Virulence Factors of Pseudomonas Aeruginosa and Antivirulence Strategies to Combat Its Drug Resistance
- PMID: 35873152
- PMCID: PMC9299443
- DOI: 10.3389/fcimb.2022.926758
Virulence Factors of Pseudomonas Aeruginosa and Antivirulence Strategies to Combat Its Drug Resistance
Abstract
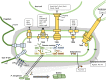
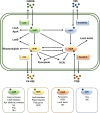
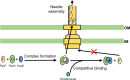
Pseudomonas aeruginosa is an opportunistic pathogen causing nosocomial infections in severely ill and immunocompromised patients. Ubiquitously disseminated in the environment, especially in hospitals, it has become a major threat to human health due to the constant emergence of drug-resistant strains. Multiple resistance mechanisms are exploited by P. aeruginosa, which usually result in chronic infections difficult to eradicate. Diverse virulence factors responsible for bacterial adhesion and colonization, host immune suppression, and immune escape, play important roles in the pathogenic process of P. aeruginosa. As such, antivirulence treatment that aims at reducing virulence while sparing the bacterium for its eventual elimination by the immune system, or combination therapies, has significant advantages over traditional antibiotic therapy, as the former imposes minimal selective pressure on P. aeruginosa, thus less likely to induce drug resistance. In this review, we will discuss the virulence factors of P. aeruginosa, their pathogenic roles, and recent advances in antivirulence drug discovery for the treatment of P. aeruginosa infections.
Keywords: Pseudomonas aeruginosa; antibiotic resistance; antivirulence strategies; infection; virulence factors.
Copyright © 2022 Liao, Huang, Wang, Yao and Lu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Impact of multidrug resistance on the virulence and fitness of Pseudomonas aeruginosa: a microbiological and clinical perspective.Infection. 2024 Aug;52(4):1235-1268. doi: 10.1007/s15010-024-02313-x. Epub 2024 Jul 2. Infection. 2024. PMID: 38954392 Free PMC article. Review.
-
Beyond antibiotics: Emerging antivirulence strategies to combat Pseudomonas aeruginosa in cystic fibrosis.Microb Pathog. 2024 Aug;193:106730. doi: 10.1016/j.micpath.2024.106730. Epub 2024 Jun 6. Microb Pathog. 2024. PMID: 38851361 Review.
-
NirA Is an Alternative Nitrite Reductase from Pseudomonas aeruginosa with Potential as an Antivirulence Target.mBio. 2021 Apr 20;12(2):e00207-21. doi: 10.1128/mBio.00207-21. mBio. 2021. PMID: 33879591 Free PMC article.
-
Pseudomonas aeruginosa Antivirulence Strategies: Targeting the Type III Secretion System.Adv Exp Med Biol. 2022;1386:257-280. doi: 10.1007/978-3-031-08491-1_9. Adv Exp Med Biol. 2022. PMID: 36258075
-
Molecular epidemiology, resistance, and virulence properties of Pseudomonas aeruginosa cross-colonization clonal isolates in the non-outbreak setting.Infect Genet Evol. 2017 Nov;55:288-296. doi: 10.1016/j.meegid.2017.09.010. Epub 2017 Sep 11. Infect Genet Evol. 2017. PMID: 28911852
Cited by
-
Impact of multidrug resistance on the virulence and fitness of Pseudomonas aeruginosa: a microbiological and clinical perspective.Infection. 2024 Aug;52(4):1235-1268. doi: 10.1007/s15010-024-02313-x. Epub 2024 Jul 2. Infection. 2024. PMID: 38954392 Free PMC article. Review.
-
Chemical Optimization of Selective Pseudomonas aeruginosa LasB Elastase Inhibitors and Their Impact on LasB-Mediated Activation of IL-1β in Cellular and Animal Infection Models.ACS Infect Dis. 2023 Feb 10;9(2):270-282. doi: 10.1021/acsinfecdis.2c00418. Epub 2023 Jan 20. ACS Infect Dis. 2023. PMID: 36669138 Free PMC article.
-
Prevalence and Virulence of Commensal Pseudomonas Aeruginosa Isolates from Healthy Individuals in Southern Vietnam (2018-2020).Biomedicines. 2022 Dec 26;11(1):54. doi: 10.3390/biomedicines11010054. Biomedicines. 2022. PMID: 36672562 Free PMC article.
-
The balance between antibiotic resistance and fitness/virulence in Pseudomonas aeruginosa: an update on basic knowledge and fundamental research.Front Microbiol. 2023 Sep 28;14:1270999. doi: 10.3389/fmicb.2023.1270999. eCollection 2023. Front Microbiol. 2023. PMID: 37840717 Free PMC article. Review.
-
Characterization of the dispirotripiperazine derivative PDSTP as antibiotic adjuvant and antivirulence compound against Pseudomonas aeruginosa.Front Microbiol. 2024 Feb 16;15:1357708. doi: 10.3389/fmicb.2024.1357708. eCollection 2024. Front Microbiol. 2024. PMID: 38435690 Free PMC article.
References
-
- Aldrovandi M., Banthiya S., Meckelmann S., Zhou Y., Kuhn H. (2018). Specific Oxygenation of Plasma Membrane Phospholipids by Pseudomonas Aeruginosa Lipoxygenase Induces Structural and Functional Alterations in Mammalian Cells. Biochim. Biophys. Acta 1863 (2), 152–164. doi: 10.1016/j.bbalip.2017.11.005 - DOI - PMC - PubMed
-
- Ali S. O., Yu X. Q., Robbie G. J., Wu Y., Shoemaker K., Yu L., et al. . (2019). Phase 1 Study of MEDI3902, an Investigational Anti-Pseudomonas Aeruginosa PcrV and Psl Bispecific Human Monoclonal Antibody, in Healthy Adults. Clin. Microbiol. Infect 25 (5), 629.e621–629.e626. doi: 10.1016/j.cmi.2018.08.004 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases
Research Materials

