Weight loss outcomes achieved by adults accessing an online programme offered as part of Public Health England's 'Better Health' campaign
- PMID: 35907834
- PMCID: PMC9339188
- DOI: 10.1186/s12889-022-13847-w
Weight loss outcomes achieved by adults accessing an online programme offered as part of Public Health England's 'Better Health' campaign
Abstract
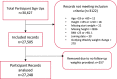
Effective use of health technology may offer a scalable solution to the obesity pandemic. Online digital programmes provide a convenient and flexible way for more people to access regular support. This service evaluation aims to determine whether adults accessing an online weight management programme via a national campaign are successful in losing weight.Data was analysed for adults registering with Slimming World's online programme using a discounted membership offered as part of PHE's 'Better Health' campaign between July and December 2020. Last-weight carried forward was used to calculate weight outcomes for participants who had the opportunity to complete 12-weeks and recorded ≥ one weight besides baseline. Engagement was determined using number of online weekly weights recorded with high engagers having weight data for ≥ 9 occasions. Socioeconomic status was assessed using postcode data. Resubscription and uploaded weight data were used to determine numbers who continued beyond the offer period.Twenty-seven thousand two hundred forty-eight adults (5.3% males) with mean age 41.0 ± 11.4 years met inclusion criteria. Mean baseline BMI was 33.4 ± 6.8 kg/m2 (29.2% 30-34.9, 18.3% 35-39.9 and 15.1% > 40 kg/m2). Mean weight loss at 12 weeks was 2.7 (± 3) kg representing a mean loss of 3% (± 3.1) body weight with 42.3% achieving ≥ 3% and 22.1% weight loss ≥ 5%. Median number of weigh-ins was six. Men had greater weight losses compared to women (p < 0.001). High engagers, both men and women, achieved greater weight losses (p < 0.001). Absolute weight loss was associated with joining BMI (rs = -0.15, p < 0.001) but for % weight change only small differences were seen (max effect size = 0.03) with no differences in weight change for high engagers between different baseline BMI categories (p > 0.05). 30.9% were in the lowest two IMD quintiles and absolute and percentage weight change did not differ across deprivation quintiles (p > 0.05). 34.9% continued to access the online support after the offer period.This service evaluation shows that an online programme, offered as part of a national campaign, can offer effective support to a large number of people with different starting BMIs and from different socioeconomic backgrounds. An increased level of engagement leads to better weight losses.
Keywords: Weight management; adults; online digital programme; service evaluation.
© 2022. The Author(s).
Conflict of interest statement
All authors, including AA, receive salaries (full or part) from Slimming World.
Figures
References
-
- National Institute for Health and Clinical Excellence NICE, 2014. Weight management: lifestyle services for overweight or obese adults. https://www.nice.org.uk/guidance/ph53. Accessed 21.02.22.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous