Effect of Preoperative MRI Coracoid Dimensions on Postoperative Outcomes of Latarjet Treatment for Anterior Shoulder Instability
- PMID: 35923867
- PMCID: PMC9340370
- DOI: 10.1177/23259671221083967
Effect of Preoperative MRI Coracoid Dimensions on Postoperative Outcomes of Latarjet Treatment for Anterior Shoulder Instability
Abstract
Background: Preoperative coracoid dimensions may affect the size of the bone graft transferred to the glenoid rim and thus the postoperative outcomes of Latarjet coracoid transfer.
Purpose: To determine the effect of coracoid length and width as measured on preoperative magnetic resonance imaging (MRI) on outcomes after Latarjet treatment of anterior shoulder instability.
Study design: Cohort study; Level of evidence, 3.
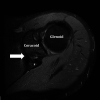
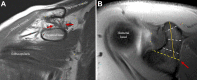
Methods: Included were patients who underwent primary Latarjet surgery between 2009 and 2019 and had preoperative MRI scans and minimum 2-year postoperative outcomes. Longitudinal coracoid length was measured on axial MRI sequences as the distance from the coracoclavicular ligament insertion to the distal tip. Comparisons were made between shorter and longer coracoids and between narrower and wider coracoids. The outcomes of interest were recurrent instability, reoperation, complications, return to sport (RTS), and American Shoulder and Elbow Surgeons (ASES) score. Independent-samples t test, Mann-Whitney test, chi-square test, and Fisher exact test were used to compare outcomes between groups, and univariate correlation coefficients were calculated to evaluate the relationships between demographics and coracoid dimensions.
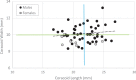
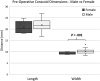
Results: Overall, 56 patients were included (mean age, 28.4 years). The mean ± SD coracoid length was 21.6 ± 2.4 mm and width 10.0 ± 1.0 mm. Relative to patients with a longer coracoid (≥22 mm; n = 26), patients with a shorter coracoid (<22 mm; n = 30) had similar rates of recurrent instability (shorter vs longer; 6.7% vs 3.8%), complications (10.0% vs 15.4%), reoperation (3.3% vs 7.7%), and RTS (76.5% vs 58.8%) and similar postoperative ASES scores (85.0 vs 81.6) (P ≥ .05 for all). Likewise, relative to patients with a wider coracoid (≥10 mm; n = 27), patients with a narrower coracoid (<10 mm; n = 29) had similar prevalences of recurrent instability (narrower vs wider; 6.9% vs 3.7%), complications (17.2% vs 7.4%), reoperation (3.5% vs 7.4%), and RTS (66.7% vs 68.4%) and similar postoperative ASES scores (87.1 vs 80.0) (P ≥ .05 for all).
Conclusion: Patients undergoing Latarjet coracoid transfer had similar postoperative outcomes regardless of preoperative coracoid dimensions. These findings should be confirmed in a larger cohort before further clinical recommendations are made.
Keywords: Latarjet; MRI; coracoid; instability; shoulder.
© The Author(s) 2022.
Conflict of interest statement
One or more of the authors has declared the following potential conflict of interest or source of funding: K.B.F. has received education payments from Liberty Surgical, consulting fees from DePuy/Medical Device Business Services, and speaking fees and honoraria from Vericel. M.E.B. has received grant funding from Arthrex, education payments from Arthrex and Smith & Nephew, and hospitality payments from Smith & Nephew. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Figures
Similar articles
-
Management of the Failed Latarjet Procedure: Outcomes of Revision Surgery With Fresh Distal Tibial Allograft.Am J Sports Med. 2019 Oct;47(12):2795-2802. doi: 10.1177/0363546519871896. Epub 2019 Sep 9. Am J Sports Med. 2019. PMID: 31498688
-
Clinical and Anatomic Predictors of Outcomes After the Latarjet Procedure for the Treatment of Anterior Glenohumeral Instability With Combined Glenoid and Humeral Bone Defects.Am J Sports Med. 2016 Jun;44(6):1407-16. doi: 10.1177/0363546516634089. Epub 2016 Mar 29. Am J Sports Med. 2016. PMID: 27217523
-
Outcomes of Latarjet Versus Distal Tibia Allograft for Anterior Shoulder Instability Repair: A Matched Cohort Analysis.Am J Sports Med. 2018 Apr;46(5):1030-1038. doi: 10.1177/0363546517744203. Epub 2018 Feb 1. Am J Sports Med. 2018. PMID: 29389219
-
Outcomes of the Latarjet Procedure Versus Free Bone Block Procedures for Anterior Shoulder Instability: A Systematic Review and Meta-analysis.Am J Sports Med. 2021 Mar;49(3):805-816. doi: 10.1177/0363546520925833. Epub 2020 Aug 14. Am J Sports Med. 2021. PMID: 32795174
-
Return to Sport After Coracoid Transfer in Athletes With Anterior Shoulder Instability: A Systematic Review.Sports Health. 2019 Sep/Oct;11(5):402-408. doi: 10.1177/1941738119853825. Epub 2019 Jul 3. Sports Health. 2019. PMID: 31268851 Free PMC article.
Cited by
-
3D MRI PD-SPACE-COR Predicting Safety Margin for Coracoid Transfer.Orthop Surg. 2023 Jun;15(6):1514-1520. doi: 10.1111/os.13719. Epub 2023 Apr 24. Orthop Surg. 2023. PMID: 37092459 Free PMC article.
-
Comprehensive analysis of bony scapula morphology and anthropometry in a homogeneous population.BMC Med Imaging. 2025 Jul 2;25(1):262. doi: 10.1186/s12880-025-01793-z. BMC Med Imaging. 2025. PMID: 40604525 Free PMC article.
References
-
- An VVG, Sivakumar BS, Phan K, Trantalis J. A. systematic review and meta-analysis of clinical and patient-reported outcomes following two procedures for recurrent traumatic anterior instability of the shoulder: Latarjet procedure vs Bankart repair. J Shoulder Elbow Surg. 2016;25(5):853–863. doi:10.1016/j.jse.2015.11.001 - PubMed
-
- Biswas D, Bible JE, Bohan M, Simpson AK, Whang PG, Grauer JN. Radiation exposure from musculoskeletal computerized tomographic scans. J Bone Joint Surg Am. 2009;91(8):1882–1889. doi:10.2106/JBJS.H.01199 - PubMed
-
- Boone JL, Arciero RA. First-time anterior shoulder dislocations: has the standard changed? Br J Sports Med. 2010;44(5):355–360. doi:10.1136/bjsm.2009.062596 - PubMed
-
- Bradley Edwards T, Walch G. The Latarjet procedure for recurrent anterior shoulder instability: rationale and technique. Oper Tech Sports Med. 2002;10(1):25–32. doi:10.1053/otsm.2002.28776
LinkOut - more resources
Full Text Sources

