Prediction of Mortality and Major Adverse Kidney Events in Critically Ill Patients With Acute Kidney Injury
- PMID: 35868537
- PMCID: PMC9780161
- DOI: 10.1053/j.ajkd.2022.06.004
Prediction of Mortality and Major Adverse Kidney Events in Critically Ill Patients With Acute Kidney Injury
Erratum in
-
Erratum Regarding "Prediction of Mortality and Major Adverse Kidney Events in Critically Ill Patients With Acute Kidney Injury" [Am J Kidney Dis. 2023;81(1):36-47].Am J Kidney Dis. 2023 Sep;82(3):377-378. doi: 10.1053/j.ajkd.2023.07.001. Am J Kidney Dis. 2023. PMID: 37612004 Free PMC article. No abstract available.
Abstract
Rationale & objective: Risk prediction tools for assisting acute kidney injury (AKI) management have focused on AKI onset but have infrequently addressed kidney recovery. We developed clinical models for risk stratification of mortality and major adverse kidney events (MAKE) in critically ill patients with incident AKI.
Study design: Multicenter cohort study.
Setting & participants: 9,587 adult patients admitted to heterogeneous intensive care units (ICUs; March 2009 to February 2017) who experienced AKI within the first 3 days of their ICU stays.
Predictors: Multimodal clinical data consisting of 71 features collected in the first 3 days of ICU stay.
Outcomes: (1) Hospital mortality and (2) MAKE, defined as the composite of death during hospitalization or within 120 days of discharge, receipt of kidney replacement therapy in the last 48 hours of hospital stay, initiation of maintenance kidney replacement therapy within 120 days, or a ≥50% decrease in estimated glomerular filtration rate from baseline to 120 days from hospital discharge.
Analytical approach: Four machine-learning algorithms (logistic regression, random forest, support vector machine, and extreme gradient boosting) and the SHAP (Shapley Additive Explanations) framework were used for feature selection and interpretation. Model performance was evaluated by 10-fold cross-validation and external validation.
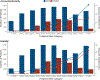
Results: One developed model including 15 features outperformed the SOFA (Sequential Organ Failure Assessment) score for the prediction of hospital mortality, with areas under the curve of 0.79 (95% CI, 0.79-0.80) and 0.71 (95% CI, 0.71-0.71) in the development cohort and 0.74 (95% CI, 0.73-0.74) and 0.71 (95% CI, 0.71-0.71) in the validation cohort (P < 0.001 for both). A second developed model including 14 features outperformed KDIGO (Kidney Disease: Improving Global Outcomes) AKI severity staging for the prediction of MAKE: 0.78 (95% CI, 0.78-0.78) versus 0.66 (95% CI, 0.66-0.66) in the development cohort and 0.73 (95% CI, 0.72-0.74) versus 0.67 (95% CI, 0.67-0.67) in the validation cohort (P < 0.001 for both).
Limitations: The models are applicable only to critically ill adult patients with incident AKI within the first 3 days of an ICU stay.
Conclusions: The reported clinical models exhibited better performance for mortality and kidney recovery prediction than standard scoring tools commonly used in critically ill patients with AKI in the ICU. Additional validation is needed to support the utility and implementation of these models.
Plain-language summary: Acute kidney injury (AKI) occurs commonly in critically ill patients admitted to the intensive care unit (ICU) and is associated with high morbidity and mortality rates. Prediction of mortality and recovery after an episode of AKI may assist bedside decision making. In this report, we describe the development and validation of a clinical model using data from the first 3 days of an ICU stay to predict hospital mortality and major adverse kidney events occurring as long as 120 days after hospital discharge among critically ill adult patients who experienced AKI within the first 3 days of an ICU stay. The proposed clinical models exhibited good performance for outcome prediction and, if further validated, could enable risk stratification for timely interventions that promote kidney recovery.
Keywords: AKI staging; Mortality; acute kidney injury (AKI); clinical decision making; critically ill patients; intensive care unit (ICU); kidney recovery; machine learning; major adverse kidney events (MAKE); renal prognosis; risk prediction tool; risk stratification.
Copyright © 2022 National Kidney Foundation, Inc. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
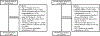
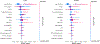
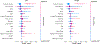
References
-
- Szczech LA, Harmon W, Hostetter TH, et al. World Kidney Day 2009: problems and challenges in the emerging epidemic of kidney disease. Journal of the American Society of Nephrology : JASN. 2009;20:453–455. - PubMed
-
- Rewa O, Bagshaw SM. Acute kidney injury[mdash]epidemiology, outcomes and economics. Nat Rev Nephrol. 2014;10:193–207. - PubMed
-
- Uchino S, Kellum JA, Bellomo R, et al. Acute renal failure in critically ill patients: a multinational, multicenter study. Jama. 2005;294:813–818. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

