Performance of PRECISE-DAPT and Age-Bleeding-Organ Dysfunction Score for Predicting Bleeding Complication During Dual Antiplatelet Therapy in Chinese Elderly Patients
- PMID: 35872883
- PMCID: PMC9304588
- DOI: 10.3389/fcvm.2022.910805
Performance of PRECISE-DAPT and Age-Bleeding-Organ Dysfunction Score for Predicting Bleeding Complication During Dual Antiplatelet Therapy in Chinese Elderly Patients
Abstract
Background: Recently, the Age-Bleeding-Organ Dysfunction (ABO) algorithm was recommended by the Asian Pacific Society of Cardiology Consensus as a binary approach to evaluate bleeding risk. This analysis made comparison of the predictive performances between the PRECISE-DAPT and ABO bleeding score in identifying the risk of 12-months major bleeding in Chinese elderly patients over 65 years old patients who underwent percutaneous coronary intervention (PCI) during dual-antiplatelet therapy period.
Methods: A total of 2,037 elderly coronary artery disease (CAD) patients (≥65 years) receiving dual antiplatelet therapy (DAPT) after PCI were enrolled in the study. The predictive accuracy of the two bleeding risk scores (PRECISE-DAPT and ABO) was compared for identifying the risk of bleeding during the dual-antiplatelet therapy in patients who underwent PCI. Major clinically relevant bleeding events were defined according to the Bleeding Academic Research Consortium (BARC) criteria.
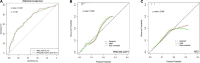
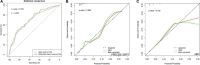
Results: The PRECISE-DAPT score in the no bleeding, BARC = 1 bleeding, BARC ≥ 2 bleeding patients was 23.55 ± 10.46, 23.23 ± 10.03, and 33.54 ± 14.33 (p < 0.001), respectively. Meanwhile, the ABO score in the three groups was 0.72 ± 0.80, 0.69 ± 0.81, and 1.49 ± 0.99 (p < 0.001), respectively. The C-statistic of the PRECISE-DAPT model for prediction of BARC ≥ 2 bleeding in overall patients was 0.717 (95% CI, 0.656-0.777) and 0.720 (95% CI, 0.656-0.784) in acute coronary syndrome (ACS) patients. Similar discriminatory capacity was demonstrated in the ABO risk score [overall, patients, AUC: 0.712 (95% CI, 0.650-0.774); ACS patients, AUC: 0.703 (95% CI, 0.634-0.772)]. No differences were observed when the ABO model was in comparison with the PRECISE-DAPT model, regardless in overall patients (z = -0.199, p = 0.842) or ACS patients (z = -0.605, p = 0.545). The calibration for BARC ≥ 2 bleeding of the PRECISE-DAPT and ABO score were acceptable, regardless in overall patients [goodness-of-fit (GOF) Chi-square = 0.432 and 0.001, respectively; p-value = 0.806 and 0.999, respectively] or ACS patients (GOF Chi-square = 0.008 and 0.580, respectively; p-value = 0.996 and 0.748, respectively).
Conclusion: No matter of clinical presentation in Asian 65-years older patients with DAPT, the PRECISE-DAPT, and ABO scores had the similar discriminative ability for 12-months BARC ≥ 2 bleeding. Considering the simplicity and reliability, the PRECISE-DAPT score might be more clinically applicable in the overall population and ACS patients in bleeding prediction.
Keywords: ABO score; PRECISE-DAPT; bleeding risk scores; dual-antiplatelet therapy; percutaneous coronary intervention.
Copyright © 2022 Dong, Lu, Wensen, Fuzhong, Khalid, Xiaoyu, Guangjuan, Yanxia, Yufeng, Xinjian, Leilei and Junhong.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
-
- Mensah GA, Roth GA, Fuster V. The global burden of cardiovascular diseases and risk factors: 2020 and beyond. J Am Coll Cardiol. (2019) 74:2529–32. - PubMed
-
- Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, et al. 2019 ESC Guidelines for the diagnosis and management of chronic coronary syndromes the task force for the diagnosis and management of chronic coronary syndromes of the European society of cardiology (ESC). Eur Heart J. (2020) 41:407–77. - PubMed
-
- Choi SY, Kim MH, Cho YR, Sung Park J, Min Lee K, Park TH, et al. Performance of PRECISE-DAPT score for predicting bleeding complication during dual antiplatelet therapy. Circ Cardiovasc Interv. (2018) 11:e006837. - PubMed
-
- Sandhu K, Nadar SK. Percutaneous coronary intervention in the elderly. Int J Cardiol. (2015) 199:342–55. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

