Therapeutic Vaccines for HPV-Associated Oropharyngeal and Cervical Cancer: The Next De-Intensification Strategy?
- PMID: 35955529
- PMCID: PMC9368783
- DOI: 10.3390/ijms23158395
Therapeutic Vaccines for HPV-Associated Oropharyngeal and Cervical Cancer: The Next De-Intensification Strategy?
Abstract
The rise in human papillomavirus (HPV)-associated oropharyngeal squamous cell carcinoma (OPSCC) has prompted a quest for further understanding of the role of high-risk HPV in tumor initiation and progression. Patients with HPV-positive OPSCC (HPV+ OPSCC) have better prognoses than their HPV-negative counterparts; however, current therapeutic strategies for HPV+ OPSCC are overly aggressive and leave patients with life-long sequalae and poor quality of life. This highlights a need for customized treatment. Several clinical trials of treatment de-intensification to reduce acute and late toxicity without compromising efficacy have been conducted. This article reviews the differences and similarities in the pathogenesis and progression of HPV-related OPSCC compared to cervical cancer, with emphasis on the role of prophylactic and therapeutic vaccines as a potential de-intensification treatment strategy. Overall, the future development of novel and effective therapeutic agents for HPV-associated head and neck tumors promises to meet the challenges posed by this growing epidemic.
Keywords: head and neck neoplasms; immune checkpoint inhibitors; immunization; intensity-modulated; papillomavirus infections; radiotherapy; vaccines.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
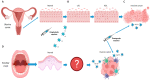
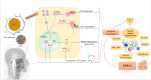
References
-
- Morand G.B., Diaconescu A., Ibrahim I., Lamarche G., Ruas J.S., Dalfen J., Hier M.P., Alaoui-Jamali M.A., Maschietto M., da Silva S.D. Molecular prognostic indicators in HPV-positive oropharyngeal cancer: An updated review. Clin. Exp. Metastasis. 2022;39:407–416. doi: 10.1007/s10585-022-10148-9. - DOI - PubMed
-
- Gillison M.L. Human Papillomavirus-Associated Head and NECK Cancer Is a Distinct Epidemiologic, Clinical, and Molecular Entity, Seminars in Oncology. Elsevier; Amsterdam, The Netherlands: 2004. pp. 744–754. - PubMed
-
- Ludwig R., Hoffmann J.M., Pouymayou B., Dappen M.B., Morand G.B., Guckenberger M., Gregoire V., Balermpas P., Unkelbach J. Detailed patient-individual reporting of lymph node involvement in oropharyngeal squamous cell carcinoma with an online interface. Radiother. Oncol. 2022;169:1–7. doi: 10.1016/j.radonc.2022.01.035. - DOI - PubMed

