Surgery for Pituitary Tumor Apoplexy Is Associated with Rapid Headache and Cranial Nerve Improvement
- PMID: 35877250
- PMCID: PMC9319222
- DOI: 10.3390/curroncol29070390
Surgery for Pituitary Tumor Apoplexy Is Associated with Rapid Headache and Cranial Nerve Improvement
Abstract
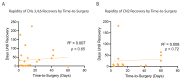
Pituitary tumor apoplexy (PTA) classically comprises sudden-onset headache, loss of vision, ophthalmoparesis, and decreased consciousness. It typically results from hemorrhage and/or infarction within a pituitary adenoma. Presentation is heterologous, and optimal management is debated. The time course of recovery of cranial nerve deficits (CNDs) and headaches is not well established. In this study, a retrospective series of consecutive patients with PTA managed at a single academic institution over a 22-year period is presented. Headaches at the time of surgery were more severe in the early and subacute surgical cohort and improved significantly within 72 h postoperatively (p < 0.01). At one year, 90% of CNDs affecting cranial nerves (CNs) 3, 4, and 6 had recovered, with no differences between early (<4 d), subacute (4−14 d), and delayed (>14 d) time-to-surgery cohorts. Remarkably, half recovered within three days. In total, 56% of CN2 deficits recovered, with the early surgery cohort including more severe deficits and recovering at a lower rate (p = 0.01). No correlation of time-to-surgery and rapidity of recovery of CNDs was observed (p = 0.65, 0.72). Surgery for PTA is associated with rapid recovery of CNDs in the early, subacute, and delayed time frames, and with rapid headache improvement in the early and subacute time frames in 50% or more of patients.
Keywords: headache; ophthalmoplegia; pituitary apoplexy; pituitary tumor apoplexy; recovery.
Conflict of interest statement
A.H.K. is a consultant for Monteris Medical and has received research grants from Monteris Medical, Stryker, and Collagen Matrix, the latter two regarding clinical outcomes studies for a dural substitute, which has no direct relation to this study. J.M. is a primary investigator for clinical studies with Chiasma, Corcept, and StrongBridge, none of which have direct relation to this study. C.K.-C. is a consultant for Medtronic and Intersect ENT, which have no direct relation to this study. M.C. received funding from (1) IMRIS Inc. for an unrestricted educational grant to support an iMRI database and brain tumor outcomes analysis project, the IMRIS Multicenter intraoperative MRI Neurosurgery Database (I-MiND), (2) The Head for the Cure Foundation, and (3) Mrs. Carol Rossfeld and The Alex & Alice Aboussie Family Charitable Foundation. I-MiND is Supported by Clinical and Translational Science Award (CTSA) Grant [UL1 TR000448] and The Siteman Comprehensive Cancer Center and NCI Cancer Center Support Grant P30 CA091842. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures


Similar articles
-
Pituitary tumor apoplexy.J Clin Neurosci. 2015 Jun;22(6):939-44. doi: 10.1016/j.jocn.2014.11.023. Epub 2015 Mar 20. J Clin Neurosci. 2015. PMID: 25800143 Review.
-
Management and outcomes of pituitary apoplexy.J Neurosurg. 2015 Jun;122(6):1450-7. doi: 10.3171/2014.10.JNS141204. Epub 2015 Apr 10. J Neurosurg. 2015. PMID: 25859804
-
Endoscopic Endonasal Surgery for Pituitary Apoplexy: Evidence On a 75-Case Series From a Tertiary Care Center.World Neurosurg. 2017 Oct;106:331-338. doi: 10.1016/j.wneu.2017.06.117. Epub 2017 Jun 30. World Neurosurg. 2017. PMID: 28669873
-
Time Course of Symptomatic Recovery After Endoscopic Transsphenoidal Surgery for Pituitary Adenoma Apoplexy in the Modern Era.World Neurosurg. 2016 Dec;96:434-439. doi: 10.1016/j.wneu.2016.09.052. Epub 2016 Sep 20. World Neurosurg. 2016. PMID: 27663263
-
Pituitary Apoplexy.Neurosurg Clin N Am. 2019 Oct;30(4):457-463. doi: 10.1016/j.nec.2019.06.001. Epub 2019 Aug 7. Neurosurg Clin N Am. 2019. PMID: 31471052 Review.
Cited by
-
Pituitary apoplexy: surgical or conservative? A meta-analytical insight.Front Surg. 2025 Jun 4;12:1579498. doi: 10.3389/fsurg.2025.1579498. eCollection 2025. Front Surg. 2025. PMID: 40535550 Free PMC article.
-
Pituitary Apoplexy in Patients with Pituitary Neuroendocrine Tumors (PitNET).Biomedicines. 2023 Feb 23;11(3):680. doi: 10.3390/biomedicines11030680. Biomedicines. 2023. PMID: 36979658 Free PMC article. Review.
References
-
- Arafah B.M., Prunty D., Ybarra J., Hlavin M.L., Selman W.R. The dominant role of increased intrasellar pressure in the pathogenesis of hypopituitarism, hyperprolactinemia, and headaches in patients with pituitary adenomas. J. Clin. Endocrinol. Metab. 2000;85:1789–1793. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

