Association Between Pulse Pressure With All-Cause and Cardiac Mortality in Acute Coronary Syndrome: An Observational Cohort Study
- PMID: 35911514
- PMCID: PMC9325995
- DOI: 10.3389/fcvm.2022.930755
Association Between Pulse Pressure With All-Cause and Cardiac Mortality in Acute Coronary Syndrome: An Observational Cohort Study
Abstract
Background: Pulse pressure (PP) is a surrogate of aortic stiffness, and reflects cardiac performance and stroke volume. Previous studies have indicated that PP was a robust predictor of cardiovascular outcomes and mortality. However, results have been mixed, and very few studies have focused on the association of PP with mortality in acute coronary syndrome (ACS). Thus, we aimed to investigate the relationship between admission PP and the prognosis of patients with ACS.
Methods: This cohort study included 10,824 patients diagnosed with ACS from the Cardiovascular Center Beijing Friendship Hospital Database Bank (CBDBANK) from January 2013 to October 2018. Patients with cardiogenic shock, malignancy, severe trauma and, no PP at admission were excluded. Restricted cubic spline and Cox proportional hazards regression were used to evaluate the association between PP and 1-year all-cause and cardiac mortality.
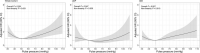
Results: In the whole cohort, a total of 237 (2.19%) all-cause deaths were reported at 1-year follow-up. Restricted cubic spline analysis suggested a J-shaped relationship between PP and mortality. Among patients with ACS, both lower and higher PP levels were related to an increased risk of mortality (P non-linear < 0.001); with a PP level of 30 or 80 mmHg, as compared with 50 mmHg, the adjusted hazard ratios for 1-year all-cause mortality were 2.02 (95% CI, 1.27-3.22) and 1.62 (95% CI, 1.13-2.33), respectively, after adjustments for potential confounders. Similar results were observed for cardiac deaths. The J-shaped relationship between PP and mortality remained in a series of subgroup analyses.
Conclusion: Our results suggested that both low and high PP were associated with an increased risk of mortality in patients with ACS.
Keywords: acute coronary syndrome; all-cause mortality; cardiac mortality; cohort study; pulse pressure.
Copyright © 2022 Wang, Su, Jiang, Li, Chen and Li.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures




Similar articles
-
Association Between Admission Pulse Pressure and Long-Term Mortality in Elderly Patients With Type 2 Diabetes Mellitus Admitted for Acute Coronary Syndrome: An Observational Cohort Study.Front Cardiovasc Med. 2022 May 11;9:855602. doi: 10.3389/fcvm.2022.855602. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 35647076 Free PMC article.
-
Prognostic value of pulse pressure after an acute coronary syndrome.Atherosclerosis. 2018 Oct;277:219-226. doi: 10.1016/j.atherosclerosis.2018.07.013. Epub 2018 Jul 20. Atherosclerosis. 2018. PMID: 30033338
-
Prognostic power of lower pulse pressure on long-term all-cause mortality in octogenarians with acute coronary syndrome: a propensity-score-matched cohort study.J Hypertens. 2015 Feb;33(2):279-86. doi: 10.1097/HJH.0000000000000403. J Hypertens. 2015. PMID: 25318655
-
The U-shape relationship between pulse pressure level on inpatient admission and long-term mortality in acute coronary syndrome patients undergoing percutaneous coronary intervention.J Clin Hypertens (Greenwich). 2022 Jan;24(1):58-66. doi: 10.1111/jch.14408. Epub 2021 Dec 9. J Clin Hypertens (Greenwich). 2022. PMID: 34882954 Free PMC article.
-
Contrast-induced acute kidney injury and adverse clinical outcomes risk in acute coronary syndrome patients undergoing percutaneous coronary intervention: a meta-analysis.BMC Nephrol. 2018 Dec 22;19(1):374. doi: 10.1186/s12882-018-1161-5. BMC Nephrol. 2018. PMID: 30577763 Free PMC article.
Cited by
-
Pulse pressure and inferior wall ST-segment elevation myocardial infarction: investigating mortality, hospital major cardiovascular events, and long-term prognosis.J Public Health Afr. 2023 Dec 1;14(12):2743. doi: 10.4081/jphia.2023.2743. eCollection 2023 Dec 27. J Public Health Afr. 2023. PMID: 38204807 Free PMC article.
-
The contribution of cumulative blood pressure load to dementia, cognitive function and mortality in older adults.J Hypertens. 2024 Nov 1;42(11):1922-1931. doi: 10.1097/HJH.0000000000003808. Epub 2024 Jul 11. J Hypertens. 2024. PMID: 38989713 Free PMC article.
References
-
- Dzau VJ. Atherosclerosis and hypertension: mechanisms and Interrelationships. J Cardiovasc Pharmacol. (1990) 15(Suppl. 5):S59–64. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

