MicroRNAs in Inflammatory Bowel Disease and Its Complications
- PMID: 35955886
- PMCID: PMC9369281
- DOI: 10.3390/ijms23158751
MicroRNAs in Inflammatory Bowel Disease and Its Complications
Abstract
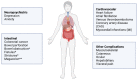
Inflammatory bowel disease (IBD), classified primarily between Crohn's disease and ulcerative colitis, is a collection of chronic gastrointestinal inflammatory conditions that cause multiple complications because of systemic alterations in the immune response. One major player is microRNA (miRNA), which is found to be associated with multiple pathways in mediating inflammation, especially those of a chronic nature in IBD, as well as irritable bowel syndrome. Although there have been studies linking miRNA alterations in IBD, even differentiating Crohn's disease and ulcerative colitis, this review focuses mainly on how miRNAs cause and mechanistically influence the pathologic complications of IBD. In addition to its role in the well-known progression towards colorectal cancer, we also emphasize how miRNA manifests the many extraintestinal complications in IBD such as cardiovascular diseases; neuropsychiatric conditions such as depression and anxiety disorders; and others, including various musculoskeletal, dermatologic, ocular, and hepatobiliary complications. We conclude through a description of its potential use in bettering diagnostics and the future treatment of IBD and its systemic symptoms.
Keywords: Crohn’s disease; colitis-associated cancer; extraintestinal manifestations; non-coding RNA; ulcerative colitis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
miRNA Molecules-Late Breaking Treatment for Inflammatory Bowel Diseases?Int J Mol Sci. 2023 Jan 23;24(3):2233. doi: 10.3390/ijms24032233. Int J Mol Sci. 2023. PMID: 36768556 Free PMC article. Review.
-
MicroRNAs as Innovative Biomarkers for Inflammatory Bowel Disease and Prediction of Colorectal Cancer.Int J Mol Sci. 2022 Jul 20;23(14):7991. doi: 10.3390/ijms23147991. Int J Mol Sci. 2022. PMID: 35887337 Free PMC article. Review.
-
Clinical presentation of Crohn's, ulcerative colitis, and indeterminate colitis: Symptoms, extraintestinal manifestations, and disease phenotypes.Semin Pediatr Surg. 2017 Dec;26(6):349-355. doi: 10.1053/j.sempedsurg.2017.10.003. Epub 2017 Oct 5. Semin Pediatr Surg. 2017. PMID: 29126502 Review.
-
Inflammatory bowel disease. Part I: Nature and pathogenesis.Dis Mon. 1991 Oct;37(10):605-66. doi: 10.1016/0011-5029(91)90024-6. Dis Mon. 1991. PMID: 1893828 Review.
-
Extraintestinal manifestations of inflammatory bowel disease.Minerva Gastroenterol Dietol. 2005 Jun;51(2):147-63. Minerva Gastroenterol Dietol. 2005. PMID: 15990704 Review.
Cited by
-
Updated immunomodulatory roles of gut flora and microRNAs in inflammatory bowel diseases.Clin Exp Med. 2023 Aug;23(4):1015-1031. doi: 10.1007/s10238-022-00935-9. Epub 2022 Nov 16. Clin Exp Med. 2023. PMID: 36385416 Free PMC article. Review.
-
Precision Medicine in Inflammatory Bowel Disease: A Spotlight on Emerging Molecular Biomarkers.Biomedicines. 2024 Jul 8;12(7):1520. doi: 10.3390/biomedicines12071520. Biomedicines. 2024. PMID: 39062093 Free PMC article. Review.
-
The role of miRNAs in the pathogenesis, diagnosis, and treatment of colorectal cancer and colitis-associated cancer.Clin Exp Med. 2025 Mar 16;25(1):86. doi: 10.1007/s10238-025-01582-6. Clin Exp Med. 2025. PMID: 40091000 Free PMC article. Review.
-
Blood miRNAs miR-549a, miR-552, and miR-592 serve as potential disease-specific panels to diagnose colorectal cancer.Heliyon. 2024 Mar 24;10(7):e28492. doi: 10.1016/j.heliyon.2024.e28492. eCollection 2024 Apr 15. Heliyon. 2024. PMID: 38571665 Free PMC article.
-
MicroRNA signatures in the pathogenesis and therapy of inflammatory bowel disease.Clin Exp Med. 2024 Sep 11;24(1):217. doi: 10.1007/s10238-024-01476-z. Clin Exp Med. 2024. PMID: 39259390 Free PMC article. Review.
References
-
- Kuenzig M.E., Fung S.G., Marderfeld L., Mak J.W.Y., Kaplan G.G., Ng S.C., Wilson D.C., Cameron F., Henderson P., Kotze P.G., et al. Twenty-first Century Trends in the Global Epidemiology of Pediatric-Onset Inflammatory Bowel Disease: Systematic Review. Gastroenterology. 2022;162:1147–1159.e4. doi: 10.1053/j.gastro.2021.12.282. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

