Sandwich Technique for Large Osteochondral Lesions of the Knee
- PMID: 35906752
- PMCID: PMC9340910
- DOI: 10.1177/19476035221102571
Sandwich Technique for Large Osteochondral Lesions of the Knee
Abstract
Objective: To evaluate whether a sandwich technique procedure for large osteochondral lesions (OCL) of the medial femur condyle reduces clinical symptoms and improves activity level as well as to assess repair tissue integration on MRI over 2 years.
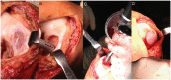
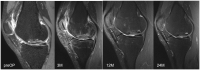
Design: Twenty-one patients (median age: 29 years, 18-44 years) who received matrix-associated autologous chondrocyte transplantation (MACT) combined with cancellous bone grafting at the medial femur condyle in a 1-step procedure were prospectively included. Patients were evaluated before surgery (baseline) as well as 3, 6, 12, and 24 months postoperatively, including clinical evaluation, Lysholm score, Tegner Activity Rating Scale, and MRI with Magnetic Resonance Observation of Cartilage Repair Tissue (MOCART) score and a modified Whole-Organ Magnetic Resonance Imaging Score (WORMS).
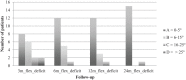
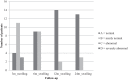
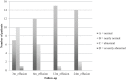
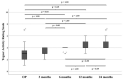
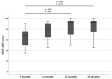
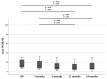
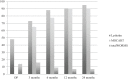
Results: Seventeen patients were available for the 24-month (final) follow-up (4 dropouts). Lysholm significantly improved from 48 preoperatively stepwise to 95 at final follow-up (P < 0.05). Tegner improvement from 2.5 at baseline to 4.0 at final follow-up was not significant (P = 1.0). MOCART score improved significantly and stepwise from 65 at 3 months to 90 at 24 months (P < 0.05). Total WORMS improved from 14.5 at surgery to 7.0 after 24 months (P < 0.05). Body mass index and defect size at surgery correlated with total WORMS at final follow-up (P < 0.05) but did not correlate with clinical scores or defect filling.
Conclusion: MACT combined with cancellous bone grafting at the medial femoral condyle reduces symptoms continuously over 2 years. A 1-step procedure may reduce perioperative morbidity. However, despite improvements, patients' activity levels remain low, even 2 years after surgery.
Keywords: MACT; autologous chondrocyte; bone grafting; cartilage transplantation; grafts; joint involved; knee.
Conflict of interest statement
Figures



References
-
- Zellner J, Grechenig S, Pfeifer CG, Krutsch W, Koch M, Welsch G, et al. Clinical and radiological regeneration of large and deep osteochondral defects of the knee by bone augmentation combined with matrix-guided autologous chondrocyte transplantation. Am J Sports Med. 2017;45(13):3069-80. doi: 10.1177/0363546517717679. - DOI - PubMed
-
- Clanton TO, DeLee JC. Osteochondritis dissecans. History, pathophysiology and current treatment concepts. Clin Orthop Relat Res. 1982;167:50-64. Available from: https://www.ncbi.nlm.nih.gov/pubmed/6807595. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

