Surgical treatment of patients with infective endocarditis: changes in temporal use, patient characteristics, and mortality-a nationwide study
- PMID: 35906539
- PMCID: PMC9336053
- DOI: 10.1186/s12872-022-02761-z
Surgical treatment of patients with infective endocarditis: changes in temporal use, patient characteristics, and mortality-a nationwide study
Abstract
Background: Valve surgery guidelines for infective endocarditis (IE) are unchanged over decades and nationwide data about the use of valve surgery do not exist.
Methods: We included patients with first-time IE (1999-2018) using Danish nationwide registries. Proportions of valve surgery were reported for calendar periods (1999-2003, 2004-2008, 2009-2013, 2014-2018). Comparing calendar periods in multivariable analyses, we computed likelihoods of valve surgery with logistic regression and rates of 30 day postoperative mortality with Cox regression.
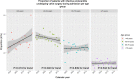
Results: We included 8804 patients with first-time IE; 1981 (22.5%) underwent surgery during admission, decreasing by calendar periods (N = 360 [24.4%], N = 483 [24.0%], N = 553 [23.5%], N = 585 [19.7%], P = < 0.001 for trend). For patients undergoing valve surgery, median age increased from 59.7 to 66.9 years (P ≤ 0.001) and the proportion of males increased from 67.8% to 72.6% (P = 0.008) from 1999-2003 to 2014-2018. Compared with 1999-2003, associated likelihoods of valve surgery were: Odds ratio (OR) = 1.14 (95% CI: 0.96-1.35), OR = 1.20 (95% CI: 1.02-1.42), and OR = 1.10 (95% CI: 0.93-1.29) in 2004-2008, 2009-2013, and 2014-2018, respectively. 30 day postoperative mortalities were: 12.7%, 12.8%, 6.9%, and 9.7% by calendar periods. Compared with 1999-2003, associated mortality rates were: Hazard ratio (HR) = 0.96 (95% CI: 0.65-1.41), HR = 0.43 (95% CI: 0.28-0.67), and HR = 0.55 (95% CI 0.37-0.83) in 2004-2008, 2009-2013, and 2014-2018, respectively.
Conclusions: On a nationwide scale, 22.5% of patients with IE underwent valve surgery. Patient characteristics changed considerably and use of valve surgery decreased over time. The adjusted likelihood of valve surgery was similar between calendar periods with a trend towards an increase while rates of 30 day postoperative mortality decreased.
Keywords: Cardiac valve surgery; Epidemiology; Infective endocarditis; Temporal trend.
© 2022. The Author(s).
Conflict of interest statement
Henning Bundgaard: Speakers honorarium from Amgen unrelated to this manuscript. Claus Moser: Independent research grant from the Novo Nordisk Foundation, unrelated to this manuscript. Ivy Susanne Modrau: Independent research grants from the Health Research Foundation of Central Denmark Region, unrelated to this manuscript. Niels Eske Bruun: Independent research grants from the Novo Nordisk Foundation, and from the regions of Southern Denmark and Zealand, unrelated to this manuscript. Christian Torp-Pedersen: Grants from Novo Nordisk and Bayer,unrelated to this manuscript. Andrew Wang: Legal expert for case of infective endocarditis (defendant), unrelated to this manuscript. Lars Køber: Speakers honorarium from Novo, Novartis, AstraZeneca and Boehringer, unrelated to this manuscript. Emil Loldrup Fosbøl: Independent research grants from the Novo Nordisk Foundation and the Danish Heart Association. The remaining authors declare that they have no competing interests.
Figures


References
-
- Habib G, Lancellotti P, Antunes MJ, Bongiorni MG, Casalta JP, Del Zotti F, et al. ESC Guidelines for the management of infective endocarditis: the task force for the management of infective endocarditis of the European society of cardiology (ESC) endorsed by: European association for cardio-thoracic surgery (EACTS), the European association of nuclear medicine (EANM) Eur Heart J. 2015;36(44):3075–3128. doi: 10.1093/eurheartj/ehv319. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

