Ultralong Follow-Up of Spinal Fusion for Adolescent Idiopathic Scoliosis: Harrington Instrumentation vs Uninstrumented Fusion
- PMID: 35878905
- PMCID: PMC9807042
- DOI: 10.14444/8328
Ultralong Follow-Up of Spinal Fusion for Adolescent Idiopathic Scoliosis: Harrington Instrumentation vs Uninstrumented Fusion
Abstract
Background: Harrington instrumentation for adolescent idiopathic scoliosis (AIS) was revolutionary and allowed patients to mobilize faster as compared with patients treated with uninstrumented fusion. However, Harrington instrumentation provided correction of the deformity in 1 plane, resulting in limited sagittal plane control. Patients who received these 2 surgeries are aging, and to date, ultralong follow-up of these patients has not been reported.
Objective: The purpose of this study was to evaluate long-term patient-reported outcomes and radiographic parameters after Harrington nonsegmental distraction instrumentation vs uninstrumented fusion in the treatment of AIS.
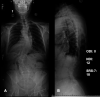
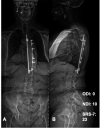
Methods: Fourteen adult patients with AIS who were previously instrumented (n = 7) or uninstrumented (n = 7) were identified. Recent x-ray image measurements such as pelvic incidence (PI), sagittal vertical axis (SVA), pelvic tilt (PT), lumbar lordosis (LL), and pelvic incidence minus lumbar lordosis (PI-LL) were used to analyze deformities. Scoliosis Research Society-7 (SRS-7), Neck Disability Index (NDI), and Oswestry Disability Index (ODI) were used to evaluate patient-reported outcomes. Complications and rates of revision surgery were also evaluated.
Results: The mean age was 67.1 ± 5 years in the instrumented group and 64.1 ± 9 years in the uninstrumented group. There were no significant differences between instrumented and uninstrumented in SRS-7 (23.4 ± 2.9 vs 23.6 ± 2.6, P = 0.93), NDI (5.7 ± 4.5 vs 10.6 ± 4.5, P = 0.08), and ODI (9.7 ± 13.7 vs 9.4 ± 8.7, P = 0.99). Radiographic measurements of instrumented vs uninstrumented resulted in comparable PT (24.0 ± 7.9 vs 30.5 ± 4.7, P = 0.09), PI (61.3 ± 16.9 vs 67.2 ± 9.5, P = 0.47), LL (34.9 ± 14.4 vs 42.8 ± 11.0, P = 0.29), PI-LL (26.4 ± 25.1 vs 24.3 ± 10.4, P = 0.43), and SVA (38.1 ± 30.1 vs 52.3 ± 21.6, P = 0.37). There were 2 patients in the instrumented group who developed adjacent segment disease that required operative intervention compared with none in the uninstrumented group (P = 0.46).
Conclusion: In long-term follow-up of instrumented and uninstrumented fusion, patients had similar patient-reported outcomes and radiographic parameters, although the instrumented cohort had higher rates of adjacent segment disease.
Keywords: Harrington; deformity; nonsegmental distraction rod instrumentation; scoliosis surgery; spinal fusion; surgical outcome.
This manuscript is generously published free of charge by ISASS, the International Society for the Advancement of Spine Surgery. Copyright © 2022 ISASS. To see more or order reprints or permissions, see http://ijssurgery.com.
Conflict of interest statement
Declaration of Conflicting Interests: Paul Rubery declares a grant from AO Spine. James Sanders declares grants from SRS and POSNA and consulting fees from Orthopaediatric. Emmanuel Menga declares a grant from Globus Medical, royalties from Evolution Spine, and consulting fees from Globus Medical. Addisu Mesfin declares grants from Globus Medical and AO Spine and consulting fees from Medtronic and DePuy Synthes. The remaining authors have no disclosures.
Figures
Similar articles
-
Utility of multilevel lateral interbody fusion of the thoracolumbar coronal curve apex in adult deformity surgery in combination with open posterior instrumentation and L5-S1 interbody fusion: a case-matched evaluation of 32 patients.J Neurosurg Spine. 2017 Feb;26(2):208-219. doi: 10.3171/2016.8.SPINE151543. Epub 2016 Oct 21. J Neurosurg Spine. 2017. PMID: 27767682
-
Comparative analysis of 3 surgical strategies for adult spinal deformity with mild to moderate sagittal imbalance.J Neurosurg Spine. 2018 Jan;28(1):40-49. doi: 10.3171/2017.5.SPINE161370. Epub 2017 Nov 3. J Neurosurg Spine. 2018. PMID: 29087808
-
Mismatch Between Pelvic Incidence and Lumbar Lordosis is the Key Sagittal Plane Determinant of Patient Outcome at Minimum 40 Years After Instrumented Fusion for Adolescent Idiopathic Scoliosis.Spine (Phila Pa 1976). 2022 Mar 1;47(5):E169-E176. doi: 10.1097/BRS.0000000000004277. Spine (Phila Pa 1976). 2022. PMID: 34798644
-
The Legacy of Harrington's Rod and the Evolution of Long-Segment Constructs in Spine Surgery.J Clin Med. 2024 Sep 19;13(18):5556. doi: 10.3390/jcm13185556. J Clin Med. 2024. PMID: 39337041 Free PMC article. Review.
-
Transforming Spinal Surgery: The Life and Innovations of Dr. Paul Harrington.Cureus. 2024 Oct 17;16(10):e71681. doi: 10.7759/cureus.71681. eCollection 2024 Oct. Cureus. 2024. PMID: 39552966 Free PMC article. Review.
Cited by
-
Comparison of 3-Dimensional Correction and Clinical Outcomes of Lenke 1A Curves with the Stable Vertebra (SV) or SV-1 Selected as the Lowest Instrumented Vertebra.Clin Orthop Surg. 2025 Apr;17(2):250-257. doi: 10.4055/cios23228. Epub 2025 Feb 25. Clin Orthop Surg. 2025. PMID: 40170777 Free PMC article.
-
Long-term follow-up of adolescent idiopathic scoliosis surgery with Harrington instrumentations: a systematic review and meta-analysis.Musculoskelet Surg. 2025 Mar;109(1):17-31. doi: 10.1007/s12306-024-00836-y. Epub 2024 May 28. Musculoskelet Surg. 2025. PMID: 38806854
References
-
- Parent S, Newton PO, Wenger DR. Adolescent idiopathic scoliosis: etiology, anatomy, natural history, and bracing. Instr Course Lect. 2005;54:529–536. - PubMed
-
- Goldstein LA. Results in the treatment of scoliosis with turnbuckle plaster cast correction and fusion. J Bone Joint Surg Am. 1959;41-A(2):321–335. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
