Ultrasound gray scale ratio for differential diagnosis of papillary thyroid microcarcinoma from benign micronodule in patients with Hashimoto's thyroiditis
- PMID: 35869461
- PMCID: PMC9306152
- DOI: 10.1186/s12902-022-01028-0
Ultrasound gray scale ratio for differential diagnosis of papillary thyroid microcarcinoma from benign micronodule in patients with Hashimoto's thyroiditis
Abstract
Background: To investigate the diagnostic value of ultrasound gray scale ratio (UGSR) in differentiating papillary thyroid microcarcinomas (PTMCs) from benign micronodules (BMNs) in patients with Hashimoto's thyroiditis (HT).
Methods: The ultrasound images of 285 PTMCs (from 247 patients) and 173 BMNs (from 140 patients) in the HT group, as well as 461 PTMCs (from 417 patients) and 234 BMNs (from 197 patients) in the non-HT group were retrospectively analyzed. The diagnosis of all cases was confirmed by histopathological examinations. The gray scale values of the nodules and surrounding thyroid tissues were measured and subsequently the UGSRs were calculated. Receiver operating characteristic curve analysis was used to determine the area under the curve (AUC), optimal UGSR threshold, sensitivity and specificity in differentiating PTMCs and BMNs in the two groups.
Results: The UGSR of PTMC and BMN was 0.52 ± 0.12 and 0.85 ± 0.24 in the HT group (P < 0.001), and 0.57 ± 0.13 and 0.87 ± 0.20 in the non-HT group (P < 0.001), respectively. The difference in PTMC-UGSR was significant between the two groups (P < 0.001), whereas BMN-UGSR did not differ between the two groups (P = 0.416). The AUC, optimal UGSR threshold, sensitivity and specificity of UGSR for differentiating PTMC and BMN in the HT and non-HT group were 0.890 versus 0.901, 0.68 versus 0.72, 91.23% versus 90.67%, and 77.46% versus 82.05%, respectively.
Conclusions: The USGR of the HT group was lower than that of the non-HT group. Moreover, UGSR exhibited important diagnostic value in differentiating PTMC from BMN in both HT and non-HT groups.
Keywords: Echogenicity; Hashimoto’s thyroiditis; Papillary thyroid microcarcinoma; Thyroid nodule; ultrasound gray scale ratio.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that there is no conflict of interest.
Figures




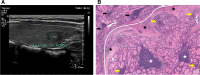
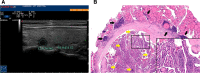


References
MeSH terms
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

