval (CI): 2.01, 2.36], road (; 95% CI: 2.28, 2.79), and railway (; 95% CI: 2.57, 3.43) noise. When noise was not mentioned, there was low to very low quality of evidence for being sleep disturbed per 10-dB increase in for aircraft (; 95% CI: 1.20, 1.93), road (; 95% CI: 1.08, 1.21), and railway (; 95% CI: 0.91, 1.49) noise. Compared with the original WHO review, the exposure-response relationships closely agreed at low (40 dB ) levels for all traffic types but indicated greater disturbance by aircraft traffic at high noise levels. Sleep disturbance was not significantly different between European and non-European studies.
Discussion: Available evidence suggests that transportation noise is negatively associated with self-reported sleep. Sleep disturbance in this updated meta-analysis was comparable to the original WHO review at low nighttime noise levels. These low levels correspond to the recent WHO noise limit recommendations for nighttime noise, and so these findings do not suggest these WHO recommendations need revisiting. Deviations from the WHO review in this updated analysis suggest that populations exposed to high levels of aircraft noise may be at greater risk of sleep disturbance than determined previously. https://doi.org/10.1289/EHP10197.
Figures
![Figure 1 depicts a flowchart with three steps: identification, screening, and inclusion. Step 1: Identification: The previous version of the review included 25 studies. 21 records were published in June 2019 and earlier identified from scoping reviews (van Kamp and others [reference 28]). Records from databases ranging from July 2019 to December 2021 were identified, including 46 from SCOPUS, 40 from PubMed, 12 from PsycINFO, and 60 from Embase. 76 duplicate records were removed from the screening. There are two manual identifications of relevant scientific projects which are not identified by the electronic literature search. Step 2: Screening: 103 records were screened, from which 69 records were excluded. 34 reports were sought for retrieval and assessed for eligibility, excluding 8 reports related to noise which were not specific to home address, 1 report related to daytime noise only, 5 reports related to not self-reported sleep, 8 reports related to ineligible sleep outcome or response scale, and 1 report which was included in the previous meta-analysis. For new studies identified via other methods, 2 reports were sought for retrieval and 2 studies were assessed for eligibility. Step 3: Included: 13 new studies were included in the review. 38 studies were included in the review, excluding 1 study from the meta-analysis and 1 report of noise exposure specific to a home address that is unavailable from the meta-analysis. A total of 36 studies were included in the meta-analysis.](https://cdn.ncbi.nlm.nih.gov/pmc/blobs/60bd/9272916/57937b4f5fb4/ehp10197_f1.gif)
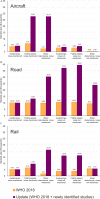
![Figure 3 is a forest plot, plotting study of subgroup and odds ratio inverse variance, random, 95 percent confidence intervals year, including (bottom to top) Aircraft: Non noise specific: Total (95 percent confidence intervals), 2.30 (1.87, 2.82); Test for subgroup differences: Chi squared equals 10.85, degrees of freedom equals 1 (uppercase p equals 0.0010); I squared equals 90.8 precent. Test for overall effect: uppercase z equals 7.91 (uppercase p equals 0.00001); Heterogeneity: Tau squared equals 0.15; Chi squared equals 190.63, degrees of freedom equals 17 (uppercase p equals 0.00001); I squared equals 91 precent. Test for overall effect: uppercase z equals 2.29 (uppercase p equals 0.02); Heterogeneity: Tau squared equals 0.12; Chi squared equals 23.78, degrees of freedom equals 6 (uppercase p equals 0.0006); I squared equals 75 precent; Subtotal (95 percent confidence intervals), 1.48 [1.06, 2.06]; Nguyen and others [32], 2.74 [1.99, 3.77] 2020; Rocha and others [45], 1.49 [1.08, 2.07] 2019; Basner and others [20], 24.43 [0.38, 1582.99] 2019; Carugno and others [35], 1.40 [0.79, 2.50] 2018; Brink [55], 0.33 [0.06, 1.73] 2011; Brink and others (2001 data) [55], 1.22 [0.94, 1.58] 2005; Brink and others (2003 data) [55], 1.20 [0.92, 1.57] 2005; Aircraft: Noise specific: Test for overall effect: uppercase z equals 10.16 (uppercase p less than 0.00001); Heterogeneity: Tau squared equals 0.09; Chi squared equals 87.86, degrees of freedom equals 10 (uppercase p equals 0.0001); I squared equals 89 precent; Subtotal (95% CI), 2.84 [2.32, 3.47]; Nguyen and others [32], 6.90 [4.78, 9.96] 2020; Rocha and others [45], 3.72 [2.61, 5.31] 2019; Brink and others [46], 4.48 [3.76, 5.32] 2019; Civil Air Authority [41], 2.04 [1.47, 2.83] 2017; Yano and others [49] 2.34 [1.69, 3.24] 2015; Nguyen and others [48], 2.70 [2.13, 3.42] 2015; NORAH [42], 2.83 [2.68, 2.98] 2015; Nguyen et al. [50], 1.14 [0.69, 1.88] 2013; Nguyen and others [51, 52], 1.46 [0.99, 2.16] 2011; Schreckenberg and others [54], 2.44 [2.05, 2.91] 2009; and Nguyen and others [53], 4.65 [2.96, 7.31] 2009 (y-axis) across less disturbed, ranging from 0.05 to 0.2 in increments of 0.15 and 0.2 to 1 in increments of 0.8, and more disturbed, ranging from 1 to 5 in increments of 4 and 5 to 20 in increments of 15 (x-axis) for Risk of bias, including selection bias, exposure assessment bias, bias due to confounding, and reporting bias.](https://cdn.ncbi.nlm.nih.gov/pmc/blobs/60bd/9272916/950b668c6187/ehp10197_f3.gif)
![Figure 4 is a forest plot, plotting Study or subgroup and odds ratio inverse variance, random, 95 percent confidence intervals year, including (bottom to top) Road: Non noise specific: Total (95 percent confidence intervals), 1.80 [1.50, 2.17]; Test for subgroup differences: Chi squared equals 43.62, degrees of freedom equals 1 (uppercase p equals 0.00001); I squared equals 97.7 precent. Test for overall effect: uppercase z equals 6.26 (uppercase p equals 0.00001); Heterogeneity: Tau squared equals 0.16; Chi squared equals 466.45, degrees of freedom equals 21 (uppercase p equals 0.00001); I squared equals 95 precent. Test for overall effect: uppercase z equals 3.14 (uppercase p equals 0.002); Heterogeneity: Tau squared equals 0.01; Chi squared equals 17.44, degrees of freedom equals 6 (uppercase p equals 0.0008); I squared equals 66 precent; Subtotal (95 percent confidence intervals), 1.13 [1.05, 1.22]; Bartels and others [47], 1.01 [0.88, 1.15] 2021; Martens and others [34], 1.10 [1.02, 1.18] 2018; Evandt and others [37], 1.20 [1.11, 1.30] 2017; Bodin and others [33], 1.12 [0.96, 1.31] 2015; Frei and others [63], 1.22 [1.03, 1.44] 2014; Halonen and others [64], 0.99 [0.88, 1.12] 2012; Brink [56], 1.43 [1.18, 1.72] 2011; Road: Noise specific: Test for overall effect: uppercase z equals 8.28 (uppercase p equals 0.00001); Heterogeneity: Tau squared equals 0.11; Chi squared equals 95.40, degrees of freedom equals 14 (uppercase p less than 0.00001); I squared equals 85 precent; Subtotal (95 percent confidence intervals), 2.32 [1.90, 2.84]; Brink and others [46], 2.56 [2.27, 2.90] 2019; Evandt and others [37], 3.19 [2.68, 3.78] 2017; NORAH [42], 1.92 [1.63, 2.26] 2015; Brown and others [60], 2.55 [2.15, 3.02] 2015; Bodin and others [33], 2.44 [1.84, 3.24] 2015; Phan and others Thai Nguyen [57], 19.93 [8.27, 48.02] 2010; Phan and others Hue [57], 1.49 [0.98, 2.26] 2010; Phan and others Ho Chi Minh City [57] 1.13 [0.76, 1.70] 2010; Phan and others Hanoi [57], 1.28 [0.86, 1.90] 2010; Phan and others Da Nang [57], 12.49 [4.64, 33.60] 2010; Hong and others [61], 1.26 [0.74, 2.14] 2010; Ristovska and others [62], 2.45 [1.71, 3.50] 2009; Sato and others Kumamoto [59], 1.41 [0.94, 2.12] 2002; Sato and others Gothenburg [57], 3.50 [2.34, 5.22] 2002; and Sato and others Sapporo [59], 2.66 [1.20, 5.89] 2002 (y-axis) across Less disturbed, ranging from 0.02 to 0.1 in increments of 0.1 and 0.1 to 1 in increments of 0.9, and 1 to 10 in increments of 9 and 10 to 50 in increments of 40 (x-axis) for risk of bias, including selection bias, exposure assessment bias, bias due to confounding, and reporting bias.](https://cdn.ncbi.nlm.nih.gov/pmc/blobs/60bd/9272916/aad0fc18dc7a/ehp10197_f4.gif)
![Figure 5 is a forest plot, plotting Study or subgroup and odds ratio inverse variance, random, 95 percent confidence intervals year, including (bottom to top) Total (95 percent confidence intervals), 2.14 [1.54, 2.97]; Test for subgroup differences: Chi squared equals 62.31, degrees of freedom equals 1 (uppercase p equals 0.00001); I squared equals 98.4 precent. Test for overall effect: uppercase z equals 4.55 (uppercase p equals 0. 00001); Heterogeneity: Tau squared equals 0.32; Chi squared equals 490.79, degrees of freedom equals 11 (uppercase p equals 0.00001); I squared equals 98 precent. Test for overall effect: uppercase z equals 2.44 (uppercase p equals 0.01); Heterogeneity: Tau squared equals 0.00; Chi squared equals 0.39, degrees of freedom equals 3 (uppercase p equals 0.94); I squared equals 0 precent; Subtotal (95 percent confidence intervals), 1.09 [1.02, 1.18]; Evandt and others [37], 1.12 [1.00, 1.25] 2017; Bodin and others [33], 1.09 [0.95, 1.24] 2015; Frei and others [63], 1.06 [0.73, 1.53] 2014; Brink [56], 1.06 [0.92, 1.23] 2011; Railway: Noise specific: Test for overall effect: uppercase z equals 8.97 (uppercase p equals 0.00001); Heterogeneity: Tau squared equals 0.10; Chi squared equals 88.70, degrees of freedom equals 7 (uppercase p less than 0.00001); I squared equals 92 precent; Subtotal (95 percent confidence intervals), 3.01 [2.37, 3.83]; Brink and others [46], 3.43 [3.03, 3.88] 2019; Evandt and others [37], 4.77 [4.02, 5.66] 2017; Bodin and others [33], 5.18 [3.44, 7.79] 2015; NORAH [42], 2.11 [1.85, 2.40] 2015; Schreckenberg and others [66], 3.00 [2.56, 3.50] 2013; Hong and others [61], 2.98 [2.14, 4.17] 2010; Sato and others Hokkaido [65], 2.36 [1.62, 3.44] 2004; and Sato and others Kyushu [65], 1.94 [1.61, 2.34] 2004 (y-axis) across less disturbed, ranging from 0.1 to 0.2 in increments of 0.1, 0.2 to 0.5 in increments of 0.3, and 0.5 to 1 in increments 0.5, and more disturbed, ranging from 1 to 2 in unit increments, 2 to 5 in increments of 3, and 5 to 10 in increments of 5 (x-axis) for risk of bias, including selection bias, exposure assessment bias, bias due to confounding, and reporting bias.](https://cdn.ncbi.nlm.nih.gov/pmc/blobs/60bd/9272916/b48ccdf327e5/ehp10197_f5.gif)

References
-
- Consensus Conference Panel; Watson NF, Badr MS, Belenky G, Bliwise DL, Buxton OM, et al. 2015. Joint Consensus Statement of the American Academy of Sleep Medicine and Sleep Research Society on the recommended amount of sleep for a healthy adult: methodology and discussion. Sleep 38(8):1161–1183, PMID: , 10.5665/sleep.4886. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
