Regulation of cholesterol homeostasis in health and diseases: from mechanisms to targeted therapeutics
- PMID: 35918332
- PMCID: PMC9344793
- DOI: 10.1038/s41392-022-01125-5
Regulation of cholesterol homeostasis in health and diseases: from mechanisms to targeted therapeutics
Abstract
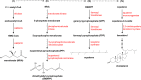
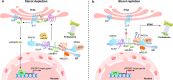
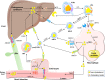
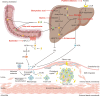
Disturbed cholesterol homeostasis plays critical roles in the development of multiple diseases, such as cardiovascular diseases (CVD), neurodegenerative diseases and cancers, particularly the CVD in which the accumulation of lipids (mainly the cholesteryl esters) within macrophage/foam cells underneath the endothelial layer drives the formation of atherosclerotic lesions eventually. More and more studies have shown that lowering cholesterol level, especially low-density lipoprotein cholesterol level, protects cardiovascular system and prevents cardiovascular events effectively. Maintaining cholesterol homeostasis is determined by cholesterol biosynthesis, uptake, efflux, transport, storage, utilization, and/or excretion. All the processes should be precisely controlled by the multiple regulatory pathways. Based on the regulation of cholesterol homeostasis, many interventions have been developed to lower cholesterol by inhibiting cholesterol biosynthesis and uptake or enhancing cholesterol utilization and excretion. Herein, we summarize the historical review and research events, the current understandings of the molecular pathways playing key roles in regulating cholesterol homeostasis, and the cholesterol-lowering interventions in clinics or in preclinical studies as well as new cholesterol-lowering targets and their clinical advances. More importantly, we review and discuss the benefits of those interventions for the treatment of multiple diseases including atherosclerotic cardiovascular diseases, obesity, diabetes, nonalcoholic fatty liver disease, cancer, neurodegenerative diseases, osteoporosis and virus infection.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
References
-
- Schoenheimer R, Breusch F. Synthesis and destruction of cholesterol in the organism. J. Biol. Chem. 1933;103:439–448. doi: 10.1016/S0021-9258(18)75823-7. - DOI
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

