Psychologic Impact of Chronic Orofacial Pain: A Critical Review
- PMID: 35943323
- PMCID: PMC10586586
- DOI: 10.11607/ofph.3010
Psychologic Impact of Chronic Orofacial Pain: A Critical Review
Abstract
Aims: To explore the prevalence of clinically significant anxiety and depression in adult patients with chronic orofacial pain (COFP) conditions.
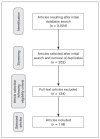
Methods: A systematic online search of the Medline (PubMed) and Ovid databases was performed for articles published from 2006 to 2019. Observational studies- including cross-sectional, case-control, and case series-and longitudinal prospective studies were included. A total of 118 articles were selected for inclusion, and the prevalence rates of clinically significant anxiety and depression were summarized.
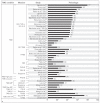
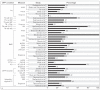
Results: Most studies focused on temporomandibular disorder (TMD) pain and less often on neuropathic COFP conditions. Prevalence rates varied widely across studies according to OFP condition and assessment measure; most questionnaire-based assessments yielded rates of clinically significant depression and anxiety in, respectively, 40% to 60% and 40% to 65% of individuals with TMD and in 20% to 50% and 25% to 55% of patients with neuropathic, mixed, or idiopathic/atypical COFP conditions. Rates of anxiety and depression were lower in studies using diagnostic instruments and in TMD studies with nonpatient samples. Most controlled studies showed a higher prevalence of anxiety and depression in individuals with COFP than in those without. Higher COFP pain levels and the presence of comorbid conditions such as migraines or widespread pain increased the likelihood of anxiety and/or depressive symptoms in individuals.
Conclusion: Clinically significant anxiety and depression were commonly observed in patients with COFP, were present at higher rates than in pain-free participants in controlled studies, and were closely linked to pain severity. More research is needed to evaluate the psychologic impact of multiple COFP conditions in an individual and the prevalence of precondition psychologic morbidity.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


References
-
- International Classification of Orofacial Pain, ed 1. Cephalalgia. 2020;40:129–221. - PubMed
-
- IASP. Pain terms. In: Merskey H, Bogduk N, editors. Classification of Chronic Pain: Descriptions of Chronic Pain Syndromes and Definitions of Pain Terms. ed 2. Seattle: IASP; 1994.
-
- Macrae WA. Chronic post-surgical pain: 10 years on. Br J Anaesth. 2008;101:77–86. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

