Duration of Acute Kidney Injury and In-Hospital Mortality in Elder Patients with Severe COVID-19: A Retrospective Cohort Study
- PMID: 35928914
- PMCID: PMC9345708
- DOI: 10.1155/2022/9929038
Duration of Acute Kidney Injury and In-Hospital Mortality in Elder Patients with Severe COVID-19: A Retrospective Cohort Study
Abstract
Background: Patients with severe coronavirus disease 2019 (COVID-19) who develop acute kidney injury (AKI) in the intensive care unit (ICU) have extremely high rates of mortality. This study evaluated the prognostic impact of AKI duration on in-hospital mortality in elder patients.
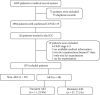
Methods: We performed a retrospective study of 126 patients with confirmed COVID-19 with severe or critical disease who treated in the ICU from February 4, 2020, to April 16, 2020. AKI was defined according to the Kidney Disease Improving Global Outcomes serum creatinine (Scr) criteria. AKI patients were divided into transient AKI and persistent AKI groups based on whether Scr level returned to baseline within 48 h post-AKI.
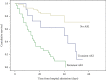
Results: In total, 107 patients were included in the final analysis. The mean age was 70 (64-78) years, and 69 (64.5%) patients were men. AKI occurred in 48 (44.9%) during their ICU stay. Of these, 11 (22.9%) had transient AKI, and 37 (77.9%) had persistent AKI. In-hospital mortality was 18.6% (n = 11) for patients without AKI, 72.7% (n = 8) for patients with transient AKI, and 86.5% (n = 32) for patients with persistent AKI (P < 0.001). Kaplan-Meier curve analysis revealed that patients with both transient AKI and persistent AKI had significantly higher death rates than those without AKI (log-rank P < 0.001). Multivariate Cox regression analysis revealed that transient and persistent AKI were an important risk factor for in-hospital mortality in older patients with severe COVID-19 even after adjustment for variables (hazard ratio [HR] = 2.582; 95% CI: 1.025-6.505; P = 0.044; and HR = 6.974; 95% CI: 3.334-14.588; P < 0.001).
Conclusions: AKI duration can be an important predictive parameter in elder patients suffering from COVID-19 and are admitted to ICU. Among these patients, those exhibiting persistent AKI have a lower in-hospital survival rate than those with transient AKI, emphasizing the importance of identifying an appropriate treatment window for early intervention.
Copyright © 2022 Yue Cai et al.
Conflict of interest statement
The authors declare that they have no competing interests.
Similar articles
-
Clinical Characteristics and Short-Term Outcomes of Acute Kidney Injury Missed Diagnosis in Older Patients with Severe COVID-19 in Intensive Care Unit.J Nutr Health Aging. 2021;25(4):492-500. doi: 10.1007/s12603-020-1550-x. J Nutr Health Aging. 2021. PMID: 33786567 Free PMC article.
-
[Stratified outcomes of "Kidney Disease: Improving Global Outcomes" serum creatinine criteria in critical ill patients: a secondary analysis of a multicenter prospective study].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2020 Mar;32(3):313-318. doi: 10.3760/cma.j.cn121430-20200218-00192. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2020. PMID: 32385995 Chinese.
-
Use of an extended KDIGO definition to diagnose acute kidney injury in patients with COVID-19: A multinational study using the ISARIC-WHO clinical characterisation protocol.PLoS Med. 2022 Apr 20;19(4):e1003969. doi: 10.1371/journal.pmed.1003969. eCollection 2022 Apr. PLoS Med. 2022. PMID: 35442972 Free PMC article.
-
Acute kidney injury is associated with severe infection and fatality in patients with COVID-19: A systematic review and meta-analysis of 40 studies and 24,527 patients.Pharmacol Res. 2020 Nov;161:105107. doi: 10.1016/j.phrs.2020.105107. Epub 2020 Jul 31. Pharmacol Res. 2020. PMID: 32739424 Free PMC article.
-
Acute kidney injury in patients with COVID-19 compared to those with influenza: a systematic review and meta-analysis.Front Med (Lausanne). 2023 Sep 19;10:1252990. doi: 10.3389/fmed.2023.1252990. eCollection 2023. Front Med (Lausanne). 2023. PMID: 37795409 Free PMC article.
Cited by
-
Acute Kidney Injury in the Context of COVID-19: An Analysis in Hospitalized Mexican Patients.Infect Dis Rep. 2024 May 16;16(3):458-471. doi: 10.3390/idr16030034. Infect Dis Rep. 2024. PMID: 38804444 Free PMC article.
-
Global geographic and socioeconomic disparities in COVID-associated acute kidney injury: a systematic review and meta-analysis.J Glob Health. 2025 Jul 25;15:04166. doi: 10.7189/jogh.15.04166. J Glob Health. 2025. PMID: 40709582 Free PMC article.
References
-
- Daneshkhah A., Agrawal V., Eshein A., Subramanian H., Roy H. K., Backman V. Evidence for possible association of vitamin D status with cytokine storm and unregulated inflammation in COVID-19 patients. Aging Clinical and Experimental Research . 2020;32(10):2141–2158. doi: 10.1007/s40520-020-01677-y. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous