The role of neutrophil extracellular traps in acute lung injury
- PMID: 35967320
- PMCID: PMC9374003
- DOI: 10.3389/fimmu.2022.953195
The role of neutrophil extracellular traps in acute lung injury
Abstract
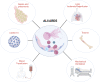
Acute lung injury (ALI) is a heterogeneous inflammatory condition associated with high morbidity and mortality. Neutrophils play a key role in the development of different forms of ALI, and the release of neutrophil extracellular traps (NETs) is emerging as a common pathogenic mechanism. NETs are essential in controlling pathogens, and their defective release or increased degradation leads to a higher risk of infection. However, NETs also contain several pro-inflammatory and cytotoxic molecules than can exacerbate thromboinflammation and lung tissue injury. To reduce NET-mediated lung damage and inflammation, DNase is frequently used in preclinical models of ALI due to its capability of digesting NET DNA scaffold. Moreover, recent advances in neutrophil biology led to the development of selective NET inhibitors, which also appear to reduce ALI in experimental models. Here we provide an overview of the role of NETs in different forms of ALI discussing existing gaps in our knowledge and novel therapeutic approaches to modulate their impact on lung injury.
Keywords: ALI (acute lung injury); ARDS (acute respiratory distress syndrome); COVID-19; DAMPs (damage-associated molecular patterns); NETs (neutrophil extracellular traps); Thromboinflammation; infections and sepsis; sterile inflammatory response.
Copyright © 2022 Scozzi, Liao, Krupnick, Kreisel and Gelman.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
-
- Kulkarni HS, Lee JS, Bastarache JA, Kuebler WM, Downey GP, Albaiceta GM, et al. Update on the features and measurements of experimental acute lung injury in animals: An official American thoracic society workshop report. Am J Respir Cell Mol Biol (2022) 66:e1–e14. doi: 10.1165/rcmb.2021-0531ST - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

