Poor treatment responses were related to poor outcomes in pediatric B cell acute lymphoblastic leukemia with KMT2A rearrangements
- PMID: 35933338
- PMCID: PMC9357304
- DOI: 10.1186/s12885-022-09804-w
Poor treatment responses were related to poor outcomes in pediatric B cell acute lymphoblastic leukemia with KMT2A rearrangements
Abstract
Background: The KMT2A gene, formerly named the MLL gene, is rearranged (KMT2Ar) in 70-75% of infants, 5-6% of children and 10-15% of adult patients with B cell acute lymphoblastic leukemia (B-ALL). The outcome after chemotherapy of pediatric cases remains poor, and only a few studies have investigated the clinical and laboratory features, treatment response and prognosis in Chinese populations.
Methods: A total of 48 B-ALL children with KMT2Ar were enrolled in the study, and clinical and laboratory data were collected and analyzed by age group. The relationship between prognosis and traditional risk factors and treatment response was investigated for these patients who received chemotherapy.
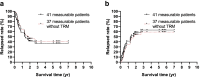
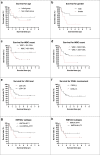
Results: The 48 enrolled patients included 28 males and 20 females; 18 (37.50%) or 30 (62.50%) patients were an age of < 12 m (infant B-ALL) or of > 12 m at onset. An initial WBC count of 300 × 109/L was detected in 7 (14.58%) patients; testicular leukemia (TL) or central nervous system involvement was found in 5 (10.41%) or 3 (6.25%) patients, respectively. Statistical differences were not found in the age groups of sex or initial WBC count, whereas TL was more common in the infant group (P < 0.05). 11q23 was detected in 18 patients; KMT2Ar was detected in 46 (95.83%) or 45 (93.75%) patients by FISH or multiplex RT-PCR technology, respectively; RNA-seq data were obtained for 18 patients, and 3 patients with uncommon KMT2Ar were identified. KMT2A-AFF1, KMT2A-MLLT3 and KMT2A-MLLT1 were the most common transcripts. Statistical differences were not found in treatment response by age groups, including dexamethasone induction, bone marrow (BM) smear status and minimal residual disease (MRD) level at different time points (TP), treatment-related mortality (TRM), or complete remission (CR) rate (P > 0.05); MRD levels monitored by FCM or PCR were unequal at the same TP. Four patients died of treatment, and TRM was 8.33%; 40 patients achieved CR, and the CR rate for the cohort was 83.33%. Seven patients quit, 15 patients relapsed, and the 5 yr cumulative relapse rate was 59.16 ± 9.16%; the 5 yr prospective EFS (pEFS) for patients who were included or excluded from the TRM group was 36.86 ± 8.48% or 40.84 ± 9.16%, respectively. Multivariate analysis for prognosis and hazard ratio was performed for 37 patients without TRM and revealed that an initial WBC count of > 300 × 109/L and a positive level of FCM-MRD were strongly related to a poor outcome for B-ALL patients with KMT2Ar (P < 0.05).
Keywords: B cell acute lymphoblastic leukemia; KMT2A rearrangement; Minimal residual disease; Pediatric; Prognosis; Treatment response.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- Agraz-Doblas A, Bueno C, Bashford-Rogers R, Roy A, Schneider P, Bardini M, Ballerini P, Cazzaniga G, Moreno T, Revilla C, Gut M, Valsecchi MG, Roberts I, Pieters R, De Lorenzo P, Varela I, Menendez P, Stam RW. Unraveling the cellular origin and clinical prognostic markers of infant B-cell acute lymphoblastic leukemia using genome-wide analysis. Haematologica. 2019;104(6):1176–1188. doi: 10.3324/haematol.2018.206375. - DOI - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources