Paraspinal musculature impairment is associated with spinopelvic and spinal malalignment in patients undergoing lumbar fusion surgery
- PMID: 35944826
- PMCID: PMC10623672
- DOI: 10.1016/j.spinee.2022.07.103
Paraspinal musculature impairment is associated with spinopelvic and spinal malalignment in patients undergoing lumbar fusion surgery
Abstract
Background context: The concept of sagittal spinal malalignment is well established in spinal surgery. However, the effect of musculature on its development has not been fully considered and the position of the pelvis is mostly seen as compensatory and not necessarily a possible cause of sagittal imbalance.
Purpose: This study aimed to investigate the influence of the posterior paraspinal muscles (PPM, erector spinae, and multifidus) and the psoas muscle on spinopelvic and spinal alignment.
Study design/setting: Retrospective cross-sectional study.
Patient sample: Patients undergoing posterior lumbar fusion between 2014 and 2021 for degenerative conditions at a tertiary care center, with preoperative lumbar magnetic resonance imaging (MRI) within 12 months prior the surgery and a preoperative whole spine radiograph were included.
Outcome measures: PPM and psoas muscle measurements including the cross-sectional area (CSA), the functional cross-sectional area (fCSA), the amount of intramuscular fat (FAT), and the percentage of fat infiltration (FI). Spinopelvic measurements including lumbar lordosis (LL), pelvic tilt (PT), sacral slope (SS), pelvic incidence (PI), and sagittal vertical axis (SVA).
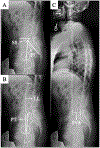
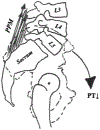
Methods: A T2-weighted MRI-based quantitative assessment of the CSA, the fCSA and the amount FAT was conducted, and FI was further calculated. The regions of interest included the psoas muscle and the PPM on both sides at the L4 level that were summarized and normalized by the patient's height (cm2/m2). LL, PT, SS, PI, and SVA were determined on standing lateral radiographs. Spearman correlation was used to calculate the crude relationship between spinopelvic and muscle parameters. Multiple linear regression models with age, sex, LL, PT, SS, and SVA set as independent variables were established to determine the association with spinal muscle outcome measures.
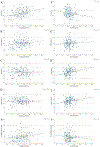
Results: A total of 150 patients (53.3% female) were included in the final analysis with a median age of 65.6 years and a median BMI of 28.2 kg/m2. Significant positive correlations were observed between PT (ρ=0.327), SVA (ρ=0.256) and PI (ρ=0.202) and the FIPPM. Significant negative correlations were detected for the PT and the fCSAPPM (ρ=-0.202) and PT and the fCSAPsoas (ρ=-0.191). Furthermore, a negative correlation was seen for PI and SVA and FIPsoas. PT (β=0.187; p=.006), SVA (β=0.155; p=.035), age (β=0.468; p<.001) and sex (β=0.235; p<.001) significantly predict FIPPM (corrected R2=0.393) as independent variables.
Conclusions: This study demonstrated the potential role of posterior paraspinal muscles and psoas muscle on pelvic retroversion and elucidated the relation to sagittal spinal malalignment. Although we cannot establish causality, we propose that increasing FIPPM, representing loss of muscular strength, may lead to increased pelvic retroversion and thus might be the initiating point for the development of the sagittal imbalance. These findings might challenge the well-known theory of increased pelvic retroversion being a compensatory mechanism for sagittal spinal balance. Thus, muscular weakness might be a factor involved in the development of sagittal spinal malalignment.
Keywords: Aging; Connective tissue; Fat infiltration; Muscle; Muscle quality; Pelvic tilt; Sagittal imbalance; Sagittal vertical axis; Sarcopenia; Spinal fusion; Spine.
Copyright © 2022 Elsevier Inc. All rights reserved.
Conflict of interest statement
Declarations of competing interests The Authors declare that there is no conflict of interest regarding this work.
Figures

Similar articles
-
Association patterns between lumbar paraspinal muscles and sagittal malalignment in preoperative patients undergoing lumbar three-column osteotomy.Spine Deform. 2024 May;12(3):801-809. doi: 10.1007/s43390-024-00828-9. Epub 2024 Mar 12. Spine Deform. 2024. PMID: 38472693
-
Differences in lumbar paraspinal muscle morphology in patients with sagittal malalignment undergoing posterior lumbar fusion surgery.Eur Spine J. 2022 Nov;31(11):3109-3118. doi: 10.1007/s00586-022-07351-3. Epub 2022 Aug 29. Eur Spine J. 2022. PMID: 36038784 Free PMC article.
-
Fat infiltration of the posterior paraspinal muscles is inversely associated with the fat infiltration of the psoas muscle: a potential compensatory mechanism in the lumbar spine.BMC Musculoskelet Disord. 2023 Oct 27;24(1):846. doi: 10.1186/s12891-023-06967-w. BMC Musculoskelet Disord. 2023. PMID: 37891498 Free PMC article.
-
Association of paraspinal muscle morphology or composition with sagittal spinopelvic alignment: a systematic review and meta-analysis.BMC Musculoskelet Disord. 2025 Aug 12;26(1):777. doi: 10.1186/s12891-025-09047-3. BMC Musculoskelet Disord. 2025. PMID: 40797242 Free PMC article.
-
ALIF in the correction of spinal sagittal misalignment. A systematic review of literature.Eur Spine J. 2021 Jan;30(1):50-62. doi: 10.1007/s00586-020-06598-y. Epub 2020 Sep 15. Eur Spine J. 2021. PMID: 32930843
Cited by
-
Relationship between posterior paraspinal muscle fat infiltration and early conversion to lumbar spinal fusion following decompression surgery.Eur Spine J. 2025 Jul;34(7):3031-3037. doi: 10.1007/s00586-025-09030-5. Epub 2025 Jun 13. Eur Spine J. 2025. PMID: 40514565
-
The association between paraspinal muscle parameters and vertebral pedicle microstructure in patients undergoing lumbar fusion surgery.Int Orthop. 2023 Apr;47(4):1051-1060. doi: 10.1007/s00264-022-05659-9. Epub 2022 Dec 23. Int Orthop. 2023. PMID: 36562815 Free PMC article.
-
Association between lumbar intervertebral vacuum phenomenon severity and posterior paraspinal muscle atrophy in patients undergoing spine surgery.Eur Spine J. 2024 Mar;33(3):1013-1020. doi: 10.1007/s00586-023-08120-6. Epub 2024 Jan 24. Eur Spine J. 2024. PMID: 38267734
-
Sarcopenia and the management of spinal disease in the elderly.Geroscience. 2025 Apr;47(2):1471-1484. doi: 10.1007/s11357-024-01300-2. Epub 2024 Aug 14. Geroscience. 2025. PMID: 39138794 Free PMC article. Review.
-
Georg Schmorl Prize of the German Spine Society (DWG) 2023: the influence of sarcopenia and paraspinal muscle composition on patient-reported outcomes: a prospective investigation of lumbar spinal fusion patients with 12-month follow-up.Eur Spine J. 2024 May;33(5):1737-1746. doi: 10.1007/s00586-024-08268-9. Epub 2024 May 27. Eur Spine J. 2024. PMID: 38801435
References
-
- Brzeszczynski F, Brzeszczynska J, Duckworth AD, Murray IR, Simpson A, Hamilton DF. The effect of sarcopenia on outcomes following orthopaedic surgery: a systematic review. Bone Joint J 2022;104-B(3):321–30. - PubMed
-
- Visser M, Kritchevsky SB, Goodpaster BH, et al. Leg muscle mass and composition in relation to lower extremity performance in men and women aged 70 to 79: the health, aging and body composition study. J Am Geriatr Soc 2002;50(5):897–904. - PubMed
-
- Goodpaster BH, Park SW, Harris TB, et al. The loss of skeletal muscle strength, mass, and quality in older adults: the health, aging and body composition study. J Gerontol A Biol Sci Med Sci 2006;61(10):1059–64. - PubMed
-
- Goodpaster BH, Carlson CL, Visser M, et al. Attenuation of skeletal muscle and strength in the elderly: The Health ABC Study. J Appl Physiol (1985) 2001;90(6):2157–65. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

