Associations of Dynapenic Obesity and Sarcopenic Obesity with the Risk of Complications in COVID-19
- PMID: 35955411
- PMCID: PMC9368708
- DOI: 10.3390/ijms23158277
Associations of Dynapenic Obesity and Sarcopenic Obesity with the Risk of Complications in COVID-19
Abstract
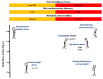
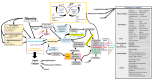
Ageing is associated with changes in body composition, such as low muscle mass (sarcopenia), decreased grip strength or physical function (dynapenia), and accumulation of fat mass. When the accumulation of fat mass synergistically accompanies low muscle mass or reduced grip strength, it results in sarcopenic obesity and dynapenic obesity, respectively. These types of obesity contribute to the increased risk of cardiovascular disease and mortality in the elderly, which could increase the damage caused by COVID-19. In this review, we associated factors that could generate a higher risk of COVID-19 complications in dynapenic obesity and sarcopenic obesity. For example, skeletal muscle regulates the expression of inflammatory cytokines and supports metabolic stress in pulmonary disease; hence, the presence of dynapenic obesity or sarcopenic obesity could be related to a poor prognosis in COVID-19 patients.
Keywords: COVID-19; ageing; complications; dynapenic obesity; sarcopenic obesity.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

Similar articles
-
Associations of Sarcopenic Obesity and Dynapenic Obesity with Bone Mineral Density and Incident Fractures Over 5-10 Years in Community-Dwelling Older Adults.Calcif Tissue Int. 2016 Jul;99(1):30-42. doi: 10.1007/s00223-016-0123-9. Epub 2016 Mar 4. Calcif Tissue Int. 2016. PMID: 26939775
-
Worsening Disability and Hospitalization Risk in Sarcopenic Obese and Dynapenic Abdominal Obese: A 5.5 Years Follow-Up Study in Elderly Men and Women.Front Endocrinol (Lausanne). 2020 Jun 30;11:314. doi: 10.3389/fendo.2020.00314. eCollection 2020. Front Endocrinol (Lausanne). 2020. PMID: 32695067 Free PMC article.
-
Obesity phenotypes are, in part, associated with physical activity in diabetic hemodialysis patients.Int Urol Nephrol. 2022 Jul;54(7):1751-1759. doi: 10.1007/s11255-021-03060-w. Epub 2021 Nov 23. Int Urol Nephrol. 2022. PMID: 34816362
-
Fall and Fracture Risk in Sarcopenia and Dynapenia With and Without Obesity: the Role of Lifestyle Interventions.Curr Osteoporos Rep. 2015 Aug;13(4):235-44. doi: 10.1007/s11914-015-0274-z. Curr Osteoporos Rep. 2015. PMID: 26040576 Review.
-
Health Consequences of Sarcopenic Obesity: A Narrative Review.Front Endocrinol (Lausanne). 2020 May 21;11:332. doi: 10.3389/fendo.2020.00332. eCollection 2020. Front Endocrinol (Lausanne). 2020. PMID: 32508753 Free PMC article. Review.
Cited by
-
Body Mass Index and Clinical Outcomes in Adult COVID-19 Patients of Diverse Ethnicities.Healthcare (Basel). 2022 Dec 19;10(12):2575. doi: 10.3390/healthcare10122575. Healthcare (Basel). 2022. PMID: 36554099 Free PMC article.
-
Association between dynapenic obesity phenotypes and physical performance in middle-age and older women living in community.Front Nutr. 2024 Sep 25;11:1480284. doi: 10.3389/fnut.2024.1480284. eCollection 2024. Front Nutr. 2024. PMID: 39385775 Free PMC article.
-
Sarcopenia, sarcopenic obesity and the clinical outcome of the older inpatients with COVID-19 infection: a prospective observational study.BMC Geriatr. 2024 Jul 4;24(1):578. doi: 10.1186/s12877-024-05177-w. BMC Geriatr. 2024. PMID: 38965468 Free PMC article.
-
Sleep duration affects the sequential change of body mass index and muscle strength: a contribution to dynapenic obesity.BMC Geriatr. 2023 May 12;23(1):288. doi: 10.1186/s12877-023-03857-7. BMC Geriatr. 2023. PMID: 37173647 Free PMC article.
-
Bridging the gap in obesity research: A consensus statement from the European Society for Clinical Investigation.Eur J Clin Invest. 2025 Aug;55(8):e70059. doi: 10.1111/eci.70059. Epub 2025 May 15. Eur J Clin Invest. 2025. PMID: 40371883 Free PMC article. Review.
References
-
- Mayoral L.P., Andrade G.M., Mayoral E.P., Huerta T.H., Canseco S.P., Rodal Canales F.J., Cabrera-Fuentes H.A., Cruz M.M., Pérez Santiago A.D., Alpuche J.J., et al. Obesity subtypes, related biomarkers & heterogeneity. Indian J. Med. Res. 2020;151:11–21. doi: 10.4103/ijmr.IJMR_1768_17. - DOI - PMC - PubMed
-
- Newman A.B., Kupelian V., Visser M., Simonsick E., Goodpaster B., Nevitt M., Kritchevsky S.B., Tylavsky F.A., Rubin S.M., Harris T.B., et al. Sarcopenia: Alternative definitions and associations with lower extremity function. J. Am. Geriatr. Soc. 2003;51:1602–1609. doi: 10.1046/j.1532-5415.2003.51534.x. - DOI - PubMed
-
- Kim Y.S., Lee Y., Chung Y.S., Lee D.J., Joo N.S., Hong D., Song G.E., Kim H.J., Choi Y.J., Kim K.M. Prevalence of sarcopenia and sarcopenic obesity in the Korean population based on the Fourth Korean National Health and Nutritional Examination Surveys. J. Gerontol. A Biol. Sci. Med. Sci. 2012;67:1107–1113. doi: 10.1093/gerona/gls071. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

