Randomized controlled trial of once-per-week intermittent fasting for health improvement: the WONDERFUL trial
- PMID: 35919268
- PMCID: PMC9241570
- DOI: 10.1093/ehjopen/oeab026
Randomized controlled trial of once-per-week intermittent fasting for health improvement: the WONDERFUL trial
Abstract
Aims: Low-density lipoprotein cholesterol (LDL-C) predicts heart disease onset and may be reduced by intermittent fasting. Some studies, though, reported that fasting increased LDL-C; however, no study evaluated LDL-C as the primary endpoint. This randomized controlled trial evaluated the effect of low-frequency intermittent fasting on LDL-C and other biomarkers.
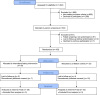
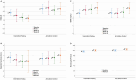
Methods and results: Adults aged 21-70 years were enrolled who were not taking a statin, had modestly elevated LDL-C, had ≥1 metabolic syndrome feature or type 2 diabetes, and were not taking anti-diabetic medication (N = 103). Water-only 24-h fasting was performed twice weekly for 4 weeks and then once weekly for 22 weeks; controls ate ad libitum. The primary outcome was 26-week LDL-C change score. Secondary outcomes (requiring P ≤ 0.01) were 26-week changes in homeostatic model assessment of insulin resistance (HOMA-IR), Metabolic Syndrome Score (MSS), brain-derived neurotrophic factor (BDNF), and MicroCog general cognitive proficiency index (GCPi). Intermittent fasting (n = 50) and control (n = 53) subjects were, respectively, aged 49.3 ± 12.0 and 47.0 ± 9.8 years, predominantly female (66.0% and 67.9%), and overweight (103 ± 24 and 100 ± 21 kg) and had modest LDL-C elevation (124 ± 19 and 128 ± 20 mg/dL). Drop-outs (n = 12 fasting, n = 20 control) provided an evaluable sample of n = 71 (n = 38 fasting, n = 33 control). Intermittent fasting did not change LDL-C (0.2 ± 16.7 mg/dL) vs. control (2.5 ± 19.4 mg/dL; P = 0.59), but it improved HOMA-IR (-0.75 ± 0.79 vs. -0.10 ± 1.06; P = 0.004) and MSS (-0.34 ± 4.72 vs. 0.31 ± 1.98, P = 0.006). BDNF (P = 0.58), GCPi (P = 0.17), and weight (-1.7 ± 4.7 kg vs. 0.2 ± 3.5 kg, P = 0.06) were unchanged.
Conclusions: A low-frequency intermittent fasting regimen did not reduce LDL-C or improve cognitive function but significantly reduced both HOMA-IR and MSS.
Trial registration: clinicaltrials.gov, NCT02770313.
Keywords: Cholesterol; Cognitive function; Insulin resistance; Metabolic syndrome; Pre-diabetes; Therapeutic fasting.
© The Author(s) 2021. Published by Oxford University Press on behalf of the European Society of Cardiology.
Figures



References
-
- Folin O, Denis W. On starvation and obesity with special regerence to acidosis. J Biol Chem 1915;21:183–192.
-
- Carlson AJ, Hoelzel F. Apparent prolongation of the life span of rats by intermittent fasting. J Nutr 1946;31:363–375. - PubMed
-
- Heilbronn LK, Smith SR, Martin CK, Anton SD, Ravussin E. Alternate-day fasting in nonobese subjects: effects on body weight, body composition, and energy metabolism. Am J Clin Nutr 2005;81:69–73. - PubMed
-
- Johnson JB, Summer W, Cutler RG, Martin B, Hyun D-H, Dixit VD, Pearson M, Nassar M, Telljohann R, Tellejohan R, Maudsley S, Carlson O, John S, Laub DR, Mattson MP. Alternate day calorie restriction improves clinical findings and reduces markers of oxidative stress and inflammation in overweight adults with moderate asthma. Free Radic Biol Med 2007;42:665–674. - PMC - PubMed
-
- Trepanowski JF, Kroeger CM, Barnosky A, Klempel MC, Bhutani S, Hoddy KK, Gabel K, Freels S, Rigdon J, Rood J, Ravussin E, Varady KA. Effect of alternate-day fasting on weight loss, weight maintenance, and cardioprotection among metabolically healthy obese adults: a randomized clinical trial. JAMA Intern Med 2017;177:930–938. - PMC - PubMed
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

