Experiences of performing ABO-incompatible kidney transplantation in Bangladesh
- PMID: 35919197
- PMCID: PMC9296974
- DOI: 10.4285/kjt.22.0014
Experiences of performing ABO-incompatible kidney transplantation in Bangladesh
Abstract
Background: The number of end-stage renal disease (ESRD) patients is increasing in Bangladesh. Currently, living kidney donation is the only viable option for transplantation in Bangladesh, and it is further restricted by ABO compatibility issues. We have performed ABO-incompatible kidney transplantations (ABOi KTs) in Bangladesh since 2018. This study examines our experiences with seven cases of ABOi KT.
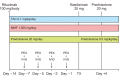
Methods: The desensitization protocol included low-dose rituximab (100 mg/body) followed by plasma exchange (PEX), which was followed by a 5-g dose of intravenous immunoglobulin. Immunosuppression was undertaken using tacrolimus (0.1 mg/kg/day), mycophenolate mofetil (1,500 mg/day), and prednisolone (0.5 mg/kg/day). All patients received basiliximab for induction therapy.
Results: The median baseline anti-ABO antibody titer was 164 (range, 132-1128). Transplantation was performed at a titer of ≤18. Our patients attended three to five PEX sessions before transplantation. Graft survival was 100% in the seven cases over a mean period of 22 months. The mean creatinine level was 204.6±47.4 µmol/L. Two patients were suspected of having developed acute rejection and received intravenous methylprednisolone, resulting in improved kidney function. One patient required posttransplant hemodialysis due to delayed graft function and subsequently improved. Infection was the most common complication experienced by ABOi KT patients. Two patients developed severe cytomegalovirus pneumonia and died with functioning grafts.
Conclusions: ABOi KT in Bangladesh will substantially expand the living kidney donor pool and bring hope to a large number of ESRD patients without ABO-compatible donors. However, the high cost and risk of acute rejection and infection remain major concerns.
Keywords: Bangladesh; Blood group incompatibility; Chronic kidney failure; Kidney transplantation; Plasma exchange.
Copyright © 2022 The Korean Society for Transplantation.
Figures
Similar articles
-
ABO-incompatible transplantation without conventional induction immunosuppression (IL-2RB or depleting agents).Saudi J Kidney Dis Transpl. 2020 May-Jun;31(3):572-581. doi: 10.4103/1319-2442.289443. Saudi J Kidney Dis Transpl. 2020. PMID: 32655043
-
Long-term results of ABO-incompatible living kidney transplantation: a single-center experience.Transplantation. 1998 Jan 27;65(2):224-8. doi: 10.1097/00007890-199801270-00014. Transplantation. 1998. PMID: 9458019
-
ABO-Incompatible Kidney Transplantation: Low Rates of Infectious Complications and Excellent Patient Survival.Transplant Proc. 2019 Mar;51(2):512-516. doi: 10.1016/j.transproceed.2019.01.002. Epub 2019 Jan 4. Transplant Proc. 2019. PMID: 30879579
-
Isoagglutinin adsorption in ABO-incompatible transplantation.Transfus Apher Sci. 2010 Oct;43(2):231-5. doi: 10.1016/j.transci.2010.07.016. Epub 2010 Jul 27. Transfus Apher Sci. 2010. PMID: 20667787 Review.
-
ABO incompatible renal transplants: Good or bad?World J Transplant. 2014 Mar 24;4(1):18-29. doi: 10.5500/wjt.v4.i1.18. World J Transplant. 2014. PMID: 24669364 Free PMC article. Review.
Cited by
-
Outcomes of ABO-incompatible kidney transplants with very high isoagglutinin titers: a single-center experience and literature review.Front Immunol. 2024 Dec 2;15:1504495. doi: 10.3389/fimmu.2024.1504495. eCollection 2024. Front Immunol. 2024. PMID: 39687613 Free PMC article.
References
-
- Rashid HU, Alam MR, Khanam A, Rahman MM, Ahmed S, Mostafi M, et al. Nephrology in Bangladesh. In: Moura-Neto JA, Divino-Filho JC, Ronco C, editors. Nephrology Worldwide. Springer; Cham: 2021. pp. 221–38. - DOI
-
- Nepali R, Shah DS. Experience of starting ABO incompatible renal transplant in Nepal. Transpl Rep. 2019;4:100026. doi: 10.1016/j.tpr.2019.100026. - DOI
LinkOut - more resources
Full Text Sources