Variation in Left Ventricular Assist Device Postdischarge Caregiver Requirements: Results From a Mixed-Methods Study With Equity Implications
- PMID: 35862012
- PMCID: PMC9388601
- DOI: 10.1161/CIRCHEARTFAILURE.122.009583
Variation in Left Ventricular Assist Device Postdischarge Caregiver Requirements: Results From a Mixed-Methods Study With Equity Implications
Abstract
Background: Left ventricular assist device (LVAD) evaluation includes a psychosocial assessment, conducted by social workers (SWs) on the advanced heart failure multidisciplinary team. Postdischarge caregiving plans are central to psychosocial evaluation. Caregiving's relationship with LVAD outcomes is mixed, and testing patients' social resources may disadvantage those from historically undertreated groups. We describe variation in policies defining adequate caregiving plans post-LVAD implant and possible impacts on patients from marginalized groups.
Methods: This was a 2-phase sequential mixed-methods study: (1) phase 1, survey of US-based LVAD SWs, describing assessment structure and policies guiding candidacy outcomes; and (2) phase 2, individual interviews with SWs to further describe how caregiving plan adequacy impacts LVAD candidacy.
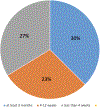
Results: Sixty-seven SWs returned surveys (rr=47%) from unique programs. Caregiving plan inadequacy (n=30) was the most common psychosocial dealbreaker. When asked what duration of caregiving is required, 23% indicated ≥3 months, 27% 4 to 12 weeks, and 30% <4 weeks. Two reported no duration requirement, 6 stated an indefinite 24/7 commitment was necessary. Across 22 interviews, SWs mirrored that caregiving plans were the most common psychosocial contraindication. How caregiving is operationalized varied. Participants voiced a tension between extended caregiving improving outcomes and the sense that some people of color, women, or low socioeconomic status patients struggle to meet stringent requirements.
Conclusions: Policies regarding adequate duration of 24/7 caregiving vary, but inadequate caregiving plans are the most common psychosocial contraindication. Participants worry about patients' ability to meet restrictive requirements, particularly from historically undertreated groups. This highlights a need to operationalize quality caregiving, standardize assessment, and support medically appropriate patients with strained social resources.
Keywords: caregivers; contraindications; health equity; heart failure; social workers.
Figures
Similar articles
-
Caregivers of Patients With Left Ventricular Assist Devices: Possible Impacts on Patients' Mortality and Interagency Registry for Mechanically Assisted Circulatory Support-Defined Morbidity Events.Circ Cardiovasc Qual Outcomes. 2017 Jan;10(1):e002879. doi: 10.1161/CIRCOUTCOMES.116.002879. Circ Cardiovasc Qual Outcomes. 2017. PMID: 28073849
-
Preliminary report on left-ventricular assist devices: are patients' and caregivers' psychosocial needs adequately addressed?G Ital Med Lav Ergon. 2017 Nov;39(2):88-92. G Ital Med Lav Ergon. 2017. PMID: 29916597
-
Assessment of pre-operative psychosocial function among people receiving left ventricular assist devices: A national survey of US LVAD programs.Heart Lung. 2019 Jul-Aug;48(4):302-307. doi: 10.1016/j.hrtlng.2019.02.003. Epub 2019 Mar 22. Heart Lung. 2019. PMID: 30905390
-
Association between psychosocial factors and left ventricular assist device implant outcomes: A systematic review.Gen Hosp Psychiatry. 2024 Sep-Oct;90:132-140. doi: 10.1016/j.genhosppsych.2024.08.007. Epub 2024 Aug 20. Gen Hosp Psychiatry. 2024. PMID: 39180882
-
The Perceptions of Important Elements of Caregiving for a Left Ventricular Assist Device Patient: A Qualitative Meta-Synthesis.J Cardiovasc Nurs. 2016 May-Jun;31(3):215-25. doi: 10.1097/JCN.0000000000000242. J Cardiovasc Nurs. 2016. PMID: 25882647 Free PMC article. Review.
Cited by
-
Disparities in Adult Patient Selection for Extracorporeal Membrane Oxygenation in the United States: A Population-Level Study.Ann Am Thorac Soc. 2023 Aug;20(8):1166-1174. doi: 10.1513/AnnalsATS.202212-1029OC. Ann Am Thorac Soc. 2023. PMID: 37021958 Free PMC article.
-
Integrating Palliative Care into the Management of Heart Failure with Reduced Ejection Fraction: A Practice Pearl.Heart Int. 2023 Jun 13;17(1):5-7. doi: 10.17925/HI.2023.17.1.5. eCollection 2023. Heart Int. 2023. PMID: 37456350 Free PMC article.
References
-
- Miller LW, Rogers JG. Evolution of Left Ventricular Assist Device Therapy for Advanced Heart Failure: A Review. JAMA Cardiol. 2018;3(7):650–658. - PubMed
-
- MacIver J, Ross HJ. Quality of Life and Left Ventricular Assist Device Support. Circulation. 2012;126(7):866–874. - PubMed
-
- Grady KL, Meyer PM, Dressler D, Mattea A, Chillcott S, Loo A, White-Williams C, Todd B, Ormaza S, Kaan A, et al. Longitudinal change in quality of life and impact on survival after left ventricular assist device implantation. Ann Thorac Surg. 2004;77(4):1321–1327. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical