Preventing nausea and vomiting after gynecological laparoscopic surgery by patient-controlled intravenous analgesia with a naloxone admixture: A randomized controlled trial
- PMID: 35866767
- PMCID: PMC9302326
- DOI: 10.1097/MD.0000000000029584
Preventing nausea and vomiting after gynecological laparoscopic surgery by patient-controlled intravenous analgesia with a naloxone admixture: A randomized controlled trial
Abstract
Background: Opioid-induced nausea and vomiting are common side effects of patient-controlled intravenous analgesia (PCIA). This study aimed to explore the inhibitory effect of a naloxone admixture on the incidence of sufentanil-induced postoperative nausea and vomiting (PONV).
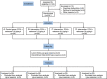
Methods: A total of 132 Uyghur American Society of Anesthesiologists I and II patients scheduled to undergo elective gynecological laparoscopic surgery were recruited; among these, 120 patients were enrolled and randomly allocated into 4 groups: patients receiving PCIA but no naloxone were included in the control group (group A); patients receiving PCIA with a low-dose naloxone admixture at 0.2 μg·kg-1·h-1 were included in group B; patients receiving PCIA with naloxone admixture at 0.4 μg·kg-1·h-1 were included in group C; patients receiving PCIA with naloxone admixture at 0.6 μg·kg-1·h-1 were included in group D. All patients were administered sufentanil at 0.04 kg-1·h-1, butorphanol at 2 kg-1·h-1, and dexmedetomidine at 0.08 kg-1·h-1 using a PCIA device within 2 days of surgery. The occurrence of nausea and vomiting, visual analogue scores for pain intensity, mean arterial pressure, heart rate, oxygen saturation, pruritus, lethargy, respiratory depression, etc, was recorded at 2, 8, 12, 24, and 48 hours postoperatively.
Results: There was a significant difference in the PONV scores between the groups at 8, 12, and 24 hours after surgery (P < 0.01). At 8 and 12 hours, the score of group C/D was significantly lower than that of group A/B (P < 0.01). At 24 hours after surgery, the PONV score of group B/C/D was significantly lower than that of group A (P < 0.01). No significant difference was observed in the general data and visual analogue scores for postoperative pain between the 4 groups.
Conclusion: Naloxone admixture administered at 0.4 to 0.6 μg·kg-1·h-1 can exert an effective inhibitory effect on the incidence and intensity of PONV in gynecological laparoscopic surgery.
Copyright © 2022 the Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
Similar articles
-
Epidural naloxone reduces postoperative nausea and vomiting in patients receiving epidural sufentanil for postoperative analgesia.Br J Anaesth. 2007 Aug;99(2):270-5. doi: 10.1093/bja/aem146. Epub 2007 Jun 7. Br J Anaesth. 2007. PMID: 17561515 Clinical Trial.
-
Effect of Dexmedetomidine Alone for Intravenous Patient-Controlled Analgesia After Gynecological Laparoscopic Surgery: A Consort-Prospective, Randomized, Controlled Trial.Medicine (Baltimore). 2016 May;95(19):e3639. doi: 10.1097/MD.0000000000003639. Medicine (Baltimore). 2016. PMID: 27175680 Free PMC article. Clinical Trial.
-
Adding dexmedetomidine to morphine-based analgesia reduces early postoperative nausea in patients undergoing gynecological laparoscopic surgery: a randomized controlled trial.BMC Anesthesiol. 2020 Jan 8;20(1):11. doi: 10.1186/s12871-019-0928-y. BMC Anesthesiol. 2020. PMID: 31914930 Free PMC article. Clinical Trial.
-
Esketamine combined with sufentanil versus sufentanil in patient-controlled intravenous analgesia: a meta-analysis.Front Pharmacol. 2024 Feb 7;15:1247646. doi: 10.3389/fphar.2024.1247646. eCollection 2024. Front Pharmacol. 2024. PMID: 38384296 Free PMC article. Review.
-
The Effect of Dexmedetomidine on Postoperative Nausea and Vomiting in Patients Undergoing Thoracic Surgery-A Meta-Analysis of a Randomized Controlled Trial.Front Surg. 2022 Mar 31;9:863249. doi: 10.3389/fsurg.2022.863249. eCollection 2022. Front Surg. 2022. PMID: 35433815 Free PMC article.
Cited by
-
Efficacy and safety of patient-controlled intravenous analgesia after APS team standardized postoperative pain management: A 6-year experience of an acute pain service in 107802 Chinese patients.Heliyon. 2024 Jan 19;10(2):e24387. doi: 10.1016/j.heliyon.2024.e24387. eCollection 2024 Jan 30. Heliyon. 2024. PMID: 38312661 Free PMC article.
-
Analgesic effect of ultrasound-guided bilateral transversus abdominis plane block in laparoscopic gastric cancer.World J Gastrointest Surg. 2023 Oct 27;15(10):2171-2178. doi: 10.4240/wjgs.v15.i10.2171. World J Gastrointest Surg. 2023. PMID: 37969718 Free PMC article.
-
Effects of perioperative low-dose naloxone on the immune system in patients undergoing laparoscopic-assisted total gastrectomy: a randomized controlled trial.BMC Anesthesiol. 2024 May 8;24(1):172. doi: 10.1186/s12871-024-02524-7. BMC Anesthesiol. 2024. PMID: 38720250 Free PMC article. Clinical Trial.
-
Penehyclidine for Prevention of Postoperative Nausea and Vomiting in Patients Undergoing Gynecological Laparoscopic Surgery Under Combined Intravenous and Inhalation Anesthesia: A Randomized, Double-Blind, Placebo-Controlled Trial.Drug Des Devel Ther. 2024 Mar 1;18:685-697. doi: 10.2147/DDDT.S453327. eCollection 2024. Drug Des Devel Ther. 2024. PMID: 38445065 Free PMC article. Clinical Trial.
-
Opioids With or Without Low-Dose Naloxone During the Perioperative Period: A Systematic Review With Meta-Analysis.Pain Res Manag. 2025 Feb 23;2025:8380502. doi: 10.1155/prm/8380502. eCollection 2025. Pain Res Manag. 2025. PMID: 40027404 Free PMC article.
References
-
- Barratt DT, Sia AT, Tan EC, et al. . Innate immune and neuronal genetic markers are highly predictive of postoperative pain and morphine patient-controlled analgesia requirements in Indian but not Chinese or Malay hysterectomy patients. Pain Med. 2021;11:2648–2660. - PubMed
-
- Andres J, Pogatzki-Zahn E, Huygen F, et al. . Controlling acute pain to improve the quality of postoperative pain management: an update from the European Society of Regional Anesthesia meeting held in Maastricht (September 2016). Pain Manag. 2017;7:513–22. - PubMed
-
- Monitto CL, Kost-Byerly S, White E, et al. . The optimal dose of prophylactic intravenous naloxone in ameliorating opioid-induced side effects in children receiving intravenous patient-controlled analgesia morphine for moderate to severe pain: a dose finding study. Anesth Analg. 2011;113:834–42. - PMC - PubMed
-
- Hill RP, Lubarsky DA, Phillips-Bute B, et al. . Cost-effectiveness of prophylactic antiemetic therapy with ondansetron, droperidol, or placebo. Anesthesiology. 2000;92:958–67. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources