The association of coagulation and atrial fibrillation: a systematic review and meta-analysis
- PMID: 35942591
- PMCID: PMC9907526
- DOI: 10.1093/europace/euac130
The association of coagulation and atrial fibrillation: a systematic review and meta-analysis
Abstract
Aims: While atrial fibrillation (AF) is suggested to induce a prothrombotic state, increasing thrombotic risk, it is also hypothesized that coagulation underlies AF onset. However, conclusive evidence is lacking. With this systematic review and meta-analysis, we aimed to summarize and combine the evidence on the associations between coagulation factors with AF in both longitudinal and cross-sectional studies.
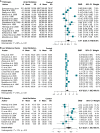
Methods and results: We systematically searched for longitudinal cohort and cross-sectional studies investigating AF and thrombosis. For longitudinal studies, pooled hazard ratios (HRs) and 95% confidence intervals (CIs) were calculated. For cross-sectional studies, we determined pooled standardized mean differences (SMDs) and 95% CIs. A total of 17 longitudinal and 44 cross-sectional studies were included. In longitudinal studies, we found significant associations between fibrinogen (HR 1.05, 95% CI 1.00-1.10), plasminogen activator inhibitor 1 (PAI-1) (HR 1.06, 95% CI 1.00-1.12), and D-dimer (HR 1.10, 95% CI 1.02-1.19) and AF incidence. In cross-sectional studies, we found significantly increased levels of fibrinogen (SMD 0.47, 95% CI 0.20-0,74), von Willebrand factor (SMD 0.96, 95% CI 0.28-1.66), P-selectin (SMD 0.31, 95% CI 0.08-0.54), ß-thromboglobulin (SMD 0.82, 95% CI 0.61-1.04), Platelet Factor 4 (SMD 0.42, 95% CI 0.12-0.7), PAI-1 (1.73, 95% CI 0.26-3.19), and D-dimer (SMD 1.74, 95% CI 0.36-3.11) in AF patients, as opposed to controls.
Conclusion: These findings suggest that higher levels of coagulation factors are associated with prevalent and incident AF. These associations are most pronounced with prevalent AF in cross-sectional studies. Limited evidence from longitudinal studies suggests a prothrombotic state underlying AF development.
Keywords: Atrial fibrillation; Coagulation; Haemostasis; Meta-analysis; Tachyarrhythmia; Thrombosis.
© The Author(s) 2022. Published by Oxford University Press on behalf of the European Society of Cardiology.
Conflict of interest statement
Conflicts of interest: All authors declare no conflict of interest.
Figures




References
-
- Heeringa J, van der Kuip DA, Hofman A, Kors JA, van Herpen G, Stricker BHet al. Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam study. Eur Heart J 2006;27:949–53. - PubMed
-
- Meyre P, Blum S, Berger S, Aeschbacher S, Schoepfer H, Briel Met al. Risk of hospital admissions in patients with atrial fibrillation: a systematic review and meta-analysis. Can J Cardiol 2019;35:1332–43. - PubMed
-
- Hindricks G, Potpara T, Dagres N, Arbelo E, Bax JJ, Blomstrom-Lundqvist Cet al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): the Task Force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Eur Heart J 2021;42:373–498. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

