Machine learning-based prediction of emergency neurosurgery within 24 h after moderate to severe traumatic brain injury
- PMID: 35922831
- PMCID: PMC9351267
- DOI: 10.1186/s13017-022-00449-5
Machine learning-based prediction of emergency neurosurgery within 24 h after moderate to severe traumatic brain injury
Abstract
Background: Rapid referral of traumatic brain injury (TBI) patients requiring emergency neurosurgery to a specialized trauma center can significantly reduce morbidity and mortality. Currently, no model has been reported to predict the need for acute neurosurgery in severe to moderate TBI patients. This study aims to evaluate the performance of Machine Learning-based models to establish to predict the need for neurosurgery procedure within 24 h after moderate to severe TBI.
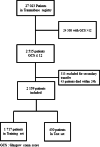
Methods: Retrospective multicenter cohort study using data from a national trauma registry (Traumabase®) from November 2011 to December 2020. Inclusion criteria correspond to patients over 18 years old with moderate or severe TBI (Glasgow coma score ≤ 12) during prehospital assessment. Patients who died within the first 24 h after hospital admission and secondary transfers were excluded. The population was divided into a train set (80% of patients) and a test set (20% of patients). Several approaches were used to define the best prognostic model (linear nearest neighbor or ensemble model). The Shapley Value was used to identify the most relevant pre-hospital variables for prediction.
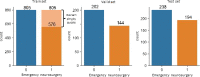
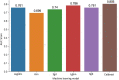
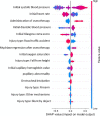
Results: 2159 patients were included in the study. 914 patients (42%) required neurosurgical intervention within 24 h. The population was predominantly male (77%), young (median age 35 years [IQR 24-52]) with severe head injury (median GCS 6 [3-9]). Based on the evaluation of the predictive model on the test set, the logistic regression model had an AUC of 0.76. The best predictive model was obtained with the CatBoost technique (AUC 0.81). According to the Shapley values method, the most predictive variables in the CatBoost were a low initial Glasgow coma score, the regression of pupillary abnormality after osmotherapy, a high blood pressure and a low heart rate.
Conclusion: Machine learning-based models could predict the need for emergency neurosurgery within 24 h after moderate and severe head injury. Potential clinical benefits of such models as a decision-making tool deserve further assessment. The performance in real-life setting and the impact on clinical decision-making of the model requires workflow integration and prospective assessment.
Keywords: Artificial intelligence; Emergency neurosurgery; Prediction models; Trauma; Traumatic brain injury.
© 2022. The Author(s).
Conflict of interest statement
TG declares consulting fees from Laboratoire du Biomédicament in the past.
Figures

References
-
- Roquilly A, Moyer JD, Huet O, Lasocki S, Cohen B, Dahyot-Fizelier C, et al. Effect of continuous infusion of hypertonic saline vs standard care on 6-month neurological outcomes in patients with traumatic brain injury: the COBI randomized clinical trial. JAMA. 2021;325:2056–2066. doi: 10.1001/jama.2021.5561. - DOI - PMC - PubMed
-
- Cooper DJ, Nichol AD, Bailey M, Bernard S, Cameron PA, Pili-Floury S, et al. Effect of early sustained prophylactic hypothermia on neurologic outcomes among patients with severe traumatic brain injury: the POLAR randomized clinical trial. JAMA. 2018;320:2211–2220. doi: 10.1001/jama.2018.17075. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

