Cost-Effectiveness of Mobile Stroke Unit Care in Norway
- PMID: 35862205
- PMCID: PMC9508956
- DOI: 10.1161/STROKEAHA.121.037491
Cost-Effectiveness of Mobile Stroke Unit Care in Norway
Abstract
Background: Acute ischemic stroke treatment in mobile stroke units (MSUs) reduces time-to-treatment and increases thrombolytic rates, but implementation requires substantial investments. We wanted to explore the cost-effectiveness of MSU care incorporating novel efficacy data from the Norwegian MSU study, Treat-NASPP (the Norwegian Acute Stroke Prehospital Project).
Methods: We developed a Markov model linking improvements in time-to-treatment and thrombolytic rates delivered by treatment in an MSU to functional outcomes for the patients in a lifetime perspective. We estimated incremental costs, health benefits, and cost-effectiveness of MSU care as compared with conventional care. In addition, we estimated a minimal MSU utilization level for the intervention to be cost-effective in the publicly funded health care system in Norway.
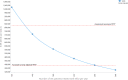
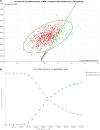
Results: MSU care was associated with an expected quality-adjusted life-year-gain of 0.065 per patient, compared with standard care. Our analysis suggests that about 260 patients with ischemic stroke need to be treated with MSU annually to result in an incremental cost-effectiveness ratio of about NOK385 000 (US$43 780) per quality-adjusted life-year for MSU compared with standard care. The incremental cost-effectiveness ratio varies between some NOK1 000 000 (US$113 700) per quality-adjusted life-year if an MSU treats 100 patients per year and to about NOK340 000 (US$38 660) per quality-adjusted life-year if 300 patients with acute ischemic stroke are treated.
Conclusions: MSU care in Norwegian settings is potentially cost-effective compared with conventional care, but this depends on a relatively high annual number of treated patients with acute ischemic stroke per vehicle. These results provide important information for MSU implementation in government-funded health care systems.
Keywords: ischemic stroke; repefusion; thrombectomy; time-to-treatment; triage.
Figures
References
-
- Hamidi V, Wisløff T, Ringerike T, Linnestad KK, Harboe I, Klemp M. Treatment of patients with acute stroke in stroke units (with or without early supported discharge). Report from norwegian knowledge centre for the health services (nokc) no. 18-2010. 2010 - PubMed
-
- Fjærtoft H, Skogseth-Stephani R, Indredavik B, Bjerkvik TF, Varmdal T. Norsk hjerneslagregister. Norwegian stroke registry, annual report for 2019. 2020
-
- Turc G, Bhogal P, Fischer U, Khatri P, Lobotesis K, Mazighi M, Schellinger PD, Toni D, de Vries J, White P, et al. European Stroke Organisation (ESO) - European Society for Minimally Invasive Neurological Therapy (ESMINT) guidelines on mechanical thrombectomy in acute ischaemic strokeendorsed by Stroke Alliance for Europe (SAFE). Eur Stroke J. 2019;4:6–12. doi: 10.1177/2396987319832140 - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

