Obesity and Breast Cancer Metastasis across Genomic Subtypes
- PMID: 35973227
- PMCID: PMC9628732
- DOI: 10.1158/1055-9965.EPI-22-0013
Obesity and Breast Cancer Metastasis across Genomic Subtypes
Abstract
Background: Obese women have higher risk of aggressive breast tumors and distant metastasis. However, obesity has rarely been assessed in association with metastasis in diverse populations.
Methods: In the Carolina Breast Cancer Study Phase 3 (2008-2013), waist-to-hip ratio (WHR), body mass index (BMI), and molecular subtype [PAM50 risk-of-recurrence (ROR) score] were assessed. Obesity measures were evaluated in association with metastasis within five years of diagnosis, overall and stratified by race and ROR score. Absolute risk of metastasis and risk differences between strata were calculated using the Kaplan-Meier estimator, adjusted for age, grade, stage, race, and ER status. Relative frequency of metastatic site and multiplicity were estimated in association with obesity using generalized linear models.
Results: High-WHR was associated with higher risk of metastasis (5-year risk difference, RD, 4.3%; 95% confidence interval, 2.2-6.5). It was also associated with multiple metastases and metastases at all sites except brain. The 5-year risk of metastasis differed by race (11.2% and 6.9% in Black and non-Black, respectively) and ROR score (19.5% vs. 6.6% in high vs. low-to-intermediate ROR-PT). Non-Black women and those with low-to-intermediate ROR scores had similar risk in high- and low-WHR strata. However, among Black women and those with high ROR, risk of metastasis was elevated among high-WHR (RDBlack/non-Black = 4.6%, RDHigh/Low-Int = 3.1%). Patterns of metastasis were similar by BMI.
Conclusions: WHR is associated with metastatic risk, particularly among Black women and those with high-risk tumors.
Impact: Understanding how risk factors for metastasis interact may help in tailoring care plans and surveillance among patients with breast cancer.
©2022 American Association for Cancer Research.
Conflict of interest statement
Conflicts of interest:
The University of North Carolina, Chapel Hill has a license of intellectual property interest in GeneCentric Diagnostics and BioClassifier, LLC, which may be used in this study. The University of North Carolina, Chapel Hill may benefit from this interest that is/are related to this research. The terms of this arrangement have been reviewed and approved by the University of North Carolina, Chapel Hill Conflict of Interest Program in accordance with its conflict-of-interest policies.
Figures
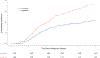


References
-
- Pajares B, Pollán M, Martín M, Mackey JR, Lluch A, Gavila J, et al. Obesity and survival in operable breast cancer patients treated with adjuvant anthracyclines and taxanes according to pathological subtypes: a pooled analysis. Breast Cancer Res. 2013;15(6):R105. doi:10.1186/bcr3572 - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

