EEG Evaluation of Stress Exposure on Healthcare Workers During COVID-19 Emergency: Not Just an Impression
- PMID: 35923294
- PMCID: PMC9339626
- DOI: 10.3389/fnsys.2022.923576
EEG Evaluation of Stress Exposure on Healthcare Workers During COVID-19 Emergency: Not Just an Impression
Abstract
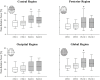
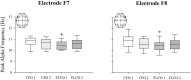
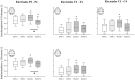
Psychological distress among healthcare professionals, although already a common condition, was exacerbated by the COVID-19 pandemic. This effect has been generally self-reported or assessed through questionnaires. We aimed to identify potential abnormalities in the electrical activity of the brain of healthcare workers, operating in different roles during the pandemic. Cortical activity, cognitive performances, sleep, and burnout were evaluated two times in 20 COVID-19 frontline operators (FLCO, median age 29.5 years) and 20 operators who worked in COVID-19-free units (CFO, median 32 years): immediately after the outbreak of the pandemic (first session) and almost 6 months later (second session). FLCO showed higher theta relative power over the entire scalp (FLCO = 19.4%; CFO = 13.9%; p = 0.04) and lower peak alpha frequency of electrodes F7 (FLCO = 10.4 Hz; CFO = 10.87 Hz; p = 0.017) and F8 (FLCO = 10.47 Hz; CFO = 10.87 Hz; p = 0.017) in the first session. FLCO parietal interhemispheric coherence of theta (FLCO I = 0.607; FLCO II = 0.478; p = 0.025) and alpha (FLCO I = 0.578; FLCO II = 0.478; p = 0.007) rhythms decreased over time. FLCO also showed lower scores in the global cognitive assessment test (FLCO = 22.72 points; CFO = 25.56; p = 0.006) during the first session. The quantitative evaluation of the cortical activity might therefore reveal early signs of changes secondary to stress exposure in healthcare professionals, suggesting the implementation of measures to prevent serious social and professional consequences.
Keywords: COVID-19; EEG; healthcare workers; mental fatigue; stress exposure.
Copyright © 2022 LoMauro, Molisso, Mameli, Ruggiero, Ferrucci, Dellarosa, Aglieco, Aliverti, Barbieri and Vergari.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

Similar articles
-
Trends in burnout and psychological distress in hospital staff over 12 months of the COVID-19 pandemic: a prospective longitudinal survey.J Occup Med Toxicol. 2022 May 25;17(1):11. doi: 10.1186/s12995-022-00352-4. J Occup Med Toxicol. 2022. PMID: 35614505 Free PMC article.
-
Infodemia: Another Enemy for Romanian Frontline Healthcare Workers to Fight during the COVID-19 Outbreak.Medicina (Kaunas). 2020 Dec 9;56(12):679. doi: 10.3390/medicina56120679. Medicina (Kaunas). 2020. PMID: 33317190 Free PMC article.
-
High levels of psychosocial distress among Australian frontline healthcare workers during the COVID-19 pandemic: a cross-sectional survey.Gen Psychiatr. 2021 Sep 6;34(5):e100577. doi: 10.1136/gpsych-2021-100577. eCollection 2021. Gen Psychiatr. 2021. PMID: 34514332 Free PMC article.
-
Psychological and mental health impacts of COVID-19 pandemic on healthcare workers in China: A review.World J Psychiatry. 2021 Jul 19;11(7):337-346. doi: 10.5498/wjp.v11.i7.337. eCollection 2021 Jul 19. World J Psychiatry. 2021. PMID: 34327126 Free PMC article. Review.
-
Addressing the psychological impact of COVID-19 on healthcare workers: learning from a systematic review of early interventions for frontline responders.BMJ Open. 2021 May 21;11(5):e044134. doi: 10.1136/bmjopen-2020-044134. BMJ Open. 2021. PMID: 34020974 Free PMC article.
Cited by
-
Neural Correlates of Burnout Syndrome Based on Electroencephalography (EEG)-A Mechanistic Review and Discussion of Burnout Syndrome Cognitive Bias Theory.J Clin Med. 2025 Jul 29;14(15):5357. doi: 10.3390/jcm14155357. J Clin Med. 2025. PMID: 40806977 Free PMC article. Review.
-
Cumulative lifetime stressor exposure impairs stimulus-response but not contextual learning.Sci Rep. 2024 Jun 7;14(1):13080. doi: 10.1038/s41598-024-62595-x. Sci Rep. 2024. PMID: 38844465 Free PMC article.
-
Neuroimaging insights into the psychosocial impact of the COVID-19 pandemic: a systematic review.Transl Psychiatry. 2025 Jul 10;15(1):236. doi: 10.1038/s41398-025-03423-2. Transl Psychiatry. 2025. PMID: 40640180 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Miscellaneous

