Preferences Elicited and Respected for Seriously Ill Veterans through Enhanced Decision-Making (PERSIVED): a protocol for an implementation study in the Veterans Health Administration
- PMID: 35859140
- PMCID: PMC9296899
- DOI: 10.1186/s43058-022-00321-2
Preferences Elicited and Respected for Seriously Ill Veterans through Enhanced Decision-Making (PERSIVED): a protocol for an implementation study in the Veterans Health Administration
Erratum in
-
Correction: Preferences Elicited and Respected for Seriously Ill Veterans through Enhanced Decision-Making (PERSIVED): a protocol for an implementation study in the Veterans Health Administration.Implement Sci Commun. 2023 Mar 14;4(1):26. doi: 10.1186/s43058-023-00416-4. Implement Sci Commun. 2023. PMID: 36918996 Free PMC article. No abstract available.
Abstract
Background: Empirical evidence supports the use of structured goals of care conversations and documentation of life-sustaining treatment (LST) preferences in durable, accessible, and actionable orders to improve the care for people living with serious illness. As the largest integrated healthcare system in the USA, the Veterans Health Administration (VA) provides an excellent environment to test implementation strategies that promote this evidence-based practice. The Preferences Elicited and Respected for Seriously Ill Veterans through Enhanced Decision-Making (PERSIVED) program seeks to improve care outcomes for seriously ill Veterans by supporting efforts to conduct goals of care conversations, systematically document LST preferences, and ensure timely and accurate communication about preferences across VA and non-VA settings.
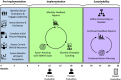
Methods: PERSIVED encompasses two separate but related implementation projects that support the same evidence-based practice. Project 1 will enroll 12 VA Home Based Primary Care (HBPC) programs and Project 2 will enroll six VA Community Nursing Home (CNH) programs. Both projects begin with a pre-implementation phase during which data from diverse stakeholders are gathered to identify barriers and facilitators to adoption of the LST evidence-based practice. This baseline assessment is used to tailor quality improvement activities using audit with feedback and implementation facilitation during the implementation phase. Site champions serve as the lynchpin between the PERSIVED project team and site personnel. PERSIVED teams support site champions through monthly coaching sessions. At the end of implementation, baseline site process maps are updated to reflect new steps and procedures to ensure timely conversations and documentation of treatment preferences. During the sustainability phase, intense engagement with champions ends, at which point champions work independently to maintain and improve processes and outcomes. Ongoing process evaluation, guided by the RE-AIM framework, is used to monitor Reach, Adoption, Implementation, and Maintenance outcomes. Effectiveness will be assessed using several endorsed clinical metrics for seriously ill populations.
Discussion: The PERSIVED program aims to prevent potentially burdensome LSTs by consistently eliciting and documenting values, goals, and treatment preferences of seriously ill Veterans. Working with clinical operational partners, we will apply our findings to HBPC and CNH programs throughout the national VA healthcare system during a future scale-out period.
Keywords: Audit with feedback; End-of-life care; Facilitation; Goals of care conversations; Implementation science; Life-sustaining treatment; Long-term care; Patient decision-making; Patient preferences.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Similar articles
-
Applying the Tailored Implementation in Chronic Diseases framework to inform implementation of the Preferences Elicited and Respected for Seriously Ill Veterans through enhanced decision-making program in the United States Veterans Health Administration.Front Health Serv. 2022 Sep 2;2:935341. doi: 10.3389/frhs.2022.935341. eCollection 2022. Front Health Serv. 2022. PMID: 36925825 Free PMC article.
-
Barriers and facilitators to goals of care conversations with Veteran residents of community nursing homes.J Am Geriatr Soc. 2023 Aug;71(8):2539-2548. doi: 10.1111/jgs.18365. Epub 2023 Apr 10. J Am Geriatr Soc. 2023. PMID: 37036028
-
Implementing goals of care conversations with veterans in VA long-term care setting: a mixed methods protocol.Implement Sci. 2016 Sep 29;11(1):132. doi: 10.1186/s13012-016-0497-0. Implement Sci. 2016. PMID: 27682236 Free PMC article.
-
Using implementation mapping for the adoption and implementation of Target:BP in community health centers.Front Public Health. 2022 Nov 24;10:928148. doi: 10.3389/fpubh.2022.928148. eCollection 2022. Front Public Health. 2022. PMID: 36504969 Free PMC article. Review.
-
Improving Communication About Serious Illness in Primary Care: A Review.JAMA Intern Med. 2016 Sep 1;176(9):1380-7. doi: 10.1001/jamainternmed.2016.3212. JAMA Intern Med. 2016. PMID: 27398990 Review.
Cited by
-
Correction: Preferences Elicited and Respected for Seriously Ill Veterans through Enhanced Decision-Making (PERSIVED): a protocol for an implementation study in the Veterans Health Administration.Implement Sci Commun. 2023 Mar 14;4(1):26. doi: 10.1186/s43058-023-00416-4. Implement Sci Commun. 2023. PMID: 36918996 Free PMC article. No abstract available.
-
Evaluating feedback reports to support documentation of veterans' care preferences in home based primary care.BMC Geriatr. 2024 May 1;24(1):389. doi: 10.1186/s12877-024-04999-y. BMC Geriatr. 2024. PMID: 38693502 Free PMC article.
References
-
- Ersek M, Miller SC, Wagner TH, Thorpe JM, Smith D, Levy CR, et al. Association between aggressive care and bereaved families’ evaluation of end-of-life care for veterans with non-small cell lung cancer who died in Veterans Affairs facilities. Cancer. 2017;123(16):3186–3194. doi: 10.1002/cncr.30700. - DOI - PubMed
-
- Tinetti ME, Naik AD, Dindo L, Costello DM, Esterson J, Geda M, et al. Association of patient priorities-aligned decision-making with patient outcomes and ambulatory health care burden among older adults with multiple chronic conditions: a nonrandomized clinical trial. JAMA Intern Med. 2019. 10.1001/jamainternmed.2019.4235. - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials